Five Zone Acupuncture and Six Actions Herb Prescribing:
Countering the Adverse Effects of Cancer Chemotherapy
Offering traditional Chinese medicine (TCM) as an adjunct to modern cancer therapies, with the primary aim of countering the adverse effects of those modern therapies and secondarily to improve long-term outcomes, represents a relatively new application of TCM. Experience with this medical specialty at one of the Institute for Traditional Medicine facilities was outlined in my 2013 report Adjunct Cancer Therapy at the Immune Enhancement Project (IEP) Clinic (1). In that document, which focused attention on the acupuncture aspect of the therapeutic program, I referred to the five zones method and here elaborate that approach to acupuncture point selection (part I). The main focus of the remainder of the current paper is introducing what I refer to as Six Actions Herb Prescribing, relaying experience gained in China and at the IEP Clinic in relation to design of herb formulations for cancer patients (part II)+.
I. Wǔqū Fāngfǎ (五区方法): Five Zones Method
The five zones method reflects a practice of many acupuncturists that had not been formally described by acupuncturists. I presented this method, without giving it a name, in an article on mind/brain disorders produced in 2000 (2), saying: “In this article, the use of standard body acupuncture for mind and brain disorders is discussed. It will be seen that only a limited number of points, on just a few of the acupuncture channels, are repeatedly relied upon to treat a variety of these disorders. This may reflect the unique effectiveness of at least some of these acupuncture points which appear to be grouped around the head, forearms, and lower legs.” I then expanded upon these acupuncture treatment strategies in my book on treating shen [spirit] disorders (3), for which I mentioned this grouping of acupuncture points in both the acupuncture section and concluding remarks. I further pointed to this method in a brief update for the acupuncture section of that book published the following year (4), providing a more recent example of its use for treating depression in post-stroke patients. It was not until 2012 that I designated this point selection approach as the five zones method, having previously referred only to needling the “three parts of the body,” for which two parts have bilateral needling, hence, a total of five zones. The name for the method was publicly revealed in 2013 at the 25th Anniversary Pacific College Symposium. In giving this brief overview of the developments, I want to make clear that I did not devise the method I am describing, but reported on acupuncture point selections that were being widely used in modern TCM, and then gave a definition to the acupuncture formulations by noting the range of points utilized, and, finally, provided this designation. While the method has its greatest number of applications in treating mind/brain disorders, it is by no means limited to that area of therapy as will be described below.
The five zones include the bilateral “transportation districts,” from elbow to hand and from knee to foot, that incorporate the five types of peripheral transportation (shu) points: jing, ying, shu, jing he, translated as: well, spring, stream, river, sea, representing the gradually enlarging flow through the channels. With Wuqu Fangfa, the points to be needled within these zones need not be only the transportation points, but should normally include at least one bilateral pair of the transportation points for arms and one pair for legs in the total point set, examples being forearm points shenmen (HT-7), waiguan (TB-5), hegu (LI-4), quchi (LI-11), and lower leg points yinlingquan (SP-9), taichong (LV-3), taixi (KI-3), zusanli (ST-36). The combination of hegu (LI-4) and taichong (LV-3), known as siguan (four gates), is commonly selected to calm psychological and physical distress; as another example, shenmen (HT-7), taixi (KI-3) and zusanli (ST-36) are often chosen in the treatment of organic brain disorders.
With this method, points are also selected in the zone of head and back of the neck—the fifth zone—primarily along the centerline, the GV vessel ranging from dazhui (GV-14) through renzhong (GV-26; also called shuigou) and including the extra point yintang between GV-24 and GV-25. Starting at dazhui (GV-14), the back of the head points are selected for strengthening yang and for treating disorders that physically affect the brain. Reaching the top of the head, needling regulates the yang and alleviates disorders that affect the function of the brain, such as insomnia. Moving to the front of the head, treated points drain excess and calm agitation. Points along either side of the center line may be used additionally, such as sishencong (EX-HN-1), fengqi (GB-20), or anmian.
The inclusion of centerline head points with the more commonly selected points at all the extremities (bilateral upper and lower limbs) produces effects that are notable; I have described the effects as a “stabilizing pattern.” In essence, the four peripheral transportation zones help the clear yang to ascend to the head and the head points of the fifth zone help the yang to return to the lower body, so that the mind is calm and focused and the body has a more firm and controlled foundation.
Wuqu Fangfa does not preclude use of points at other locations of the body, but does require these five zones to be needled as a substantial portion of the treatment strategy. The most common additions for general use are the waist area points: at the front of the body from guanyuang (CV-4) to zhongwan (CV-12) and alongside this channel, such as tianshu (ST-25); and at the back from yaoyangguan (GV-3) to jizhong (GV-6), mainly relying on shu points of the adjacent bladder channel from dachangshu (BL-25) to pishu (BL-20), as well as points on the outer bladder channel of that region, such as zhishi (BL-52). When specific symptoms suggest use of points elsewhere, they are selected accordingly as secondary points. Ashi points and modern ear acupuncture points (which are not head points of Wuqu) might make another addition, but attention to the five zones should not be lost.
Because needling of these zones is often recommended by acupuncturists without making reference to the presence of a particular methodology as I am defining here, practitioners reading about the treatment of symptoms and diseases may not gain a valuable insight into this five zone strategy that can be purposefully employed. For example Dr. Li Zhang, trained at Beijing University of Chinese Medicine, described treatments for anxiety (5) with four syndrome categories using points that fit the Wuqu method. This table displays the recommended points, with head/neck, arm, and leg points separated into columns for easy visualization of the five zones.
Pattern |
Head/Neck |
Arms |
Legs |
Others |
Heart/Spleen Deficiency |
sishencong |
shaohai, shenmen, daling |
yinlingquan, fenglong, sanyinjiao |
danzhong, zhongwan, qihai |
Liver Qi Stagnation Affecting Spleen |
sishencong, yintang, taiyang |
waiguan, yemen |
yinlingquan, zusanli, ligou, taichong |
qimen, xuehai, daimai |
Kidney Qi Deficiency |
sishencong, yintang, shengting |
chize, neiguan |
jiaoxin, taixi, shenmai, kunlun |
guanyuan, zhongli |
Lung Qi Deficiency |
sishencong, yintang |
quchi, kongzui, lieque |
zusanli, xiajuxu, fenglong, neiting |
yutang |
The most frequent references to point selection consistent with the five zone method of therapy is to be found in the book Case Studies from the Medical Records of Leading Chinese Acupuncture Experts (6). Though the book was compiled in 2009 and published in 2011, it predominantly presents case reports from before the year 2000, some going back to the 1960s.
The advisor for this book and the largest contributor of case studies to its collection is a leading acupuncture professor, one of China’s designated “great masters of TCM,” Cheng Xinnong (1921-present). Even more so than the others whose cases were offered, he used the five zones treatment pattern frequently and for a diverse array of disorders.
 Cheng is best known internationally for his book Chinese Acupuncture and Moxibustion (7) chosen in China and the west as a college text for acupuncture studies. He noted that for the use of distal points (emphasis added): “Among the points of the fourteen meridians, those located on the limbs, especially below the elbow and knee joints, are effective not only for local disorders but also for disorders of the remote zang-fu organs and tissues on the course of their pertaining meridians.” In the collection of case studies, it is noted that: “The head is the place where all the yang channels meet, and clean yang qi of the six fu organs and the essence of the five zang organs all flow upward to it.” The conceptual framework for the five zone method is essentially laid out in these two statements, but the parts needed to be joined together: peripheral points from elbow to fingers and from knees to toes, and the points in the region of the head and neck.
Cheng is best known internationally for his book Chinese Acupuncture and Moxibustion (7) chosen in China and the west as a college text for acupuncture studies. He noted that for the use of distal points (emphasis added): “Among the points of the fourteen meridians, those located on the limbs, especially below the elbow and knee joints, are effective not only for local disorders but also for disorders of the remote zang-fu organs and tissues on the course of their pertaining meridians.” In the collection of case studies, it is noted that: “The head is the place where all the yang channels meet, and clean yang qi of the six fu organs and the essence of the five zang organs all flow upward to it.” The conceptual framework for the five zone method is essentially laid out in these two statements, but the parts needed to be joined together: peripheral points from elbow to fingers and from knees to toes, and the points in the region of the head and neck.
From an examination of published acupuncture strategies that do not incorporate the five zones, such as those that dominate the extensive list of recommendations in Therapeutics of Acupuncture and Moxibustion (8), it is evident that the forearm and lower leg points are often selected, but head points not included. The deficiency in choosing head points was a concern expressed by the developers of scalp acupuncture (9), who focused on what were designated as shu points on the scalp, placing particular reliance on the “zone” of central line of the governing vessel and adjacent to it. Scalp acupuncture was often accompanied by needling shu points on the extremities, such as quchi (LI-11), hegu (LI-4), waiguan (TB-5), neiguan (PC-6), sanyinjiao (SP-6), and taichong (LV-3) for stroke patients.
Needling the points of the governing channel removes obstruction in the flow of the yang qi and essence and thereby aids the return of these pure essences to the rest of the body, so that the head points will be important for treating symptoms that arise locally, such as headache, dizziness, facial paralysis, sinus congestion, and eye disorders, as well as for treating syndromes affecting the rest of the body, which may be due to dysfunctions of the brain (e.g., epilepsy, post-stroke, and restlessness) or because of disrupted circulation of qi, blood, and yang downward, as in acute lumbar pain due to invasion of wind.
The situations that may call for use of Wuqu Fangfa can be contrasted to those where other methods would be more appropriate. Although the outline presented here represents broad generalizations, the division illustrates that Wuqu Fangfa has many applications but is not a likely first choice for other medical concerns:
Indications for Five Zone Method |
Other Methods Usually More Appropriate |
Disorders affecting the head |
Localized disorders, but not the head or along GV vessel |
Dysfunctions, injuries, diseases of the brain |
Disorders affecting primarily the fu organs |
Emotional distress and mental imbalances |
Disorders that do not disturb the mental activities |
Peripheral nervous system dysfunction |
Endocrine dysfunction |
Disorders affecting several parts of the body |
Disorders primarily affecting a single zang organ |
Imbalances in yang qi circulation |
Imbalances of yin essence |
The “other methods” include simple needling with two or three points locally or, for more complex patterns, leaving out one area of the five defined zones: for example, no points of the head/neck zone, or no forearm points, or no lower leg points; there will usually be more attention to torso points. In the case of adverse effects of chemotherapy and radiation, because these medical interventions affect several parts of the body, cause an imbalance of yang qi circulation (often affecting appetite and sleep as a result), are accompanied by emotional distress, adversely alter brain activity (the condition sometimes referred to as “chemo brain”) and sometimes the peripheral nervous system (neuropathy), the five zone method fits well for this application.
For easy reference, I present here a summary of the five zones method as applies to the treatment of cancer patients at the IEP Clinic, relying on our foundational group of points, the new twenty needles and their associated points (1):
New Twenty Needles Points:
| zusanli (ST-36) | 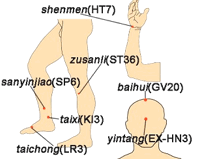 |
|
| sanyinjiao (SP-6) | ||
| taixi (KI-3) | Lower Limbs | |
| taichong (LV-3) | ||
| hegu (LI-4) | Upper Limbs | |
| quchi (LI-11) | ||
| neiguan (PC-6) | ||
| baihui (GV-20) | Head | |
| yintang (Ex-HN-3) | ||
| qihai (CV-6) | Torso | |
| zhongwan (CV-12) | ||
| tianshu (ST-25) |
Example of Five Zones Method
Common additions to the above set were the lower limb points yinlingquan (SP-9; substituted for SP-6 or added to it), zhaohai (KI-6; substituted for KI-3), qiuxu (GB-40); upper limb points shousanli (LI-10, frequent substitute for LI-11); shenmen (HT-7; substitute for PC-6 or added to it), lieque (LU-7), waiguan (TB-5); torso points jianjing (GB-21), danzhong (CV-17; also called shanzhong); and head/neck points shenting (GV-24; added to GV-20), fengchi (GB-20), and extra point anmian (near GB-20). In a few instances, two adjacent points on a meridian were needled at the same time, such as LI-10 and LI-11 or GB-20 and GB-21. For calming the disturbed spirit, some practitioners at IEP also add ear points.
II. Six Actions Herb Therapy
Introduction to the Reasons for Changing Herbal Strategies
The subject of counteracting adverse effects of cancer therapies with herbs has been approached by many Chinese physicians. The reason for offering this particular presentation about six actions is to raise the concern that the initial focal point for thinking about and addressing this problem may be inadequate, while remaining largely unchallenged. I am willing to make this suggestion because I have experienced other areas of Chinese medicine applied to modern medical concerns where the original way of analyzing the disorder relied too heavily on ancient concepts that were more suited to the experience with notably different disease conditions, even though symptoms were similar. There are instances where Chinese physicians have come to this same conclusion, so I am not treading upon entirely new territory.
As an example, multiple sclerosis is a disease that was relatively rare in earlier centuries (appearing in the late 19th century) and virtually non-existent in China until quite recently. One of its common manifestations is a progressive difficulty with moving the legs and feet, which then causes withering of the leg muscles because they are less used. These signs of the disease turned attention of modern TCM doctors to the ancient literature, as is the common method of determining how to proceed from the traditional-style pathology and therapeutics to the modern case. They sought formerly encountered diseases that caused weakening of the muscles, particularly of the legs, with withering of the muscle mass, a condition known as weizheng (flaccidity syndrome). The texts, starting with the preferred reference point, the Neijing Suwen, depicted a heat syndrome that caused damage through one or more of a number of possible mechanisms. The dominant thought was that heat so damaged the yin that it could no longer sustain the flesh, and the muscles would wither. Treatment strategies for such conditions—restoring yin and cleansing deficiency heat that remained after the initiating disorder—had been developed in ancient times and were then suggested by modern practitioners of TCM for patients with MS (10)
However, upon seeing numerous American MS patients at the IEP clinic, it became evident that neither a feverish disease nor other fire syndrome was associated with onset of MS, that yin deficiency was rarely seen as a predominant disease manifestation, and that yin nourishing herbs were of value but had only limited effect on the current status of the disability or its progression. By contrast, it was observed that stagnation syndromes were more prevalent.
Along similar lines, a Chinese physician, Cheng Yongde, who saw many patients with ALS, considered that the application of ancient doctrines was steering treatment in the wrong direction, working with one of the traditional views of weizheng. I wrote about his considerations in an article on ALS (11):
Cheng Yongde noted that in the past Chinese physicians mainly relied on the ancient doctrine of the Niejing Suwen (ca. 100 A.D.) in treating diseases where the muscles atrophy. The basic approach they take when encountering a disease that causes the muscles to weaken and atrophy is to direct treatment at enhancing the function of the stomach/spleen system, rooted in the concept that the spleen governs the muscles. By treating the associated meridians (e.g., yangming meridian), the muscles would be nourished and invigorated. Cheng believes, instead, that ALS is due to a blockage of the governing vessel, leaving it unable to regulate the qi and blood flowing to the viscera; then, the limbs are not adequately nourished by the flow of qi and blood. Therefore, using acupuncture to unblock the governing vessel is the key to therapy.
The lesson to be gained from these and other such examples is that when we encounter new disease conditions, the first analysis made through the process of applying standard TCM principles may need revision as experience and understanding of the new disorder grows; the determination serving as a starting point may represent only one aspect of the disease process, possibly not the central one Even if some success is attained initially, it may be only a partial result compared to what is potentially to be achieved. I chose these two examples because they represent cases where tonification therapies—to replenish damaged yin on the one hand, and to restore function of the spleen and its generation of qi and blood to nourish the muscles on the other—did not quite fit the patient presentations.
In the case of countering the side-effects of chemotherapy and radiation, the early clinical work on this subject was done in China at a time when there were only a few chemotherapy drugs and when radiation beams were quite crudely applied (the beam was relatively wide and could only be approximately aimed at the internal mass). The effects of treatment were drastic and were also largely uncontrolled by any of the palliative medications that were available. Of particular note was the frequent occurrence of oral ulcerations and skin irritation from chemotherapy and substantial burning of the skin (and everything in the path) of the radiation beam. It is not surprising, then, that in an English language publication based on this early work (12) it was reported that “According to Traditional Chinese Medicine, radiation and chemotherapy are regarded as an extrinsic external stimulus which manifest in the form of heated toxin. It invades the body as an external evil damaging and destroying the normal physiology….”
At the outset, each particular manifestation of this destructive effect was treated by modifications of well-known traditional formulas, thus, for example: a modified Xuanfuhua Daizheshi Tang (Inula and Hematite Combination) for treating nausea and vomiting; a modified Guipi Tang (Ginseng and Longan Combination) for low blood counts; or modified Baitouweng Tang (Pulsatilla Combination) for burning and inflammation affecting the bowels. However, not long afterward it was realized that one could address the fundamental impact of the medical treatments by relying on a basic formula suited to most patients that might then be modified if necessary to address the most severe manifestations in the individual. Such modification would either be attained by adding herbs for the specific concern or by providing a second formulation to address the condition.
The dominant treatment method for countering side effects of cancer chemotherapy has been tonification, and this comes in response to the evident debility caused by the interventions and the apparent inability of some organs to function, such as the spleen (in relation to the digestive system disturbances) and the kidney (in relation to the blood system deficiencies). Defensive activity would be impaired (as revealed by serious infections) and the hair would fall out (indicating blood deficiency). Because of the interpretation that “heat toxin” damaged the yin and substantially weakened the spleen, nourishing yin (with moistening herbs like maimendong and herbs that benefit the hair, like nüzhenzi) and tonifying qi (with herbs that bolster weiqi, such as huangqi, and that protect spleen functions, with soothing herbs like qianshi and shanyao) became the prominent methods.
By examining formulas that the modern TCM doctors were prescribing for their patients, certain herbs drew the attention of laboratory researchers. For example huangqi (astragalus) and nüzhenzi (ligustrum) were announced as being beneficial for cancer patients at a 1983 Chinese conference (MD Anderson Cancer Center in Houston cosponsored the Chinese conference and provide the site for research on these two herbs). A pair of related publications suggested that each of these herbs could have the effect of restoring immune functions in the patients, as illustrated by study of blood drawn from them and compared to that from a control group of non-cancer patients.
While there is no doubt that cancer patients undergoing modern medical therapies suffer from deficiency syndromes, some of the modern drugs give less evidence of heat toxin and yin deficiency than was seen in the past. The circumstances surrounding cancer diagnosis and treatment as well as physiological effects of cancer treatment also point to the presence of stagnation syndromes, not just deficiency. The presence of stagnation was originally observed only in passing, for example that radiation and chemotherapy causes (12, emphasis added): “imbalance of yin and yang, obstruction of the circulation of qi and blood, disturbance of the function of the organs…” In one of the most extensive texts about providing herbal support for cancer patients undergoing chemotherapy (13), a section was devoted to the problem of blood stasis, indicating its importance. Nonetheless, little further commentary was provided throughout the rest of the book and the formulas routinely incorporated only one herb, jixueteng (millettia) that might have been classified as being used for this purpose. Therefore, the emphasis and aim of this article will be to make a broader analysis of the situation and suggest a more comprehensive way of treatment.
Why Six Actions?
Since ancient times, scholars of Chinese medicine have frequently presented their medical concepts, diagnostics, and therapeutics by enumeration of a small number of divisions: three essences, four diagnostic methods, five elements, six climatic factors, seven emotional factors, eight types of herbal therapy. When establishing these defined categories in order to concisely sum up the complexities of nature and of human health and disease and to provide an easy reference for memorization and description, subtle gradations—complex and intermediate conditions—could become lost. Such losses are particularly acute during a student’s study of these classifications, because a novice can easily accept the simplicity they convey as being not so much a useful tool for interchange of information and ideas, but a profound key to an absolute reality of nature. The important subtleties that are not immediately obvious from the classification systems can be brought back into the discussion, and especially so when describing multiple therapeutic actions of an individual herbs or particular circumstances that affect a patient. Still, it is necessary to intentionally and sometimes laboriously pursue the actual complexities rather than taking the easier path of turning to the few restrictive categories. Otherwise the fallback route of black and white divisions will overshadow reality, clouding observations and limiting effective actions.
When it comes to herbal therapies, the most fundamental influence driving the original development of its categories was—and remains—the concept of yin and yang. In the Advanced Textbook on Traditional Chinese Medicine and Pharmacology (14), where the early history of Chinese medicine theories is being reviewed and brought forward to the modern times, it is noted that:
In the final analysis, a disease is the result of a breakdown in the equilibrium of the body’s yin and yang….Thus, a cardinal principle of treatment is to reconcile the two aspects….just as Basic Questions says, “The yin and yang should be carefully observed and adjusted.” ….Since the theory of yin/yang underlies the differentiation of syndromes, all pathological changes may be summarized as disturbances of yin and yang. Any disorders of the exterior and interior, of descending and ascending of qi, all syndromes of heat and cold, excess and deficiency, any disharmony between the ying and wei systems, and all disturbances of the qi and blood, are expressions of the disharmony between yin and yang. Broadly speaking, the following treatment methods are used to balance yin and yang: relieving exterior syndromes and eliminating interior syndromes; sending up the lucid yang and bringing down wastes; clearing away the heat and warming the cold; reinforcing the deficient in deficiency syndromes and reducing the excess is excess syndromes; harmonizing the nutrient and defensive systems; and adjusting the qi and blood.
This last listing of methods provides subdivisions of yin and yang that depict paired opposites of bodily conditions, such as deficiency and excess; cold and heat; internal causation and external causation of disorders; internal manifestation and external manifestation of symptoms and signs. This set of four pairs gave rise to the standard “eight methods [strategies] of therapy” used in herbalism. The eight features of an ailment to be addressed by herbs were elucidated by Gou Congshi in the Bencao Yanyi, published around 1119 A.D. He provided some fairly limiting category descriptions, which point to the general principles involved allowing for broader applications, writing that (15):
There are eight important points in the treatment of illness...The first is deficiency, signified by the five signs: fine pulse, cold skin, shortness of breath, polyuria and diarrhea, low appetite for food and drink. The second is excess, this is signified by the five signs: full pulse, hot skin, bloated abdomen, urinary retention and constipation, depression. The third is cold, that is, cold in the internal organs [zangfu]. The fourth is heat, that is, heat in the internal organs. The fifth is superficial evil, signifying that the disease did not originate with a disturbance of the normal qi in the organs. The sixth is internal evil, that is, the illness did not arise from external causes. The seventh is interior; this signifies that the disease is not located in the body surface [skin and muscles]. The eighth is the exterior; this signifies that the illness is not located in the interior portion of the body [internal organs, bones].
And, the basic yin/yang division later yielded the three other pairs: “sending up the lucid yang and bringing down wastes; harmonizing the nutrient and defensive systems; and adjusting the qi and blood.”
As the systematic application of herbology grew more complex over the subsequent centuries, the number of categories of treatment also grew so that in most modern listings of herbs the various medicinal materials are divided into about two dozen standard categories. In addition to the above mentioned categories there are such groupings as herbs to: resolve phlegm, sedate internal wind, open the orifices, sedate the spirit, and astringe discharge.
The number six frequently has been used in Chinese medicine categorization, such as the six environmental influences, the six disease stages (of the Shanghan Lun), and the six pairs of zang and fu (with five sets corresponding to the five elements, and the fire element divided into two). It is not a matter of six being a magical number to which the medical scholars tried to fit many of their concepts, rather, it is a number of categories that is sufficiently large to account for many phenomena, yet small enough that the divisions can be remembered and worked with. As will become evident, the six actions herb therapy comprise about the largest number of therapeutic effects that can be utilized at once without formulations becoming diffuse and cumbersome.
The “Six Actions Herb Prescribing” that is described here does not represent a proposal for a new categorization of the herb actions; rather, these are strategies selected as a particular subset of the roughly two dozen groupings routinely used in modern TCM. To incorporate the important herbs into these groups, some adjustments are made as to how a few of the herbs might be best categorized for the current purpose. As an example, chaihu (bupleurum) is categorized in modern Materia Medica with the herbs for resolving the surface (the cooling subgroup), but this herb is probably more often used in regulating the flow of qi—influencing the liver’s controlling mechanism and helping to raise clear qi—so it is placed in what follows with qi regulating herbs. The six actions chosen for inclusion here are contained within the yin/yang summary that was given in the Advanced Textbook (14) as quoted above, with a focus on “adjusting qi and blood.” The six actions come from expansion of the pairing of qi and blood, namely: qi and blood to be nourished; qi and blood to be circulated; clear qi to be raised up to the brain; and blood to be generated from marrow (the brain and marrow being two extensions of the kidney organ system).
My selection of these therapeutic approaches was arrived at through recognition that the actions are both theoretically of benefit in countering the side effects of chemotherapy for cancer and they are being utilized frequently at the IEP Clinic because practitioners are seeing these as appropriate to the cancer patients. Experience at IEP is of potential value because the circumstances in China differed from those encountered here and the changes in modern medical treatment are progressing rapidly with new drugs, new drug delivery methods, and improved palliative care. In contrast to the continued reliance on tonification therapy relayed in modern literature, it is proposed here that all six action of herbs are likely of value in treating cancer patients and that most of them should be combined into a single treatment, either within a single formulation, or through the combining of two or more base formulas. This article will focus attention on chemotherapy, but the principles of treatment for countering adverse effects of radiation therapy are quite similar.
An Orientation to Chemotherapy
The term chemotherapy could be applied to any drug; the term was originally utilized by the German chemist Paul Ehrlich when he was working on drugs to treat infections: he coined it for any use of chemicals (chemo-) given to treat disease (therapy). In the realm of cancer treatment, chemotherapy is most often used to describe drugs that directly inhibit the reproduction of cancer cells (e.g., 5-FU, taxol, platinum drugs), but it can also be used to depict other strategies, such as drugs that block estrogens from stimulating cancer cells (e.g. Tamoxifen, Aromatase Inhibitors), which typically involve a notably different (and often milder) set of adverse reactions. The subject of concern in this article is the former group of drugs that powerfully inhibit the metabolism and reproduction of cancer cells, often leading to cell death (apoptosis). A characteristic of their common side effect profiles is that they tend to also inhibit the metabolic activity and reproduction of other non-cancer cells, having particularly strong impact on rapidly reproducing cells. Chemotherapy drugs are selected, developed, and approved for use by virtue of their specificity for inhibiting cancer cells, yet none of the current widely used agents are sufficiently specific that they don’t produce to a lesser extent the same type of inhibitory impact on non-cancer cells. Inhibitory effects include bone marrow suppression, impaired turn-over of gastro-intestinal cells, and reduced mitochondrial activity. While active cancer cells (those that are reproducing) will die as a result of the treatment, with shrinking of tumor masses, non-cancer cells are more likely to be functionally inhibited but with relatively limited die-off, so that recovery of their functions can take place during the days after treatment is withdrawn. Sometimes adverse effects will persist, especially in the case of neurological damage to peripheral nerves, but for most patients the production of blood cells and intestinal cells returns to normal or near normal.
TCM Interpretation of Chemotherapy Adverse Effects
In the early development of Chinese medicine some herbs were suggested to have the capability to counteract toxicity of plant drugs, and I reviewed these in the introduction to the subject of countering side effects of modern drug therapies (16). The best known of the group is licorice, and there are two prominent sets of herb materials that are related to it: 1) those from the same family as licorice (Leguminosae) also used for this purpose, including shandougen (Sophora subprostrata), baibiandou (dolichos), dandouchi (soja; processed soybeans), and chixiaodou (phaseolus); and 2) very sweet tasting items, such as dazao (jujube) and fengmi (honey). Eating legumes (beans, Chinese: dou) as part of the diet for cancer patients is best for getting an adequate dose of these food-herbs for this counter-toxicity approach, rather than adding ingredients to already complex herb formulas, but shandougen, though attributed some sweet taste, is predominantly very bitter, so this ingredient or its concentrated extract, would be used in formulations that could be swallowed directly without tasting (e.g., tablet).
The primary approach to chemotherapy adverse effects requires an analysis of the bodily imbalances that are to be rectified. From the TCM perspective, the ability of the body to regenerate day to day is primarily a function of the qi and blood and so the inhibition of cellular reproduction by chemotherapy points to imposed deficiencies of qi and blood. The Advanced Textbook (14) lists five functions of qi, designated as: promoting, warming, defensive, controlling, and activity. Qi and blood function as a pair, and in virtually all the ancient medical literature of China, the phrase “qi and blood” was the basis for what we today often simply depict as qi. The nature and role of blood in TCM is somewhat less clearly defined than qi, but one of the Neijing Suwen quotations is often utilized to give a sense of the function of blood: “When the liver receives blood, the vision is normal; when the feet receive blood, they are able to walk; when the palms receive blood, they are able to hold things; and when the fingers receive blood, they are able to grasp.”
Once the first dose or two of chemotherapy works its way through the populations of existing cells to impact their activity and reproduction (about ten days), the physical changes come on very rapidly. From the first day of obvious symptoms, their severity increase day by day, either until a plateau is reached or some corrective measures are put in place, with palliative drugs, for example. This rapid change in the body’s ability to promote its replenishment, control its functions, and be active in transformation of food essences, with lethargy as one of the signs of the drug actions illustrates the impairment of qi and blood. The defensive action of qi is today interpreted in terms of immune responses, so herbs that tonify qi and herbs that are said to enhance immune responses may be gathered together under the same grouping.
Below is presented a table of herbs that tonify qi, adding to the standard list eleuthero and gynostemma and medicinal mushrooms (a few of which are described in a separate table); additionally, two antitoxin herbs that were used in China as anticancer medicinals but are now often designated as functioning through immune enhancing activity are included in a separate table in this section.
Herbs that Tonify Qi
Common Name, |
Additional Properties |
Comments |
Astragalus huangqi Astragalus membranaceus |
increases and raises clear qi and yang, controls sweating |
Frequently used for persons debilitated by disease with weakened immune functions, poor digestion, and spontaneous sweating. |
Atractylodes baizhu Atractylodes macrocephala |
dries dampness, harmonizes stomach and spleen |
Especially used in cases of weakened digestion and diarrhea and for those who easily get infections. |
Codonopsis dangshen Codonopsis pilosula |
increases fluids |
Frequently used as a substitute for ginseng; it lacks the yang invigorating action. |
Eleuthero ciwujia Eleutherococcus senticosus |
benefits kidney; warm |
Developed as health product in Russia during 1970s, adopted by China for same use, as a ginseng-substitute. |
Medicinal Mushroom*
|
benefits lungs, sweet |
In modern times, these herbs are increasingly used for immune-enhancing properties. |
Ginseng renshen Panax ginseng |
tonifies kidney and lung, pacifies spirit, invigorates, raises yang |
Useful in virtually all deficiency syndromes; especially used with spirit agitation. |
Gynostemma jiaogulan Gynostemma pentaphyllum |
benefits lung; cool |
A Chinese folk remedy for lung diseases, popularized in the 1990s, after it was found to contain some active ingredients of ginseng. |
Jujube dazao (or hongzao) Zizyphus jujuba |
pacifies spirit, harmonizes actions of herbs, protects stomach |
Used as an aid to reduce harshness, protect the stomach, and harmonize the action of ingredients. |
Licorice gancao Glycyrrhiza uralensis |
moistens lungs, harmonizes actions of herbs, counters toxicity |
Often prepared by honey-frying to enhance tonic effects; used in small amounts in numerous formulas to harmonize ingredients. |
*Examples of Mushrooms used to Boost Immune Functions
Cordyceps dongchongxiacao Cordyceps sinensis |
controls cough and dyspnea |
Mainly used for chronic asthma associated with kidney deficiency; recently adopted as immune enhancing agent. |
Coriolus yunzhi Coriolus versicolor |
dispels moisture; warm |
Developed as a source of immune-enhancing polysaccharides in Japan during 1970s, adopted by China for same purpose. |
Ganoderma* lingzhi Ganoderma lucidum |
nourishes all internal organs, removes toxin, vitalizes blood |
Designated as a sedative, this herb is mainly used now for immune-enhancing and blood-circulating properties. |
Anti-Toxin Herbs that Enhance Immune Functions
Common Name, Pinyin, Sources |
Additional or Dominant Properties |
Comments |
Oldenlandia baihuasheshecao Oldenlandia diffusa |
antitumor effects |
Modern applications are mainly for cancer patients; it is an herb of low toxicity with reputation for inhibiting tumor growth. |
Scutellaria banzhilian Scutellaria barbata |
antitumor effects |
Modern applications of this herb are as an addition to oldenlandia in the treatment of tumors. |
Herbs that Nourish Blood
Tang-kuei danggui Angelica sinensis |
vitalizes blood, moves qi, moistens intestines, regulates menstruation |
This is the most widely used blood nourishing herb. |
Lycium gouqizi Lycium barbarum |
nourishes yin, aids vision, benefits marrow |
Especially used for the combination of kidney- and liver-deficiency syndrome and for eye disorders. |
Peony (white peony) baishao Paeonia alba |
cools blood, vitalizes blood, astringes liver yin, alleviates spasms and pain |
Peony is extensively used for a variety of applications; red peony (chishao) is used when blood vitalizing is the main concern. |
Ho-shou-wu heshouwu Polygonum multiflorum |
nourishes yin |
Ho-shou-wu is mostly used when there is kidney and liver deficiency; it is almost always used in formulas for the hair. |
Rehmannia shou dihuang Rehmannia glutinosa |
nourishes yin, benefits marrow |
Extensively used in cases of kidney deficiency, and almost always used when for kidney/liver deficiency. |
Smoothing the Flow of Qi, Enlivening the Circulation of Blood
Deficiency of qi will itself cause some disturbance in the flow of qi through the body. However, a substantial impact on the quality of qi circulation comes from emotional distress that is in this case associated with cancer diagnosis and response to the difficult experience of medical treatments that often become increasingly traumatic. In the book Prevention and Treatment of Carcinoma with Traditional Chinese Medicine (17), it is noted that:
The mental state of the patient plays an important role in the course of treatment….Generally speaking, cancer patients are in low spirits and full of worries….Vexation, hesitation, grief, fear, nervousness, depression and low spirit should be relieved so as to prevent poor appetite.
While the author believed that the mental state of the patient would be addressed primarily by the actions and words of family, friends, and medical staff, these conditions persist to a certain extent and influence the body. As one major consequence, qi circulation can stagnate, thus worsening drug-induced fatigue, lowering appetite, and altering ability to make decisions.
Further, while qi deficiency is a reasonable means of representing what happens to the person as a result of the chemotherapy impact on cellular activities, the transporting action of the spleen and the qi smoothing action of the liver are also inhibited by chemotherapy, so that there is a direct effect on qi circulation that requires attention.
Both qi deficiency and disturbances in qi circulation impair the free flowing of blood, as does the decline in physical activity that results from fatigue. In the book Cancer Treatment with Fu Zheng Pei Ben Principle by Pan Mingji (13), Pan indicates that blood stasis is a problem even before cancer is diagnosed, before any treatment with surgery, chemotherapy, or radiation. He says:
TCM believes the mechanism of cancer is related to blood stasis….The fact that cancer patients reveal a state of hyper-coagulation has been gradually accepted….90% of cancer cases reveal, by fingertip volume pulse wave and microcirculation of the nail fold, that arterial capillaries are spasmodic and narrow, with decreased or even missing capillary loops. Some may reveal blood corpuscle congestion and blood flow is intermittently interrupted.
Tissue damage due to surgery or radiation therapy will cause more severe blood stasis in the affected area. With regard to chemotherapy, Pan notes that blood vitalizing herbs are important to the comprehensive treatment, including the long-term success of the medical therapies:
Usually, the side effects of chemotherapy can be greatly ameliorated when coordinated with Fu Zheng Pei Ben prescriptions and [herbs] which activate blood circulation and relieve blood stasis, thereby also increasing the blood flowing in cancer tissue. It is very helpful when the concentration of chemicals, immune remedies, and immune lymphocytes increase in the cancer tissues, as the therapeutic effect is then also greatly increased.
Along similar lines, it is thought that the impact of radiation therapy is improved by vitalizing blood circulation, because one of the mechanisms of radiation is to introduce high concentrations of reactive (ionized) oxygen to kill the cancer cells, such that if the cells are at the same time better able to get oxygen from the blood the effect will be enhanced. Additionally, quick access of immune substances from the blood will help kill the damaged cells and break them down. Pan referred to this in a later text (18), saying:
The main function of this medicine [herbs for removing blood stasis] is to ameliorate damage to microcirculation and add to the flow of blood and oxygen in tumor tissue. It is desirable to bring the anticarcinogen [drug] into the tumor to help the chemotherapy drugs. One of the reasons why radiotherapy fails is the lack of oxygen in cancer cells. The medicine for removing blood stasis can increase the quantity of oxygen in cancer cell and heighten their sensitivity to radiation.
Limited circulation reduces the ability of the severely damaged cancer cells to die, while good circulation may help the less damaged normal cells recover more quickly. The concern for improving circulation to tumor cells differs from efforts to halt tumor-stimulated growth of a circulatory system for a tumor mass, for which the drugs that inhibit the generation of new vessels (angiogenesis inhibitors) are directed. The tumor needs a blood supply to survive at all, but it is able to utilize a restricted one quite effectively and especially the restrictions prevent cancer treatments from having their full effects.
Western practitioners of Chinese medicine raised the concern that activating blood circulation might promote metastasis of cancer cells. However, metastasis in many cancers is a normal process that is very difficult to alter, and the Chinese concept is that the primary cause for concern is not the temporary circulation of the cells, but the adherence of them to other tissues, an adherence that is needed to allow for new tumor growth. The herbs used for promoting blood circulation are understood to reduce this adherence and thus inhibit metastatic growths from occurring.
While the formerly mentioned methods of tonify qi and nourishing blood are a good means of improving qi circulation, additional efforts may be needed. Below are some of the herbs classified as regulating qi, with a separated section to display the large number of ingredients that are various types of citrus fruits. It is important to note, however, that herbs in other categories may also regulate qi as a secondary property, such as chuanxiong (cnidium), so that one can formulate concisely by relying on those ingredients.
Herbs that Regulate Qi
Common Name, Pinyin, Sources |
Additional or Dominant Properties |
Comments |
Areca seed binglangzi Areca catechu |
dispels moisture accumulation, breaks up accumulations |
Primarily used for abdominal swelling associated with water accumulation. Areca peel (dafupi) is sometimes used instead. |
Bupleurum chaihu Bupleurum chinense |
raises yang qi, resolves surface, cooling |
Used for dredging qi from liver constraint; especially valued for disorders that combine internal syndromes with external syndromes. |
Citrus Group (see separate table) |
resolves phlegm-damp |
Several members of the citrus family are used to regulate qi; they are grouped together in a table displaying some of their slight differences. |
Cyperus xiangfuzi Cyperus rotundus |
alleviates pain, regulates menstruation |
Analgesic for headaches and abdominal pains and alleviates stagnation-caused menstrual irregularities; overcomes mild depression. |
Lindera wuyao Lindera strychnifolia |
alleviates pain, warms the kidney |
Mainly used for lower abdominal pain associated with cold kidney; has properties similar to cinnamon twig (guizhi). |
Melia chuanlianzi Melia toosendan |
alleviates pain |
Mainly used for pain in the chest and upper abdomen (liver area). |
Saussurea muxiang Saussurea lappa or Jurinea souliei |
alleviates pain, controls diarrhea, sedative |
Used for mainly for abdominal disorders that include diarrhea. |
Citrus Group of Qi Regulating Herbs
Common Name, Pinyin, Sources |
Additional or Dominant Properties |
Comments |
Chih-ko zhiqiao Citrus aurantium |
resolves phlegm, disperses accumulations |
Used for food stagnancy, epigastric aching, and lung congestion. |
Chih-shih zhishi Citrus aurantium |
purges gallbladder to produce mild laxative effect, clears heat and phlegm |
Used for abdominal stagnation with constipation and for lung congestion. |
Blue citrus qingpi Citrus reticulata |
resolves phlegm |
Mainly used for lung disorders with phlegm accumulation and for dispersing soft swellings. |
Citrus chenpi Citrus noblis |
strengthens spleen, dries moisture and phlegm |
The most widely used qi-regulating herb; it is also used in treatment of most phlegm disorders, combined with pinellia. |
Aurantium jupi Citrus reticulata |
lowers up-rushing qi, relieves stagnation in the chest |
Used for nausea, vomiting, hiccough, and coughing. |
Fu-shou fushougan Citrus medica |
alleviates pain, controls vomiting |
Used for digestive distress with abdominal pain and distention. |
 |
The herbs that vitalize blood circulation are emphasized as important by TCM cancer specialists but often do not appear in the formulations, with the primary exception of jixueteng (millettia or spatholobus, see illustration below, the stem is used). This herb is chosen because of its dual use for nourishing and vitalizing blood circulation; it came into the cancer adjunct formulas early on and has been retained. |
Herbs that VITALIZE BLOOD
Common Name, Pinyin, Sources |
Additional or Dominant Properties |
Comments |
Carthamus honghua Carthamus tinctorius |
regulates menstruation, alleviates pain of injuries |
Combined with persica in treatments of blood stasis causing pain. |
Cnidium chuanxiong Ligusticum chuanxiong |
dispels wind, regulates qi, controls pain, nourishes blood |
It is the main herb used for headache pain; used in most formulas for qi and blood staganation and in many formulas for nourishing blood. |
Corydalis yanhusuo Corydalis ambigua |
controls pain, regulates qi |
Mainly used for abdominal pain syndromes, including menstrual pain. |
Curcuma yujin Curcuma aromatica |
regulates qi, disperses accumulations |
Mainly used in cases of qi and blood stagnation with accumulation, including treatment of phlegm masses and other lumps. |
Millettia jixueteng Spatholobus suberectus |
nourishes blood, alleviates numbness, relaxes tendons |
Modern applications are mainly for anemia and promoting microcirculation; traditionally used for numbness of the legs in the elderly. |
Myrrh moyao Commiphora sp. |
controls pain, disperses swellings, promotes tissue regeneration |
Used mainly for injuries (along with frankincense, ruxiang) and for swellings, such as abscesses. |
Frankincense (or mastic) ruxiang Boswellia carterii |
controls pain, relaxes muscles, reduces bleeding |
Mainly used in treatment of injuries, usually combined with myrrh (moyao), considered useful for peripheral neuropathy. |
Red peony chishao Paeonia obovata |
clears heat, cools blood |
Especially used for blood stasis syndrome with blood heat. |
Persica taoren Prunus persica |
moistens the intestines |
Often used for abdominal blood stasis accompanied by constipation; combined with carthamus (honghua) for blood stasis disorders. |
Salvia danshen Salvia miltiorrhiza |
cools blood, nourishes blood, sedative |
Primarily used for cardiovascular disorders and for liver fibrosis; also useful as a sedative. |
Sparganium (or Scirpus) sanleng Sparganium stoloniferum |
regulates qi, disperses mass |
Mainly used for hard masses (blood stasis type), especially those in the abdomen; usually combined with Zedoaria (ezhu). |
Vaccaria wangbuliuxing Vaccaria pramidata |
regulates menstruation, disperses swelling |
Primarily used for swelling in the lower abdomen, particularly for women’s disorders. |
Zedoaria ezhu Curcuma zedoaria |
regulates qi, disperses mass, benefits stomach functions |
Mainly used for hard masses, in combination with Sparganium (sanleng); also for digestive disturbance with distention. |
Raising Clear Qi and Yang
Raising of clear qi primarily refers to extracting the nutritive essences from food and raising them to the upper body so that they can then be distributed (by lung and heart) to all the organs. Raising of the clear yang refers mainly to bringing both nutrients and yang qi to the head so that the brain and mind can function properly; the yang will then be distributed downward from the top of the body. However, the references to raising clear (“lucid”) qi and yang are not firmly distinguished and depending on the author and the emphasis placed on the different functions, these terms may be used interchangeably and so it is perhaps best to refer to them together as an entity.
In the book Essentials of Chinese Medicine (19), there is this explanation of raising of the clear:
This is a characteristic function of the spleen, and refers to both raising clear qi upward and stabilizing the internal organs in their original locations [i.e., counteracting prolapse].
Controlling the raising up of the Clear: Here, the “clear” means the nutrients that are extracted from drink and food, and raising the clear means propelling them upward and distributing them. After food and drink have been digested by the stomach, the spleen extracts the nutrients and, though its function of raising the clear, delivers them upward to the heart and lung, and thence to the entire body.
If this function of the spleen is normal, all the internal viscera and tissues will obtain enough nutrients and function well. If it is abnormal, there may appear such symptoms as dizziness, blurred vision, and fatigue. If clear yang fails to ascend, the clear and the turbid may remain intermixed and sink downward. This may be manifested by such symptoms as spermatorrhea, vaginal discharge, abdominal distention, and diarrhea.
The separation of clear and turbid is an important subdivision of the raising of the clear; “intermixing” of clear and turbid, when their separation is incomplete, can lead to a variety of abdominal problems and discharges from the lower body. In his essay, Heaven Above, Earth Below, Cheng Lok-Kwan provides this elucidation (20):
The distinction between clear yang and turbid yin is very important in Chinese medicine. Turbid means thick, or dense. Turbid does not mean dirty or bad. The head is heaven: it is the highest part of the body. It is the most yang part of the body, hence, it should be filled with clear yang. If it is, the brain and senses will function well. The person will be able to perceive the world and communicate clearly, and respond appropriately. If it is not, then we think either a blockage prevented the clear yang from rising, or that the body is unable to descend the turbid yin. Either way, the head is now filled with turbid yin. The senses will be clouded, the head will feel heavy, and the person will not be able to think or speak clearly.
Here, the concept of raising clear yang is associated with bringing nourishment (which is as aspect of the qi) to the brain. For raising clear qi and yang, the primary principle is to strengthen the spleen, particularly with herbs that contribute an upward movement, so that huangqi (astragalus) and renshen (ginseng) are key items. However, to assure separation of clear and turbid, herbs that promote the digestive functions of the stomach are utilized: they help to generate a clear qi and to aid the downward movement to the “thick” digestive materials. Of greatest importance are shenqu (shen-chu), maiya (malt), and jineijin (gallus) and the aromatic herbs sharen (cardamom), muxiang (saussurea), and yizhiren (alpinia). To help make sure the channels of flow are clear and open, orifice opening herbs are used, such as shichangpu (acorus) and yuanzhi (polygala). As an adjunct to these different types of herbs, those that help filter excess dampness are utilized: they improve spleen function, aid the separation of clear and turbid, and promote fluid movement to the kidney system. The primary ingredients relied upon are baizhu (atractylodes) and fuling (hoelen). Some herbs were already described in the tables above.
Additional Herbs to Help Raising Clear Qi and Yang
Common Name, |
Additional or Dominant Properties |
Comments |
Acorus shichangpu Acorus gramineus |
sedative, warms meridians, invigorates digestion |
This is the most widely used herb for orifice opening; it is included in many sedative formulas and has a mild action. |
Alpinia yizhiren Alpinia oxyphylla |
supplements spleen, strengthens stomach |
Mainly used for abdominal pain due to cold; also for poor appetite; action is similar to cardamom (sharen). |
Cardamom sharen Amomum villosum |
alleviates stagnation of food |
Alleviates stomach pain, loss of appetite, nausea, diarrhea, and fullness after eating. |
Crataegus shanzha Crataegus pinnatifida |
helps digestion of meat and fats, resolves phlegm |
This herb has modern uses of promoting blood circulation; traditionally used to promote digestion of thick foods. |
Gallus jineijin Chicken gizzard lining |
controls diarrhea |
This material is thought to help break down masses and is used in treatment of concretions (stones) and tumors. |
Hoelen (or Poria) fuling Poria cocos |
strengthens spleen, calms spirit |
The most widely used herb for filtering fluids, it is very mild yet highly effective, especially in decoction form. |
Malt maiya Hordeum vulgare |
regulates qi |
Used as a mild agent to harmonize liver and spleen, regulating the flow of qi while promoting the stomach’s digestive function. |
Shen-chu shenqu Medicated wheat |
strengthens spleen, controls diarrhea, resolves surface congestion |
This is the most widely used digestive aid; it is also suited to treatment of acute ailments, such as summer heat syndrome. |
Oryza guya Oryza sativa |
harmonizes stomach and spleen, strengthens spleen |
Sprouted rice is used as a tonic and also a stomach protectant when administering fire-purging herbs, such as gypsum (shigao). |
Polygala yuanzhi Polygala tenuifolia |
resolves phlegm |
Often selected for insomnia, poor memory, and confusion associated with “phlegm mist affecting the heart orifices.” |
Benefitting the Marrow
One of the cell lines highly sensitive to the effects of chemotherapy and radiation are the stem cells that produce red and white blood cells and platelets (thrombocytes) located in the marrow. The decline in production of new blood cells is one of the major reasons for halting a chemotherapy sequence, because of increased susceptibility to infection (as a result of low WBC) and debilitating fatigue (result of low RBC). Some protection of the marrow function is attained by utilizing hormones that stimulate the production of blood cells (e.g., Epogen and Neupogen); it is anticipated that some protective action can be attained with herbs such as lurong (deer antler), shudi (rehmannia), and gouqizi) lycium fruit.
While the marrow of Chinese medicine has this overlapping connection to the marrow we understand by modern medicine that produces these blood cell lines, the marrow of Chinese medicine also extends to the brain. Therefore, nourishing the marrow along with raising the pure qi and yang, is important in maintaining good cognitive function, memory, and mental focus, according to the Chinese medicine system. Some of the herbs for benefiting marrow were already included in descriptions of blood nourishing herbs.
Additional Herbs for Benefiting Marrow
Common Name, |
Additional or Dominant Properties |
Comments |
Deer antler lurong Cervus nippon |
nourishes blood, invigorates yang |
Frequently used in cases of weakness with a combination of yin, yang, and blood deficiency; the gelatin nourishes blood. |
Cistanche roucongrong Cistanche salsa |
moistens intestines |
Mostly used for impotence and infertility; useful in cases of constipation due to abdominal cold and blood deficiency. |
Cuscuta tusizi Cuscuta chinensis |
astringent, clears vision |
Widely used in kidney-tonic formulas due to its mild nature. Used in eye formulas based on treating kidney/liver deficiency. |
Dipsacus xuduan Dipsacus asper |
vitalizes blood |
Mainly used in cases of wounds and bone fractures; also for female reproductive disorders. |
Morinda bajitian Morinda officinalis |
dispels chill, invigorates yang |
Mainly used when yang deficiency manifests in chilliness and cold-caused pain. |
Psoralea buguzhi Psoralea corylifolia |
dispels chill, nourishes blood |
Used in cases of coldness due to yang deficiency; also used in treating bone marrow deficiency. |
Tortoise shell guiban Chinemys reevesii |
lowers yang, cools blood, nourishes blood, stops bleeding |
Frequently used for deficiency of yin and blood with yang agitation or bleeding, with modern use for aplastic anemia. |
Turtle Shell biejia Trionychidae species |
softens lumps, disperses accumulations |
Used for abdominal masses; combined with tortoise shell (guiban) in treatment of yin and blood deficiency with sweating. |
Providing the Herbal Formulations
In China, the majority of the reported work done with cancer patients has been through administration of high dose decoctions. The decoction form allows for adjustment of ingredients according to patient presentation. This form also allows for a high level of active constituents, since a quantity of one to two cups of tea can maintain in soluble form the extractable content of about 100-200 grams of dried crude herbs. The decoctions are prepared for the patients when they are in hospital, and that service is often continued by the hospital pharmacy for out-patients.
Many western patients (though certainly not all) reject the decoction form due to the lengthy cooking procedure, the smell of the herbs while being prepared, and the taste of the decoction when consumed. The use of dried decoctions to make “instant” teas removes these first two barriers, but usually imposes a significant cost, and few practitioners or patients realize that the conversion from 100-200 grams of dried herbs in decoctions corresponds to about 20-40 grams of dried decoctions (made as 5:1 extracts).
By switching to culturally acceptable forms, such as pills, capsules, and tablets, the quantity of herb materials that can reasonably be ingested is greatly reduced, while the cost may remain relatively high. Some herbs are successfully used in their powdered form in somewhat modest quantity, and some extracts that can be put into pill form are more concentrated than the dried decoctions used to make tea. Therefore, with some careful design, herbal materials in these more acceptable forms may be utilized, but with the understanding that a significant number of “units” must be consumed to have the desired impact, that is, to have more than a placebo effect or greater than a barely perceptible outcome.
Transitioning from Tonic Formulation
The attempt to counteract the adverse effects of chemotherapy came to be known as Fu Zheng treatment, meaning to “support normality.” The concept was that adverse influences, whether those described in ancient times (often as evil qi, xieqi) or of modern times (such as side effects of powerful drugs) were resisted by the person’s normal qi, which could be strengthened by tonic herbs. Later, this basic concept was broadened to what Pan Mingji had described as Fu Zheng Pei Ben, where the latter term means to strengthen the root, referring to supplementing the depleted foundation of qi, blood, and essence (jing). In his 1988 book describing that approach (13), Pan presented a generalized prescription based on his clinical work with cancer patients undergoing chemotherapy which he dubbed Yiqi Buxue Jianpi Tang (yiqi is a term used to indicate strengthening the qi and raising the clear qi; buxue is to nourish the blood; and jianpi is to strengthen the spleen). His formula was a very high dose decoction as follows:
Yiqi Buxue Jianpi Tang
Chinese Name |
Common Name |
Dosage |
Relevant Action |
huangqi |
astragalus |
15-30 |
tonify qi, strengthen spleen |
dangshen |
codonopsis |
15-18 |
tonify qi, strengthen spleen |
baizhu |
atractylodes |
12 |
tonify qi; strengthen spleen |
fuling |
hoelen |
12 |
improve spleen function |
gancao |
licorice |
4.5 |
tonify qi; strengthen spleen |
shudi |
rehmannia |
15 |
nourish blood |
gouqizi |
lycium |
12 |
nourish blood |
heshouwu |
ho-shou-wu |
12 |
nourish blood |
huangjing |
polygonatum |
10 |
tonify qi |
nüzhenzi |
ligustrum |
15 |
nourish yin |
beishashen |
glehnia |
10 |
nourish yin |
maimendong |
ophiopogon |
10 |
nourish yin |
jixueteng |
millettia |
24 |
nourish blood |
qianshi |
euryale |
12 |
strengthen spleen |
shanyao |
dioscorea |
12 |
strengthen spleen |
The decoction of about 200 grams of herbs could be further modified to address specific symptoms, mainly by adding more herbs, though some of the standard ingredients might be removed as well (he did not indicate which might be removed, but gave lists of potential additions). Dangshen (codonopsis) was being used as a substitute for renshen (ginseng). Although renshen was the preferred ingredient, this prescription was written at the time when the herb was mainly reserved for manufactured products and for export, not allowed for most hospital prescriptions.
The effects of tonifying qi and strengthening the spleen, and of nourishing blood and yin are each supported by several herbs of Pan’s basic formula, but in light of the six herb actions, it is weak in the areas of circulating qi and blood, and only slightly directed at benefitting marrow.
Use of this particular formulation in the west turned out to be problematic for a number of reasons, most of them described above in terms of the decoction form of the herbs. The instant tea (dried decoctions) that were available for use appeared more attractive, and formula selection came from Japan.
In Japan, the practice of Chinese herbal medicine called Kampo, has been based on selecting formulas from a group of prescriptions that had been selected by experts in the early 1950s and then relied upon continuously since then. The problem of countering side effects of chemotherapy was raised in the 1980s, and the primary formula selected for that purpose was Shiquan Dabu Tang (Ginseng and Tang-kuei Ten Combination). At that time, and until recently, the Kampo formulas were provided to the west mainly through Taiwan rather than Japan, and this particular formula was well-known. It tonifies qi and strengthens the spleen with the ingredients of Si Junzi Tang (Major Four Herbs Combination) and nourishes and vitalizes blood with the ingredients of Si Wu Tang (Tang-kuei Four Combination), and also aids the uplifting of clear qi with huangqi (astragalus). A number of its ingredients are considered important for enhancing immune functions, including renshen, huangqi, baizhu, and gancao. The formula is relatively weak in the areas of promoting circulation of qi (danggui and chuanxiong have some effect), and it is also deficient in nourishing the marrow.
Chinese doctors also considered this formula for the same applications, but made various modifications to better suit their understanding of the needs. As an example (21), the base formula was modified by adding jixueteng (millettia), huangjing (polygonatum), gouqizi (lycium fruit), heshouwu (ho-shou-wu), shanzhuyu (cornus), lianzi (lotus seed), and shanyao (dioscorea), which primarily increased the tonification effects and more closely approximated Pan’s recommended formula; it was stronger in benefiting marrow than Shiquan Dabu Tang alone.
Early Efforts at ITM
At the end of the 1980s, as Pan’s Fu Zheng Pei Ben book became available, concerns regarding cancer therapies remained strongly focused on immunosuppression. This was a decade before approval of the drug neuopogen for helping stimulate production of white blood cells (WBC), when a break in the chemotherapy regimen was common; allowing for growth and metastasis of cancer cells, making them resistant to further treatment. An early effort at countering the immunosuppression was an ITM formula in tablet form designated Astragalus 10+ (Huang Qi Da Bu Pian). The name reflects a key ingredient for enhancing immune functions, and portrays the development of the formulation, which began in 1986 as “Astragalus Eight Herb Formula” was then expanded to Astragalus Ten Herb Formula, and finally to the twelve herb version (hence the “+”) first described in 1988. It includes the eight herbs that were subject of considerable research efforts following up on the “adaptogen” model, as mentioned above, and eventually adding others which were consistent with the concept of Fu Zheng Pei Ben therapy. Using renshen (ginseng) rather than dangshen (codonopsis), Astragalus 10+ includes ingredients of Pan Mingji’s prescription: (maimendong) ophiopogon, nüzhenzi (ligustrum), heshouwu (ho-shou-wu), baizhu (atractylodes), and huangqi (astragalus). It additionally provides the adaptogens ciwujia (eleuthero) and wuweizi (schizandra), and these other ingredients: lingzhi (ganoderma; reflecting the growing interest in medicinal mushrooms for cancer patients), roucongrong (cistanche; pursuing the idea of nourishing kidney yin and yang to enhance marrow function), and shangshen (morus fruit, which nourishes yin and blood while improving marrow, having a function similar to gouqizi). The formula can be properly described as a combination of tonic herbs, with principles of action being to tonify qi, raise clear qi and yang, nourish blood, and benefit marrow. In relation to six herb actions, the formulation is weak in the areas of regulating qi circulation and vitalizing blood (lingzhi was considered a blood vitalizing herb). The number of tablets to take was rather large to help approach a useful dosage, though one could not come close to the massive dosage of Pan’s decoctions.
An effort to get a decoction format was also made. The concept behind it was to suggest turning to this form of administration for patients recently diagnosed and about to start or just starting chemotherapy, before the most severe symptoms had set in. The patient would have a chance to get used to making and drinking decoctions without the presence of nausea, and the result of using the formula would hopefully reduce the severity of the reactions, permitting continued use of the decoction for some time. The usual recommendation, provided in advance of offering the first batch of crude herbs, was to plan on using the decoctions for about three weeks then follow-up with tablets if desired.
The crude herbs were provided in packets that were ready to cook as a tea, and labeled Astragalus/Oldenlandia Mixture. The intent of the formula was illustrated in the name, with astragalus already well-known for qi tonifying and immune enhancing effects and with baihuasheshecao (oldenlandia) being one of China’s “anticancer” herbs. This herb is almost always used in combination with banzhilian (scutellaria) for cancer patients, and its activity was increasingly attributed to immune-related functions rather than any direct inhibition of cancer cell growth. Given the concerns about development of chemotherapy induced nausea that could inhibit use of this form of the herbs, digestion-promoting, stomach-calming ingredients were included: yizhiren (alpinia), sharen (cardamom), and shenqu (shen-chu). To help assure the continued distribution of “clear qi,” jiegeng (platycodon) was included to resolve phlegm and stagnation in the chest. The choice of yizhiren and sharen was made to also aid the circulation of qi, as these spicy agents would disperse stagnation. Further, based on the concept that qi and blood deficiency were early adverse effects of chemotherapy, huangqi in this formula was paired with the blood nourishing agents shudi (rehmannia) and biejia (turtle shell). Since qi and blood deficiency engendered impairment of blood circulation, jixueteng (millettia) and danshen (salvia) were also used. The combination of shudi and biejia for nourishing kidney yin with danshen and jiexueteng for microcirculation were expected to help protect bone marrow. This formulation was thus an early representation of the six actions approach that this article has described.
A new tablet formula was then composed, to be one of the potential alternatives to Astragalus 10+, which made use of an herb gaining interest by Chinese physicians working with cancer patients: jiaogulan (gynostemma). This herb was not one of the mainline TCM ingredients, but was known from folk medicine. Researchers discovered that its active components were similar to, and in some cases the same as, those of ginseng. Based on traditional uses, it also has some of the properties attributed to jiegeng (platycodon). The following formula, called Gynostemma Tablets (Fu Zheng Kang Ai Pian), was made for patients with concern about low bone marrow function (22):
| jiaogulan | Gynostemma |
| huangqi | Astragalus |
| baizhu | Atractylodes |
| baihuasheshecao | Oldenlandia |
| gouqizi | Lycium |
| heshouwu | Ho-shou-wu |
| danggui | Tang-kuei |
| buguzhi | Psoralea |
| tusizi | Cuscuta |
The emphasis is on tonifying qi and raising clear qi (huangqi, jiaogulan, baizhu) and nourishing blood and yin (danggui, heshouwu, gouqizi), but two herbs are included for benefiting marrow, buguzhi (psoralea) and tusizi (cuscuta), and these two were selected because they were being used in China for conditions of low production of blood cells, such as in cases of aplastic anemia as well as for leukopenia secondary to cancer chemotherapy.
This formula returns to the focus on tonification therapy, but was intended to be combined with another formula, such as one for regulating qi and vitalizing blood, and this is because it lacks the other methods of therapy that have been identified as of importance for these cases.
Further investigation of Chinese prescriptions for bone marrow deficiencies led to design of a second formula, called Millettia 9 (Ji Xue Teng Pian) that could be combined with one of the above combinations (Astragalus 10+ or Gynostemma Tablets or the Astragalus/Oldenlandia Decoction) providing an emphasis on blood vitalizing to restore microcirculation to the marrow (22):
| jixueteng | Millettia |
| danshen | Salvia |
| sangshen | Morus fruit |
| yejiaoteng | Polygonum stem |
| huangqi | Astragalus |
| chuanxiong | Cnidium |
| shudi | Rehmannia |
| xuduan | Dipsacus |
| muxiang | Saussurea |
This formula is derived from blood-nourishing prescriptions described in Chinese medicine publications for bone marrow depression. As an example, if one combined Gynostemma Tablets with Millettia 9, the formula closely approximates Jixueteng Yijing Tang (23; Millettia Raise the Marrow Decoction), which likewise includes jixueteng, danshen, huangqi, and shudi from Millettia 9 and gouqizi, huangqi, heshouwu, buguzhi, tusizi, and danggui from Gynostemma Tablets, the only other ingredients in Jixueteng Yijing base formula are ejiao (gelatin), nüzhenzi (ligustrum), and hanliancao (eclipta).
In these formulas, jixueteng (millettia) and danshen (salvia) are of particular interest because Chinese doctors consider these to have both vitalizing and nourishing properties, which is also true of chuanxiong (cnidium). Yejiaoteng (polygonum stem) is the stem of heshouwu, sharing in its blood nourishing properties. Muxiang regulates qi circulation, but also helps raise clear qi. Xuduan with shudi benefit both the yang and yin of the kidney to nourish marrow; xuduan (dipsacus) has the secondary effect of vitalizing blood circulation. A combination of Gynostemma Tablets and Millettia 9 will contribute to all six methods of therapy, with perhaps a weakness in the area of raising clear qi, though that is addressed with huangqi (astragalus) and baizhu (atractylodes); regulating qi circulation is also somewhat limited, accomplished in part with chuanxiong (cnidium) and primarily with muxiang (saussurea). Still, the Chinese concept that nourishing the blood of the liver allows it to better circulate qi definitely applies here, and there is considerable focus of these formulas in nourishing blood. This pair of formulas used together is one which practitioners at IEP have considered especially effective.
The difficulty encountered is delivering these six therapeutic methods with a relatively small number of herbs, so additional formulation work is underway. Normally, two to three herbs are to be employed for each therapeutic action, relying especially on herbs that provide more than one of those actions. Each of these two formulas has 9 herbs, and there are 17 different herbs (though heshouwu and yejiaoteng could be deemed a single herbal material, so 16); this is comparable to Pan’s base formula of 15 herbs.
To consolidate multiple formulas into one concise prescription that incorporates all six herb actions is accomplished by selecting only those herbs that are most critical to the desired effects. A previous presentation of six actions herb prescribing came about by combining three TCM formulas for helping patients with multiple sclerosis and other autoimmune disorders. After successful treatment, or as a result of natural disease variations, when the patient is in a relatively stable condition, a formula can be utilized to help maintain that condition. In 1998, the formula called Remission Pills (San Fang Ding Ji Pian; San Fang refers to three formulas) was introduced by ITM for these cases. It involved the combination of Xiao Chaihu Tang (Minor Bupleurum Combination) to tonify qi, raise clear qi, and regulate qi circulation, Tao Hong Siwu Tang (Tang-kuei Four Combination with taoren and honghua) to nourish blood and vitalize blood, and Liuwei Dihuang Wan (Rehmannia Six Formula) to benefit kidney. Because of the different application, the sixth action did not focus as much on the marrow aspect of the kidney as would formulas for cancer patients. The formula has 18 ingredients.
An investigation of herb prescribing at the IEP Clinic shows that certain formulations aside from the usual ones for counteracting adverse chemotherapy effects are used with some frequency. Some are given only once or intermittently for particular situations that arise, such as using a prescription for common cold or influenza or a combination suited for an acute injury. The most commonly used prescription for general use, often given for an extended time, is a tablet called Bupleurum 12 (Tiao He Pian; the name refers to its harmonizing intent). This is a “constitutional” formula that addresses general imbalances rather than a specific symptom or disease. Bupleurum 12 is especially useful for regulating qi and raising qi and yang, the two areas where a combination such as Gynostemma Tablets and Millettia 9 are somewhat weak. Although I do not advise combining three formulas at once to get the desired actions (but prefer to design alternative formulas that provide the desired therapeutic actions with fewer herbs), it is worthwhile to see how the herbs in these three frequently used formulas at IEP Clinic serve to address the six herb actions:
Action |
Herbs with Primary Use in the Category |
Herbs with Secondary Use |
Tonify qi |
huangqi, renshen, jiaogulan, gancao |
baizhu |
Regulate qi |
chaihu, zhishi, muxiang |
danggui, chuanxiong |
Raise clear qi |
fuling, banxia, ganjiang |
huangqi, baizhu, renshen, chaihu |
Nourish blood |
danggui, baishao, shudi, heshouwu, gouqizi, sangshen, yejiaoteng |
jixueteng, danshen, chuanxiong |
Vitalize blood |
jixueteng, danshen, chuanxiong, |
xuduan, baishao, danggui |
Benefit marrow |
buguzhi, tusizi, xuduan |
shudi, goujizi |
In working toward developing more concise formulations, a starting point is the key herbs that generate the desired actions. Some of the herbs described in this article are clearly central to the treatment strategy for aiding cancer patients suffering from side effects of their medical therapies, including huangqi (astragalus), jixueteng (millettia), shudi (rehmannia), baizhu (atractylodes), and danggui (tang-kuei). The other formula ingredients are best chosen to extend the properties of those herbs, and in this case, attention to marrow benefiting herbs is distinctly needed. Of the six herb actions, the regulation of qi has been the weakest aspect of this area of formula development and it is my hope that this deficiency will be recognized by the explanations provided here and rectified in the future. While some specific herbal combinations that are used at the IEP Clinic have been described here, the same approach can be utilized with other formulations, so these serve only as examples for explanation. Most importantly, the six herb action prescribing method provides a foundation for designing an effective treatment.
References
- Dharmananda S, Adjunct Cancer Therapy at the Immune Enhancement Project (IEP) Clinic. 2013 Institute for Traditional Medicine, Portland, OR.
- Dharmananda S, Acupuncture and Herbs for Mind/Brain Disorders (part I: Acupuncture). 2000 Institute for Traditional Medicine, Portland, OR.
- Dharmananda S, Towards a Spirit at Peace. 2005 Institute for Traditional Medicine, Portland, OR.
- Dharmananda S, Acupuncture for Shen Disorders Update, 2006 Institute for Traditional Medicine, Portland, OR.
- Zhang L, Generalized Anxiety Disorder and Acupuncture Treatment. Acupuncture.com 2010: 8 (7).
- Zhu B, Wang HC, Case Studies from the Medical Records of Leading Chinese Acupuncture Experts, 2010 Singing Dragon, Philadelphia, PA.
- Cheng XN (chief editor), Chinese Acupuncture and Moxibustion. 1987 (revised 1999; third edition 2010) Foreign Languages Press, Beijing.
- Xu XG (chief editor), Therapeutics of Acupuncture and Moxibustion (vol 6. of The English-Chinese Encyclopedia of Practical Traditional Chinese Medicine). 1989 Higher Education Press, Beijing.
- Dharmananda S and Vickers E, Synopsis of Scalp Acupuncture. 2000 Institute for Traditional Medicine, Portland, OR.
- Dharmananda S, Chinese Herbal Treatment for Multiple Sclerosis and Other Flaccidity Syndromes, Including Myasthenia Gravis and Amyotrophic Lateral Sclerosis. 1996 Institute for Traditional Medicine, Portland, OR.
- Dharmananda S, Treatment of ALS with Chinese Medicine. 2003 Institute for Traditional Medicine, Portland, OR.
- Cheung CS, Kaw UA, Treatment of Toxic Effects Resulting from Radiation and Chemotherapy by Traditional Chinese Medicine. 1980 Traditional Chinese Medicine Publisher, San Francisco, CA.
- Pan Mingji (compiler). Cancer Treatment with Fu Zheng Pei Ben Principle. 1987/1988 Fujian Science and Technology Publishing House, Fuzhou
- State Administration of TCM and Pharmacy, Advanced Textbook of Traditional Chinese Medicine and Pharmacology (v. 1). 1991 New World Press. Beijing.
- Dharmananda S, Enumerating the Methods of Therapy. 1997 Institute for Traditional Medicine, Portland, OR.
- Dharmananda S, Counteracting the Side Effects of Modern Medical Therapies with Chinese Herbs. 1998 Institute for Traditional Medicine, Portland, OR.
- Kun J. Prevention and Treatment of Carcinoma with Traditional Chinese Medicine. 1983/1985 Commercial Press, Hong Kong.
- Pan Mingji (compiler). How to Discover Cancer through Self Examination. 1990 Fujian Science and Technology Publishing House, Fuzhou.
- Liu L and Liu ZW, Essentials of Chinese Medicine (v 2). 2010 Springe-Verlag, London
- Cheng LK, Heaven Above, Earth Below. 2011 http://lok-kwan.com/2011/08/21/heaven-above-earth-below/
- Wang YR, Influence of Shiquan Dabu Tang (Ginseng and Tang-kuei Ten Combination) on immune functions after radio- and chemotherapies in tumor patients. Hubei Journal of Traditional Chinese Medicine 1997; 19(5): 21–22.
- Dharmananda S. A Bag of Pearls. 2004 Institute for Traditional Medicine, Portland, OR
- Dharmananda S, Millettia (jixeuteng). 1999 Institute for Traditional Medicine, Portland, OR.
February 2014