Autoimmune Diseases
and the potential role of Chinese Herbal Medicine
by Subhuti Dharmananda, Ph.D., Director, Institute for Traditional Medicine, Portland, Oregon
BACKGROUND TO THE DISEASE CATEGORY
Autoimmune diseases are chronic disorders that have been difficult, and often impossible, to cure. There can be remission of symptoms—spontaneously or as the result of applied therapies—but the potential for return of the disease remains in almost all cases. The characteristic of these diseases is immune system targeting of body components, so that these components are damaged, either temporarily or permanently, or their activities are altered. The autoimmune diseases almost always have a significant genetic component; in addition many of the diseases in this category appear to have a viral or other infectious agent as a trigger for onset of the autoimmune status. There may be a variety of other factors that are important to finally set off a pattern of symptomatic disease so that its first manifestation may be after age 20 (there are also late-onset autoimmune diseases). In fact, if the disease appears much earlier than that (i.e., prior to the teen years), it is usually a very aggressive form with a strong genetic component.
There are dozens of diseases that are classified as involving autoimmune responses or suspected of having an autoimmune basis. In many of the diseases, there is a significant difference in incidence among men and women; overall, women are about 3 times as likely as men to suffer from autoimmune disorders (however, in some disorders, such as MS, men appear to have a more severe disease pattern). If the initial symptoms are mild or if the disease progresses slowly or develops its symptoms in an unusual pattern, diagnosis is difficult. Some patients relay experiences of pursuing medical diagnosis and treatment for a decade before getting a definitive disease name. A greater number of tests that can suggest or confirm presence of an autoimmune disease have become available so that it is now easier to make a diagnosis than ever before, but some disorders suspected of being autoimmune diseases still lack reliable tests, especially for their early stages.
The incidence of autoimmune diseases in the U.S. has been estimated to be just over 3%, with a current affected population of about 10 million people. Societies representing people suffering from autoimmune diseases consistently over-report the incidence rates, using the upper limits from the highest estimate ranges; thus, the incidence rates given in these circumstances—often relayed by the news media—must be interpreted cautiously. Some of the common autoimmune disorders are outlined below.
Connective Tissue Diseases
The most prevalent autoimmune disorders are connective tissue diseases, accounting for nearly half of all the cases; rheumatoid arthritis is the dominant one. The main connective tissue diseases are:
RHEUMATOID ARTHRITIS
This is a systemic disorder in which immune cells attack and inflame the membrane around joints (it also can affect the heart, lungs, and eyes, though rarely). The incidence in women is far higher than men for younger individuals, but the difference is less with disease onset after age 50. Symptoms: Inflamed and/or deformed joints, loss of strength, swelling, pain.
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE)
SLE can affect virtually any organ system, producing inflammation. It is up to 9 times more common in women than men and occurs in black women 3 times as often as white women. Symptoms: 90% of patients experience joint inflammation similar to rheumatoid arthritis. Fifty percent develop a classic “butterfly” rash on the nose and cheeks. Raynaud's phenomenon (extreme sensitivity to cold in the hands and feet) appears in about 20 percent of people with SLE. Other symptoms include fever, weight loss, hair loss, mouth/nose sores, malaise, fatigue, and brain disorders. Exposure to UV light can promote the disease process.
SYSTEMIC SCLEROSIS (SCLERODERMA)
Scleroderma results from attack of immune cells that produce scar tissue in the skin, internal organs, and small blood vessels. It affects women three times more often than men overall, but increases to a rate 15 times greater for women during childbearing years, and appears to be more common among black women. Symptoms: In most patients, the first symptoms are Raynaud’s phenomenon and swelling and puffiness of the fingers or hands. Skin thickening follows a few months later. Other symptoms include skin ulcers on the fingers, joint stiffness in the hands, pain, sore throat, and diarrhea.
SJÖGREN'S SYNDROME
Sjögren's syndrome is a chronic, slowly progressing inability to secrete saliva and tears, and is usually a late-onset disease. It can occur alone or with rheumatoid arthritis, scleroderma, or SLE. About 90% of cases occur in women, most often at or around the menopausal years. Symptoms: Dryness of the eyes and mouth, swollen neck glands, difficulty swallowing or talking, unusual tastes or smells, thirst, tongue ulcers, and severe dental caries (which occur because of the lack of saliva).
The other autoimmune diseases fall into several groupings, among the most common are these:
Neuromuscular Diseases
The neuromuscular diseases are mainly those involving immune attack affecting the nerves, which has the result of impairing muscle responses. The primary response is usually muscular paralysis, but there can also be tremor and/or tonic spasm where nerve transmission is partially blocked.
MULTIPLE SCLEROSIS (MS)
A disease of the central nervous system that usually first appears between the ages of 20 and 30, and affects women twice as often as men. MS is the leading cause of disability among young adults, and it causes irreversible scarring of the myelin sheath to varying extents. The primary form is remitting/relapsing, but there is also a “progressive” form, which worsens regularly. Symptoms: Numbness, weakness, tingling or paralysis in one or more limbs, impaired vision and eye pain, tremor, lack of coordination or unsteady gait, and loss of control of urination.
MYASTHENIA GRAVIS
This is characterized by gradual muscle weakness, often appearing first in the face, particularly at the eyes and then affecting the mouth and throat. Symptoms: Drooping eyelids, double vision, and difficulty breathing, talking, chewing, and swallowing.
Endocrine Diseases
The endocrine diseases involve attack of the immune system against one of the glands, sometimes with rapidly progressing destruction (as in diabetes or Addison’s disease). However, in Grave’s disease, antibodies attach to a hormone stimulating receptor on thyroid cells and don’t destroy the cells but rather stimulate their production of thyroid hormone.
HASHIMOTO'S THYROIDITIS
This is a type of autoimmune disease in which the immune system destroys the thyroid gland. It is primarily a disease suffered by women (50 times more often than men). Symptoms: Low levels of thyroid hormone cause mental and physical slowing, greater sensitivity to cold, weight gain, coarsening of the skin, and goiter (a swelling of the neck due to an enlarged thyroid gland).
GRAVES' DISEASE
Graves' disease is one of the most common autoimmune diseases, affecting about 1% of people in the U.S, frequently appearing during childhood, and affecting women 7 times as often as men. Patients with Graves' disease produce an excessive amount of thyroid hormone. Symptoms: Weight loss due to increased energy expenditure; increased appetite, heart rate, and blood pressure; tremors, nervousness and sweating; frequent bowel movements.
INSULIN-DEPENDENT (TYPE 1) DIABETES
Type 1 diabetes is caused by autoimmune attack against the pancreatic islet cells that produce insulin, resulting in very low levels of insulin production, usually too little to survive without providing exogenous sources (insulin shots). The disease usually occurs in children and young adults (differentiated from Type 2 diabetes that does not originate from autoimmune processes, and most often affects those who are obese), and affects boys and girls at about the same rate, a slightly higher incidence in boys. Symptoms: Increased thirst, increased urination, weight loss, fatigue, nausea, frequent infections.
Other Autoimmune Diseases
Some of the more common disorders that don’t fit the above categories are mentioned here. These occur in roughly equal rates for men and women.
INFLAMMATORY BOWEL DISEASE
Inflammatory bowel disease refers primarily to two autoimmune disorders of the small intestine—Crohn's disease and ulcerative colitis. Symptoms of Crohn's disease: Persistent diarrhea, abdominal pain, and general fatigue. Symptoms of ulcerative colitis: Bloody diarrhea, pain, urgent bowel movements, joint pains, and skin lesions. In both diseases, there is a risk of significant weight loss and malnutrition.
HEMATOLOGIC AUTOIMMUNE DISEASES
Blood cells can be affected by autoimmune disorder. In autoimmune hemolytic anemia, red blood cells are prematurely destroyed by antibodies; in thrombocytopenic purpura (usually described as ITP), the immune system attacks the platelets, and in autoimmune neutropenia (destroying a group of white blood cells, neutrophils). These diseases often occur in children and are believed to be triggered by a viral infection in many instances.
UNDERSTANDING THE DISEASES
Many times, autoimmune disorders are mistakenly described as excessive responses of the immune system or deranged responses of the immune system (“the immune system has broken down”). In fact, this depiction is misleading. A portion of the immune system has been targeted to attack specific parts of the body, in the same manner that it would target a pathogen; it may be functioning normally and without disorder, other than the “target,” which was established by genetics and certain events. Thus, even if the immune system is in all other ways normal, this response gives rise to the disease symptoms. What is of particular interest is the fact that for several of the autoimmune diseases the activity of the immune system may come and go, so that there are periods of “remission” and periods of “exacerbation.” For these diseases, if a method for maintaining remission can be found, then even though the underlying condition isn’t completely eliminated, it is not producing new symptoms or progressing. And, a discovery for significantly prolonging remission may result in developing strategies for addressing other, more consistently active autoimmune diseases.
The medical method of treating many of these diseases that has been available for about a century is with potent anti-inflammatory and immune-inhibiting drugs. The therapy usually provides a very quick beneficial result (noted within hours of the first dose) but then there is the conundrum that most of these drugs are not well suited to long-term therapy, so there has been a difficult risk-benefit balancing to help keep people symptom free to the extent possible without them suffering too many side-effects or adverse events. Overall, the results have been remarkably good, but far from satisfactory.
An example of the unusual steps that may have to be taken to maintain results is in Grave’s disease, which involves an antibody-induced stimulation of the thyroid gland rather than inflammation. Absent a good method to inhibit the immune system’s role in overproduction of thyroid hormone, a treatment commonly used is to eliminate the thyroid tissue by administering radioactive iodine and then provide an exogenous source of thyroid hormone for life. This method saves lives and helps people lead a life free of the serious Grave’s disease symptoms, but one would prefer to eventually resolve the antibody problem instead and preserve the thyroid gland.
Modern research has aimed at two ways of addressing the basic problem: one is trying to interrupt the specific immune attack (rather than using broad immune suppression) by determining which substances can interact with the involved portion of the immune system; the other is to find ways to modulate the immune response so that there is less likely to be an attack against the body (but still leaving the immune system fully capable of fending off infections or inhibiting other pathological processes). Other approaches to treatment will develop with genetic engineering, use of stem cells, and upcoming techniques yet to be evaluated.
An example of the immunological approach is use of IVIG (intravenous immunoglobulin) for ITP. This treatment is based on extraction of human blood plasma, which is rich in immunoglobulins that interfere with the destruction of platelets by the autoimmune process. The treatment is fast acting, but does not cure the disease, and little is known about its mechanism. IVIG is currently very expensive and reserved for emergency cases, though its use is becoming more prevalent with favorable experience. The standard therapy is to use prednisone, which is inexpensive, also has quick response, but can not be maintained long term (spleen removal also helps reduce the severity of the disease, but rarely halts its progression for long). Another example is an experimental approach to treating MS in early stages of investigation. In this disease, T-cells are involved in the attack against the myelin sheath of the nerves of the central nervous system. The T-cells appear to be controlled by exposure to large amounts of the myelin proteins they normally would attack, so by intravenous administration of these proteins, the MS attacks might be impaired. Currently, MS patients take drugs that are derivatives of interferon which modifies the immune response in a manner not fully understood, but results in reduced frequency of exacerbations for the remitting/relapsing type of MS.
If there is success in the endeavors to interrupt the autoimmune attacks, patients my not need to turn to Chinese medicine as a potential method of alleviating autoimmune responses. However, medical research is several years away from finding reliable treatments, and even where some success has been attained, there are limitations. Thus, patients with these diseases will for many years be seeking help through adjunctive methods, such as traditional Chinese medicine.
CHINESE MEDICINE AND AUTOIMMUNE DISEASES
The long tradition of Chinese medicine that has led up to its modern practice did not have a concept that clearly correlates with what we know today as autoimmunity. Possibly the closest concept was related to the idea of trapping a pathogenic force inside the body (for example, by closing the pores rather than dispelling pathogens through sweating), or by providing conditions that would invite such a pathogen to remain in the body (e.g., interior nourishment and dampness, but weak defense), so that a disease would continue far longer than it should. Xu Dachun (1) described a condition where the body’s own qi merges with that of the pathogen; he used the analogy of oil poured into flour: the ingredients can not be separated. In such situations, the body’s normalizing efforts may end up participating in the problem, and this reminds us of the case where the immune system is participating in an attack against the body itself. He also mentions a situation where a disease appears to have been cured, but then suddenly it seems to come back and may even end in death; he likens the situation to a fight between two tigers, where one wins (that is, the body wins; the pathogen is defeated), but in doing so, it has exhausted all his strength and eventually succumbs as well. This can remind us of a remitting and relapsing autoimmune disease. Although there are some intriguing parallels with autoimmunity in these kinds of stories, the fact is that the ancient Chinese depictions are too general for us to use in any practical way.
Generally, the traditional Chinese medical ideas became fixed upon the concept of external pathogens (which can be climactic influences, such as cold and wind) entering the body; they might then be successfully expelled. With autoimmunity, one part of the body (an invisible immune system component) is attacking another part (such as connective tissue), and there may be no foreign disease component involved at the time (even if one served as a trigger years earlier) and nothing to “expel.” Thus, the analogies remain limited.
Most times, the description of diseases in the pre-20th century literature of China gives us insufficient information to associate them with specific modern diseases. That is because the literature would often leave out key elements we need to make the correlation, such as how long the disease has lasted and how it has varied over time (months). More typically the descriptions in the Chinese texts involve the immediate situation: the symptoms as presented and how the disease has changed over just a few days. Then, it is impossible to know if this was a case of exacerbation of an autoimmune disease, or if it was an infectious disease, or some other condition. Still, we are able to turn to the centuries of Chinese medical experience for insights into at least one of the autoimmune diseases: rheumatoid arthritis. It seems evident from the Chinese literature that this disease existed in the past; we have the traditional descriptions which show a distinct overlap—in terms of symptoms and disease progression—with the modern depiction.
The textual evidence points to rheumatoid arthritis among other painful disorders of the joints, muscles, tendons, ligaments, blood vessels, and other tissues: the bi syndromes. In the Neijing Suwen, it is indicated that the pathological entities of wind, cold, and wetness could lead to such a “bi” syndrome, at least one of which had characteristics of rheumatoid arthritis. It was said in that ancient record that when the wind component dominated, the symptoms would migrate; when cold dominated, the condition would be especially painful; when dampness dominated, the site of the affliction would become fixed (today, Chinese literature often attributes this localization to blood stasis and/or phlegm accumulation).
During the 20th century, Chinese doctors began routinely incorporating modern medical diagnostics into the field of traditional medicine. Immunology didn’t develop significantly anywhere in the world before the 20th century, and it came to China somewhat late, but was immediately applied to discussion of traditional disease categories and to the use of herbs or their active components for treatment of the disorders. Chinese publications in the late 1970s and into the 1980s showed awareness of immune system components in the autoimmune diseases, but there was lack of clarity as to what role they might play. Then, during the 1990s, as Western literature was more readily accessed, Chinese studies began to concentrate on specific immune system components and the role of mediators of immune responses, which brings us to the current situation.
TRADITIONAL APPROACHES INTO THE MODERN TIME
The development of traditional Chinese medicine over the centuries led to a focus on treating patients individually according to the “signs and symptoms” (syndrome) rather than according to a disease name. The exception to the general principle is that certain herbs or acupuncture points might be deemed especially “good for” a disease type, such as bi syndrome, and included for that reason primarily. As Chinese medicine was modernized during the 20th century, great emphasis was still placed on this approach of “differential diagnosis.” Reports of diagnostics and treatments based on this method shed only limited light on the basis for Chinese herb treatment of autoimmune diseases, because of the great variability in treatment from patient to patient and even from visit to visit of the same patient, and also because of the lack of specific diagnosis. Thus, for example, a report on treating rheumatoid arthritis might involve patients with several different diseases that could have been distinguished by modern means, because the focus of attention was on the Chinese medicine syndromes. Also, the claims of resulting improvements as the result of treatment were not reliable due to a number of political, social, and educational factors prevalent during this period.
An example of a report from this field may suffice to reveal the difficulties. In the 1983 Journal of the American College of Traditional Chinese Medicine (2), a lengthy article by Lin Jiehou on rheumatoid arthritis—as treated by one of China’s leading physicians Wang Weilan—was presented. Wang Weilan is to this day a medical doctor at the Beijing Municipal TCM Hospital. This is how the disease was described:
Rheumatoid arthritis is a generalized chronic disorder. It usually has a prolonged course with complicated manifestations. The existence of hot, cold, excess, deficiency and the persistence of the bi entity eventually involve the yin, yang, qi, blood, and the five solid organs [zang]. In the struggle between the evil and normal qi of both the hot and cold types of rheumatoid arthritis, the flourishing of either of the evils will generate a state of deficiency. The pertinent tonification of the deficiency, supporting the normal qi, and the dissipating of the evil are critical in a proper treatment. Clinically, it is recognized that there is qi deficiency, blood deficiency, and deficiency of the organs. For qi deficiency, herbs for tonifying qi are used; for blood deficiency, herbs for tonifying blood are used; for yin deficiency, the principle used is to moisten the yin; for yang deficiency the principle used is to tonify the yang.....From the wholistic point of view, although rheumatoid arthritis usually manifests as a local lesion, the disease process is intimately related to the entire integrated defense mechanism of the body, which is explained by the following: “The normal qi must be deficient before the evil can take the opportunity to invade....The internal existence of normal qi will prevent the interference by the evil.” Therefore, the deficiency of the normal qi is the basis of the internal factor and leads to the looseness of the cutaneous tissue [body surface] and the lowering of the body’s resistance. If the external factor is the contraction of cold in the winter, then the cold evil can take the opportunity to enter the weak and deficient body and to directly strike at the ligaments and the bones, thus causing: internal damage to the blood and the meridians, qi stagnation, blood stasis and ecchymosis, and limitation of movements. The prolongation of the disease course will cause the cold evil to transform into heat and form toxins; thus, there will be the appearance of both cold and hot, and the existence of both deficiency and excess symptoms which creates a very complicated situation.
This description fits the generally recognized theories of traditional Chinese medicine. While the authors is admitting to a “complicated situation,” one can see in the analysis reference to virtually every category of pathology: wind, cold, heat, damp, blood stasis, normal and evil qi, blood, yin/yang, five internal organs, deficiency, excess, toxins, etc. This seeming state of disarray or lack of focus in the description of the disease, its pathology, and its treatment, reflects two important features of traditional Chinese medicine:
1. The tradition developed in the absence of modern analysis of disease. Attempting to apply the traditional concepts to a modern disease category (such as rheumatoid arthritis) is very difficult because the origins and nature of the descriptions are so different. There are claims often made by Western practitioners of Chinese medicine that they are able to target the underlying problem to resolve the disease (while modern medicine can only suppress symptoms), because they identify the syndrome and target it. In fact, it is a complicated matter to pin down a specific pattern, as displayed in the above description, and many times practitioners rely instead on selecting from a small number of set formulas for the disease; perhaps one for people sensitive to cold, another for those with joints that feel hot, one for upper body manifestation, and another for the lower body. However, such selection is really aimed at the “branch” of the disease, rather than the “root.”
2. While Traditional Chinese medicine presents therapeutic methods that correspond directly to the diagnostic categories (hence; the comments by the above quoted author: for qi deficiency, tonify qi; for blood deficiency, tonify blood, etc.), there had been no specific claims for success in the past. Instead, Chinese authors would usually simply state that for a certain syndrome one should apply a certain corresponding remedy. Thus, it is possible that these treatments might be given with only moderate or temporary improvements. Then, as medical doctors and researchers began treating patients in the modern setting, they found that the responses were not as clear cut as hoped, so that they would express the fact that the situation was complicated.
The above explanation must be taken in context: rheumatoid arthritis (as is the case with most autoimmune diseases) is not easily understood by modern medicine and although initial treatments are usually simple, over time, the situation becomes quite complex. On the other hand, broad categories, such as qi, blood, yin, and yang and their corresponding tonics is far less precise that the modern medical knowledge of the disease and the treatment options.
Medical journals presenting clinical reports in China began appearing from all the major hospitals, medical colleges, and research institutes (which were often grouped into giant complexes). For rheumatoid arthritis, many of the reports described “new” agents, such as the active components of Tripterygium wilfordii (leigongteng), which is a toxic plant (though it can be used without apparent adverse effects by many patients). It has potent immunosuppressive activity from it glycosides similar to that attained with steroids, but without the usual steroid side-effects. Other isolated active ingredients, such as the alkaloids of Sinomenium, were indicated as helpful, but these alkaloids could cause serious side-effects in a significant portion of the treated patients. There were also numerous reports of using ordinary decoctions.
As an example, Li Jun, at the Ministry of Health in Gansu, reported on treatment of 46 cases of rheumatoid arthritis with a decoction (3). The formula he used was comprised mainly of herbs that vitalize blood (such as achyranthes, cyathula, persica, cnidium, tang-kuei, carthamus), but it was modified according to differential diagnosis for each patient. He claimed that “12 patients were cured, 25 markedly improved, and 7 improved.” This appears a remarkable result; according to modern medical analysis, this disease is almost never cured, yet here more than one in four patients was said to be cured; in addition, more than half the remaining patients were markedly improved (this category was explained: “signs and symptoms basically disappeared). One would think that with such results, this formulation would be studied further and developed into a modern drug or health product or a routine therapy at one or several of the hospitals, especially since none of the ingredients reported to be used were toxic in normal dosage. However, this report was never followed up, and though many other doctors in China have reported using blood-vitalizing herbs, their formulas were apparently based on their own ideas, rather than pursuing what Li Jun had accomplished in Gansu. Why?
There are two primary answers to this:
1. The results reported in many such publications were, in fact, unreliable and other researchers in China were aware of this. Under the conditions that prevailed at the time of Li Jun’s work (in the 1980s, published in 1988), clinical reports were often exaggerated. Therefore, no follow-up was called for.
2. A highly competitive situation existed (and still exists) in this field; each doctor has his favored recipes and is interested in working with his own formulation(s) and reporting their success, rather than following-up a prior study with a formula of someone else’s design.
This is an unsatisfactory situation that is only gradually improving. The lack of adequate progress is easily noted in the English language publications from China, such as the Journal of Traditional Chinese Medicine and the Chinese Journal of Integrative Medicine. In relation to the first point, it has been noted that virtually all TCM clinic reports issued in Chinese journals provide positive results, often extremely positive; negative results are rare, and usually involve only a “control” substance, which might be a commercial product that the researcher is pointing to as inferior to his test formulation. In relation to the second point, frequently researchers provide very limited information about the formula, hiding ingredients, not disclosing proportions, and giving incomplete details of dosing, thus protecting their personal recipes, but also preventing others from pursuing the apparently promising research further.
Today, the study techniques are getting better, and therapies thought to be of benefit are more often being subjected to pharmacological analysis to verify activity and determine a mechanism of action. As an example, in a report in the 2000 issue of Journal of Traditional Chinese Medicine (4), the authors presented six data tables showing characteristics of the patients, comparison of overall therapeutic results, analysis of the symptom and sign changes, and the changes in laboratory measures of the patients’ blood, such as immunoglobulins, rheumatoid factor, sedimentation rate, T-cell subsets, and changes in hemoglobin and red blood cells. There were two treatment groups, with some details given about the herbs used (one for yang deficiency; one for yin deficiency), and a control group using an established herbal formula on the market.
In that report, as with other studies, there is a remarkable result claimed: of 87 cases treated with the research formulations, 9 were said to be “clinically cured,” and 58 showed that the treatment was “markedly effective.” Only 13 cases were said to show the treatment ineffective. Yet, up to this time (six years later), further research on these particular formulas has not been presented. The authors, led by Zhou Xueping and Zhou Zhengying at Nanjing University of TCM, ventured an explanation of the disease:
Rheumatoid arthritis is a chronic obstinate disease that involves multiple joints all over the body. Because of its diversity in classification and therapeutic principles in TCM, there has been confusion whether it is a deficiency or excess in nature. We hold that deficiency of the liver- and kidney-yin, stagnancy of qi due to accumulation of pathogenic cold in channels and collaterals, and phlegm stagnation combined with blood stasis are the main pathogenesis, of intermediate and late rheumatoid arthritis. The cardinal viscera being deficient is the kidney, the syndrome belongs to the category of deficiency in origin and excess in superficiality, or deficiency intermingled with excess, which also has the differences of cold and heat, yin and yang in nature. If one suffers from insufficiency of the yang-qi and invasion of pathogenic cold and dampness from the outside for a long time, manifestations of yang insufficiency, cold in the interior, stagnation of phlegm, and blood stasis would occur. If one has yin deficiency, the pathogenic wind, dampness, and heat would take advantage of the yin deficiency and invade into the body. In this case, treatment with drugs too warm and too dry in nature, the stagnating cold would transform to heat, resulting in damp-heat syndrome, a pathogenic factor causing too much consumption of yin and blood. Therefore, tonifying kidney, resolving phlegm, and removing blood stasis are the primary principles in the treatment....
There is a slightly more focused presentation than in the earlier analysis quoted, but this is partly because the authors have decided here to focus on more advanced cases, thus eliminating some of the variables associated with also considering more recent disease onset. While these explanations are instructive in revealing the way these physicians thought, they are far from definitive. Descriptions like these are so broad and lacking in evidence to support them, that it is difficult to apply practically.
The same lead authors presented another paper in the same journal in 2004 (5), reporting on another formulation, claimed to be derived from one of the formulas used in the prior report, but containing almost no overlapping ingredients other than rehmannia and wasp’s nest. This was given to patients with rheumatoid arthritis of the yin deficiency type with “heat in the collaterals.” As with the above paper, they claimed a similar level of effectiveness with 9.5% cured, 38.1% markedly effective and only 9.5% ineffective, with better results than a control group treated with Tripterygium. They explained:
In rheumatoid arthritis (RA), though arthralgia due to cold is commonly seen clinically, arthralgia due to heat is also frequently seen. RA of the type of yin-deficiency and heat in the collaterals is caused by the following factors: weak body constitution, deficiency of yin and blood, invasion of exogenous heat, improper use of drugs, and so on. If yin is deficient, the evils of wind, dampness, and heat would invade through the weak points, and then channels and collaterals would become obstructed. If yang is in excess there would be excessive heat in the body. After invading into the body, the evils of wind, cold, and dampness will produce heat with the help of the excess of yang. When these evils remain in the body, their stagnation would cause damp-heat. Furthermore, if the drugs too warm and dry in nature or hormones are taken for a long term, yin and blood might be consumed. This disease manifests as excessive in superficiality at the beginning, but there is deficiency in origin at the same time. Deficiency of the kidney is the root cause of the occurrence of RA of the type of yin deficiency and heat in the collaterals, which is the pathogenic basis for long-term arthralgia....
In the formulation revealed by the authors, raw rehmannia and loranthus were included to nourish the kidney yin; the main focus was on treating inflammation with sinomenium, silkworm, wasp’s nest, and other herbs that have such a reputation; the selected ingredients do not necessarily treat heat or yin deficiency. The basic theory presented by the authors is that the weak body allows for invasion of exogenous factors, which, in this case, produce a heat syndrome. There is a surprising lack of commentary about the unusually good results in this and the other reports, other than the apparent superiority to the control treatments. In this case, because Trypterigium is so potent, a further analysis and discussion would seem essential.
While Chinese medical reports indicate the presence of clear-cut syndromes in the patients, there are difficulties in lack of consistency in diagnostics among Western practitioners. Studies have shown that if the same patients are presented to different experienced practitioners of traditional Chinese medicine, the diagnosis will often not be in agreement among them. This was confirmed recently in the analysis of patients with rheumatoid arthritis (6). Three American practitioners of Chinese medicine who each had at least 5 years experience were presented with 40 rheumatoid arthritis patients. The average agreement rate for the individual patient diagnostic category among the practitioners was just 31.7%. However, when they prescribed textbook remedies (standard formulas, such as Duhuo Jixue Tang), they had a high level of agreement in their recommendations, about 91.2% of the time. This evaluation demonstrates, as described earlier, that there are a few basic formulas that practitioners will rely upon, and they are usually applied without much reliance on refined diagnostics, but instead turning to certain obvious and general conditions.
Despite the difficulties with the Chinese literature, we may be able to distill some valuable lessons from the intensive work done in China. It is a matter of sorting through the various concepts and reports to follow the theories and practices. I have chosen to focus on rheumatoid arthritis for the analysis given above because of its higher frequency of occurrence than other autoimmune disorders and the fact that it has a long history of analysis and treatment in China. The results that could be obtained by examining the Chinese literature for numerous autoimmune disorders would be beyond what can be presented here. Some analysis of the literature on rheumatoid arthritis and other autoimmune diseases have been set forth in other ITM publications, which are available on the ITM web site (www.itmonline.org); these include: ulcerative colitis, Raynaud’s syndrome, scleroderma, lupus, multiple sclerosis, and ITP.
UNDERLYING DISORDER
Autoimmune disorders, because of their chronic nature are understood to be based on an underlying deficiency syndrome, as was explained by Lin Jiehou and Zhou Xueping. In brief, it is the deficiency that permits the pathology to manifest. If the vessels were full of qi and blood, and the organs working properly and full of their essences, the person would be healthy, or might, at the worst, suffer minor and short term diseases. Instead, the deficiency condition allows external pathogenic influences to enter, and permits the disease to progress, transform, and become serious because of inadequate resistance to this process by the normalizing qi. Genetic factors involved in diseases are often associated with the Chinese concept of essence deficiency (specifically, a kidney deficiency); diseases that progress with aging are also attributed to deficiencies of kidney and liver and involve the “essence” deficiency (jingxu). The potential role of viruses or other infectious agents in triggering the disease process (as indicated by some modern investigations) corresponds, in part, to the failure to repel the external pathogen.
As underlying contributors to disease, one would expect the deficiencies to be evident prior to the initiation of the autoimmune disease. On the other hand, there might be little chance to observe this because the deficiencies might involve only those aspects of qi, blood, and essence that regulate resistance to certain disease conditions, so that more obvious signs of deficiency, such as pallor, fatigue, imbalances of heat and cold, etc., might not be especially pronounced for such individuals. Still, one would expect that by undertaking a careful diagnosis prior to the onset of the autoimmune symptoms, some deficiencies would be observed. Otherwise, the TCM theory would have to be relinquished.
In order to more firmly establish the presence of such underlying deficiencies, it would be necessary to obtain medical histories (including information oriented to reveal the standard “signs” recognized by TCM practitioners) from persons who were recently diagnosed with an autoimmune disease. That way, they might be able to reliably recall preceding conditions, particularly those in months before the first clear evidence of the disease. Such an investigation has not yet been done. Most attention is naturally focused upon treatment of persons who are seeking relief from an existing disease, one which may have been present for some time already since early symptoms are often easily controlled by modern drugs while Chinese herbal medicine is sought out if the disease is inadequately controlled by that means or if the drugs are not well tolerated.
According to common TCM approaches to disease treatment, tonification of the deficiencies would be a part of the therapy throughout treatment, since the effect of other therapeutic approaches would be boosted by the presence of adequate qi, blood, and essence. For example, to vitalize circulation of blood, the qi must be adequate, according to the Chinese theory. Tonification would be especially important during any phases of remission where there would not be an immediate requirement to intensively alleviate inflammation, pain, and other acute symptoms, while it would usually be a secondary part of the treatment if the acute syndrome is present.
BRANCHES
Each autoimmune disorder manifests differently, and often one disease appears entirely unrelated to another, despite a common basis in immune attack. For example, early onset diabetes (type I) results in hunger, weight loss, excessive urination, fatigue, and other symptoms, while connective tissue diseases may result in pain, stiffness, swelling, and redness; ITP results in spontaneous bleeding (or risk of it), and Sjogren’s disease results in dryness. Put simply, the symptoms of the autoimmune disease—and the TCM analysis of them—will depend on which cells in the body are the subject of attack by the immune system.
Nonetheless, there are some secondary patterns that are relatively consistent. First, any of the diseases that reach an advanced stage appear to manifest at least two imbalances defined in TCM. One is the deficiency of kidney that may be at the root of the disease but may also come about from the damage caused by the disease process or even by the drugs previously used to control the disease. This deficiency may manifest as cold or hot symptoms (depending on whether yin or yang is most severely affected), weakness of limbs, fatigue, changes in bowel and urination patterns, dryness or excess moisture. The other is development of blood stasis (which is considered a type of “excess” pattern). Blood stasis can occur directly as part of the local disease manifestation (for example: the autoimmune attack causes inflammation, which damages the capillary beds in the affected area) or as a later effect (for example, high blood sugar in diabetes over time causes circulatory disorders, with damage to both the capillary beds and the larger vessels).
In the case of advanced rheumatoid arthritis described by Zhou, it was suggested that in addition to kidney deficiency and blood stasis, phlegm accumulation was involved. Even so, in the treatments used for those arthritis cases, each formula had only one herb specific for resolving phlegm accumulation (sinapis in one formula and arisaema in the other).
Certainly, in each disease, one has to consider that there will be additional factors, aside from kidney damage and blood stasis, though the kidney imbalance may explain many of those additional factors (e.g., kidney cold leads to accumulation of phlegm in the channels). Treating the kidney system successfully may help resolve these other secondary disorders. The presence of obvious hot or cold symptoms is a major reason for modifying formulas; it is common to use cinnamon, aconite, and other warming herbs that benefit the kidney yang for cold disorders, and to use raw rehmannia and moutan along with other herbs to clear heat in the blood, for the hot disorders.
MODERN ANALYSIS
Many herbs and isolated active components of herbs, when evaluated in model systems (such as cell cultures or laboratory animals), are shown to have anti-inflammatory activities or immune-regulating functions. Unfortunately, it is often difficult to project from the laboratory studies to the effects that might be attained in the complex autoimmune diseases as they manifest in humans. Still, it may be worth mentioning here an example where the results are intriguing. Some Chinese herbs that are frequently used in treatment of autoimmune diseases have been analyzed for active component groups, which are then tested to demonstrate a possible mechanism of action in autoimmune disorders. Testing in models of arthritic inflammation is relatively easy and it is in demand because of the high frequency of the disease. We can begin the examination with the central herb for kidney tonification, a common ingredient in formulas for chronic diseases, particularly autoimmune disorders, and used in formulas for cold and for hot syndromes: rehmannia.
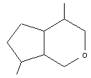 Rehmannia used in most kidney tonic formulas, such as Rehmannia Six Formula (Liuwei Dihuang Wan) and Rehmannia Eight Formula (Bawei Dihuang Wan), has as primary active components a class of chemical substances called iridoid glycosides. Iridoids, a type of monoterpene, have the basic structure shown here; which often has a glucose molecule attached, making it a glucoside (general term: glycoside). Iridoid glycosides are among the main active components for two ingredients of these formulas: rehmannia (dihuang) and cornus (shanzhuyu). And, for those formulas containing the yang tonic cistanche (roucongrong), there are additional iridioids that it provides.
Rehmannia used in most kidney tonic formulas, such as Rehmannia Six Formula (Liuwei Dihuang Wan) and Rehmannia Eight Formula (Bawei Dihuang Wan), has as primary active components a class of chemical substances called iridoid glycosides. Iridoids, a type of monoterpene, have the basic structure shown here; which often has a glucose molecule attached, making it a glucoside (general term: glycoside). Iridoid glycosides are among the main active components for two ingredients of these formulas: rehmannia (dihuang) and cornus (shanzhuyu). And, for those formulas containing the yang tonic cistanche (roucongrong), there are additional iridioids that it provides.
Iridoid glycosides are also found as major components of some of the heat-clearing herbs, such as gardenia, scrophularia, picrorhiza, plantago seed, and chin-chiu (qinjiao) that are sometimes included in treatment of autoimmune disorders. For example, in a report on lupus therapy by integrated traditional and modern medicine (7), patients received Lingdan Pian, which included at least three herbs with iridoid glycosides: chin-chiu (qinjiao), rehmannia, and scrophularia; the formula also contains ching-hao, moutan, turtle shell, buffalo horn, licorice, and other herbs. In a treatment for ITP (8), the main ingredients of a formula included at least two herbs with iridoid glycosides: gardenia and raw rehmannia; the formula also contains red peony, moutan, tang-kuei, and astragalus. In the treatment of rheumatoid arthritis of the yin deficiency type described in the first report by Zhou, the formula included the iridoid-containing herbs rehmannia and chin-chiu; other formula ingredients were ho-shou-wu, campsis, and earthworm.
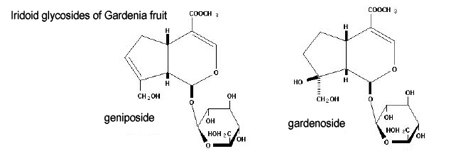
Recent studies revealed that geniposide, and other iridoids from gardenia fruits (see sample structure illustrations above, the glucose molecule is at the bottom right of each structure), showed pharmacological action consistent with suppressing immune inflammatory processes. For example, the compounds produced significant inhibition of IL-2 secretion, thus reducing antibody-stimulated activation of human peripheral blood T cells (9). In another study (10), it was shown that geniposide could lower serum IL-1β and TNF-α levels in rheumatoid arthritis rats, which was suggested to be related to its clinical effects of inhibiting development of rheumatoid arthritis. In another study, extract of chin-chiu (Gentiana macrophylla) was used in animal models of inflammation (11). It was noted in the abstract that:
The anti-inflammatory activity observed in Gentiana macrophylla is comparable to that observed in prednisone. These observations suggest that Gentiana macrophylla displays considerable potency in anti-inflammatory action and could be used as an anti-inflammatory agent in the control of inflammation of rheumatoid arthritis.
Chin-chiu extract tablets were used in previous Chinese clinical work in the treatment of lupus (SLE). It was claimed to be especially effective for nephropathy, arthralgia, and erythema, and contributed to improvement in blood parameters indicating immune status (12).
This kind of work—with clinical evaluations, chemical analysis, and pharmacological investigations—may help elucidate the role of traditional medicine in autoimmune diseases and point to efficacious treatments relying on selected herbs or their active components. Such efforts would not necessarily overshadow the potential benefits of using additional herbs to treat “constitutional” or other aspects of a disease, but would aid in the process of selection from the huge number of herbs that are currently in use. The applicatiion of herbs and their active components for autoimmune diseases would rarely be cause for concern when combining this type of therapy with modern drugs. Very few cases of interactions that would be detrimental have been observed with use of herbs and drugs, and those few cases are mainly restricted to certain drugs (e.g., Warfarin) and certain herbs (e.g., St. John’s Wort) that are not routinely used in these cases (13). Thus, there is a good possibility for utilizing Chinese medicine for patients with autoimmune diseases relying on both traditional concepts and modern developments.
REFERENCES
Unschuld PU, Forgotten Traditions of Ancient Chinese Medicine, 1990 Paradigm Publications, Brookline, MA.
Lin Jiehou, Bi-entity (arthritis): Clinical experience of master-physician Wang Weilan, Journal of the American College of Traditional Chinese Medicine 1983; (3): 3–28.
Li Jun, Treatment of 46 cases of rheumatoid arthritis with modified Shentong Zhuyu Tang, Beijing Journal of Traditional Chinese Medicine 1988; (6): 35–36.
Zhou Xueping, et.al., Intermediate and late rheumatoid arthritis treated by tonifying the kidney, resolving phlegm, and removing blood stasis, Journal of Traditional Chinese Medicine 2000; 20(2): 87–91.
Zhou Xueping, et. al., Clinical study of Qingluo Tongbi Granules in treating 63 patients with rheumatoid arthritis of the type of yin deficiency and heat in collaterals, Journal of Traditional Chinese Medicine 2004; 83–87.
Zhang GG, et. al., Variability in the traditional Chinese medicine (TCM) diagnoses and herbal prescriptions provided by three TCM practitioners for 40 patients with rheumatoid arthritis, Journal of Alternative and Complementary Medicine 2005; 11(3): 415–421
Zhong Jiaxi, et. al., 25 cases of systemic lupus erythematosus treated by integrated traditional Chinese medicine and Western medicine, Chinese Journal of Integrated Traditional Chinese Medicine and Western Medicine 1999; 19(1): 47-48.
Fruehauf H, The Treatment of Difficult and Recalcitrant Diseases with Chinese Herbs, 1997 ITM, Portland, OR.
Chang WL, et. al., Immunosuppressive iridoids from the fruits of Gardenia jasminoides, Journal of Natural Products 2005; 68(11): 1683–1685.
Zhu J, et. al., Effect of geniposide on serum IL-1beta and TNF-alpha of rheumatoid arthritis rats, Chinese Journal of Traditional Herbal Drugs 2005; 30(9): 708–711.
Yu F, et. al., Inhibitory effects of Gentiana macrophylla extract on rheumatoid arthritis of rats, Journal of Ethnopharmacology 2004; 95(1): 77–81.
Yuan ZZ and Feng JC, Observation on the treatment of systemic lupus erythematosus with a Gentiana macrophylla complex tablet and a minimal dose of prednisone, Chinese Journal of Integrated Chinese and Western Medicine 1989; 9(3): 156–157.
Dharmananda S, Checking for possible herb-drug interactions, START Manuscripts 2003, Portland, OR.
 Rehmannia used in most kidney tonic formulas, such as Rehmannia Six Formula (Liuwei Dihuang Wan) and Rehmannia Eight Formula (Bawei Dihuang Wan), has as primary active components a class of chemical substances called iridoid glycosides. Iridoids, a type of monoterpene, have the basic structure shown here; which often has a glucose molecule attached, making it a glucoside (general term: glycoside). Iridoid glycosides are among the main active components for two ingredients of these formulas: rehmannia (dihuang) and cornus (shanzhuyu). And, for those formulas containing the yang tonic cistanche (roucongrong), there are additional iridioids that it provides.
Rehmannia used in most kidney tonic formulas, such as Rehmannia Six Formula (Liuwei Dihuang Wan) and Rehmannia Eight Formula (Bawei Dihuang Wan), has as primary active components a class of chemical substances called iridoid glycosides. Iridoids, a type of monoterpene, have the basic structure shown here; which often has a glucose molecule attached, making it a glucoside (general term: glycoside). Iridoid glycosides are among the main active components for two ingredients of these formulas: rehmannia (dihuang) and cornus (shanzhuyu). And, for those formulas containing the yang tonic cistanche (roucongrong), there are additional iridioids that it provides.