BORNEOL, ARTEMISIA, and MOXA
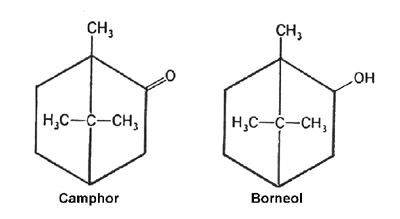
Borneol refers both to a specific chemical compound (see Figure 1) and to a mixture of similar compounds (of which borneol is one) in a resinous crude material obtained from certain herbs. The chemical constituent borneol is one of the active ingredients of artemisia, which contains other aromatic compounds of similar structure and medicinal function. Both borneol (as a crude resin) and artemisia are utilized internally and externally in the practice of Chinese medicine. Moxa is shredded artemisia that is burned on or near the body to produce local heating, as well as to generate an additional influence from the moxa material itself, perhaps imparting borneol and other active constituents to the body. In this article, the properties, uses, and interrelations of borneol, artemisia, and moxa are explored.
The medicinal agent borneol (bingpian) refers to the resin obtained from Dryobalanops aromatica (see Figure 3) or from Blumea balsamifera. Both plants are rich in the natural chemical constituent borneol (also known as borneol camphor). Synthetic borneol, obtained by simple chemical transformation of camphor and turpentine oil, is sometimes used in China as a substitute for the natural product. In recent years, new sources of natural borneol have been discovered, mainly certain species of Cinnamonum tree (cinnamon tree). These may eventually become a resource for natural borneol. Borneol was first recorded in the Tang Bencao (Materia Medica of the Tang Dynasty), published in 659 A.D., where it was described (1) as being "bitter, acrid, and slightly cold, used to dispel pathogenic factors in the chest and abdomen."
Artemisia argyii (aiye) which is the same as or interchangeable with Artemisia vulgaris (vulgaris = common), refers to the leaves of the Chinese mugwort, which are used as an internal medicine and as the source of moxibustion wool. The herb was recorded as a medicinal ingredient by the famous Taoist herbalist Tao Hongjing around 500 A.D. He mentioned it in two of his books: the Ming Yi Bie Lu and Bencao Jingji Zhu, where it was originally called ai (the character shows two blades of the cutting shears). Today, it is usually called aiye (ye = leaf). The herb had already been used for moxibustion prior to Tao's mention of it, and had been included in early herb formulas, such as those of the Jingui Yao Lue (ca. 200 A.D.). As will be discussed below, artemisia has the fragrance of borneol; their uses are similar.
The typical form of borneol is in thin, semi-opaque, whitish angular pieces or crystals, and this appearance is the reason for its current Chinese name (bing = ice, pian = slice). A detailed description of this substance appeared in the Bencao Gangmu (1596 A.D.), where it was not called bingpian, but rather was called ai (same Chinese character as used for aiye, artemisia). The association with aiye (Artemisia argyii) is not coincidental: the active constituents of aiye include borneol, camphor, and cineole, which are also the main components of natural bingpian. Blumea, the local Chinese source of bingpian, is in the same plant family as artemisia (Compositae); it is not uncommon for plants of the same family to yield similar chemical ingredients. Blumea is called ainaxiang (fragrant herb that looks like artemisia).
Three forms of borneol were mentioned (2) in the Bencao Gangmu: aifen (powdery borneol), the crude product aipian (the refined substance, now known as bingpian), and aiyu, a by-product of distillation. The material was obtained from Blumea grown in the southern part of China, primarily Hainan Island (near Canton), or from imported material (from Borneo in Indonesia) derived from Dryobalanops. Borneol was originally used as a carminative to reduce fevers and alleviate digestive distress. It was also said to inhibit worms. Another name given to borneol was longnaoxiang (dragon camphor fragrance), referring to its alchemical applications (the term "nao" also means brain).
Today borneol is classified as an agent for opening blocked orifices, and is described as pungent, bitter, and slightly cold (3). It is indicated for severe obstruction of the orifices (that may cause coma or convulsive diseases), for heat syndromes, and for pain. Although not often mentioned as useful for this purpose, borneol is a common addition to treatments for lung diseases in modern clinical practice. It is also applied topically (usually with other substances) for a wide range of conditions, mainly for swelling in the throat, mouth sores, ear infections, cervical erosion, psoriasis, boils, pain, and eye diseases.
Because the resin is strongly aromatic and, partly, because of its historically high price (which has been reduced in recent years, in part due to the availability of the synthetic version), the recommended dosage is quite small. Many herb guides list the internal dosage as 30 to 100 mg, taken in powders or pills (if added to a decoction, it will all evaporate). The Pharmacopeia of the PRC (4) indicates 150 to 300 mg per day. It appears that Chinese Herbal Medicine: Materia Medica (5) by Bensky and Gamble has an error in reporting of dosages, indicating 300 to 900 mg per day, a higher recommendation than virtually all other sources.
The largest amount of borneol used in a traditional style formula is in Guanxin Suhe Wan, which has been made into a patent remedy. This is a modern version of the traditional prescription of the He Ji Ju Fang called Suhexiang Wan (6). The manufacturer of Guanxin Shuhe Wan (7) reports 5 ingredients (styrax, borneol, frankincense, sandalwood, and aristolochia), with borneol comprising 15% of the prescription (borneol was 4% of Suhexiang Wan). Suhexiang Wan contains these same ingredients plus 9 others (including the endangered rhino horn and musk, and the potentially toxic cinnabar). The recommended daily dosage of the patent remedy is 1 pill (or capsule) each time, 1-3 times per day, with each pill containing about 100 mg of borneol (thus, the daily dose would be 100 to 300 mg of borneol, in the same range as the modern Pharmacopoeia... recommendation).
The borneol source Blumea balsamifera is also an important herb of Ayurvedic medicine (called kukundara). In the Indian Materia Medica (8) it is described as containing a volatile oil with the odor of wormwood (the common name applied to several Artemisia species). The Indian uses are similar to the Chinese: fresh juice of the leaves is dropped into the eyes to treat chronic purulent discharges; internally, it is used for worms and dysentery. Additional uses are treatment of chronic uterine discharges (it is listed as an astringent) and of a certain "disease of the nose called Ahwah, peculiar to Bengal, and accompanied by strong fever, heaviness in the head, and pains in the neck, shoulders, and loins." It is also mentioned as an expectorant. The borneol source Dryobalanops aromatica is described in the Indian Materia Medica. It is described as being diaphoretic, antiseptic, antispasmodic, and stimulant, and said to be a tree closely related to the Indian Sal tree (Shorea robusta in the same plant family), the resin of which is widely used in Indian medicine.
Borneol, and the closely related compound bornyl acetate, are ingredients of cardamon, nutmeg, ginger, lindera, magnolia bark, turmeric, liquidambar, and camphor oil. All of these are used in the treatment of pain syndromes. Interestingly, all these herbs are said to have a warming quality, while borneol itself is said to be "slightly cold." Blumea is listed in the Materia Medica as warming, as are most other materials classified along with borneol as opening the orifices, such as musk, acorus, and styrax. It is possible that the classification of borneol as being slightly cold is an error introduced at a time when its applications were more limited (focused on treating diseases with fever).
Borneol is used in greater frequency for topical applications than for internal use. Those applications are numerous, but especially apply to injuries, burns, rheumatic pains, hemorrhoids, skin diseases, and ulcerations of the mouth, ear, eye, and nose. Borneol (or camphor, see section below) is almost always used in complex formulas, and typically comprises 1.6 to 8.5 percent of the total prescription. Because topical preparations are often difficult to make in convenient form on the spot, they are frequently used as patent remedies. Some examples, with the labeled quantities of borneol or camphor, are (7):
| Anti-rheumatic Plaster (Jing Zhi Goupi Gao) | 
| 5% borneol |
| Plaster for Rheumatism (Shang Shi Zhi Gao) | 
| 8.5% borneol |
| Fel Ursi Hemorrhoids Ointment (Xiongdan Zhi Chuang Gao) | 
| 1.6% borneol |
| Injury Plaster (Shang Shi Bao Zhen Gao) | 
| 7.1% camphor |
| Liquid for Injuries (Zheng Gu Shui) | 
| 2% camphor |
For short-term administration, a larger proportion of borneol may be utilized. For example, in the English-Chinese Encyclopedia of Practical Traditional Chinese Medicine, vol. 4 (9), a recipe for treating purulent otitis media is:
| borneol | 
| 20% |
| dragon bone | 
| 33% |
| alum | 
| 20% |
| kaempheria (camphor root) | 
| 27% |
This is combined with one pig gallbladder. The powdered materials are applied in the ear once per day. Kaempheria (shannai) is a relative of ginger that contains borneol and camphor. Traditionally, kaempheria is used topically for toothache and internally for warming the spleen and stomach to treat cold pain in the abdomen, vomiting, and diarrhea.
The Manual of Dermatology in Chinese Medicine (10) provides the following examples of special preparations with borneol for application to the skin:
Luhui Binz Zhu Weifu Ji: 1 fresh aloe-vera leaf, 0.3-1.0 grams borneol, a pinch of pearl powder: mash the ingredients together and apply 1-2 times daily for herpes zoster sores.
Bing Shi Dan: 30 grams calcined gypsum powder, 0.6 grams borneol powder: combine and apply to herpes zoster pustules.
Di Yu Er Cang Hu Gao: 18 grams each of phellodendron, atractylodes (cangzhu), and xanthium, 36 grams sanguisorba, 3 grams menthol, and 1.5 grams each of calomel and borneol: grind to powder, combine with petroleum jelly, and apply to skin 2-3 times daily for atopic dermatitis.
Dong Chuang You: combine 5 grams borneol and 15 grams camphor with 100 grams dried chili peppers: grind the borneol and camphor into powder and add to a hot water extract of chili pepper (steep peppers in hot water for 10 hours in closed container, string and then add alcohol to precipitate solids that are removed). Add glycerine and apply the ointment 3-4 times daily to the affected area (but not ulcerated lesions) for treating frostbite.
Qing Liang Fen: combine powdered talcum (120 grams), licorice (20 grams) and borneol (12 grams): sprinkle on affected area 3-5 times daily for treatment of sunburn causing erythema, wheals, or itching.
Dahuang Bingpian Fang: combine 100 grams rhubarb powder and 20 grams borneol in 250 grams table vinegar: let steep for 7 days; apply to affected sites 3 times daily for seborrheic dermatitis.
Dingxiang Bingpian San: combine 30 grams cloves with 6 grams borneol: grind to powder and apply to underarms 1-2 times daily to treat sweat odor.
Historically, more is known about the therapeutically and chemically similar camphor than about borneol (often called Borneo camphor). Borneol is a component of camphor oil. Camphor is a molecule that differs from borneol by the loss of two hydrogen atoms with formation of an exposed double-bonded oxygen terminal (see Figure 1). This chemical difference makes camphor somewhat stronger than borneol, it also makes it more toxic. Like camphor, borneol and bornyl acetate (hydrogen is replaced by acetic acid at the oxygen terminal) are powerful agents for regulating qi and alleviating pain (see The use of aromatic agents for regulating qi, vitalizing blood, and relieving pain).
Camphor was originally obtained from Cinnamomum camphora (11), a tree native to the Far East (as mentioned previously, Cinnamonum trees have been found to be good sources of borneol). During the 18th century camphor entered into the world trade in medicinal products. During the U.S. Civil War, the demand for camphor was so high (being used to treat wounds, pain, itching, and other conditions faced by soldiers) that the U.S. contracted for the entire Taiwan supply. It was even proposed that an effort be made to purchase Taiwan in order to monopolize the camphor trade. It is perhaps for this reason that Japan acquired Taiwan in 1895. Prior to World War II, 80% of the world's camphor supply came from Taiwan.
Like borneol, camphor has been used in the Orient as an antiseptic, antispasmodic, carminative, cardiac stimulant, respiratory aid, and anthelmintic. The uses of camphor, as understood in the U.S., are quite similar to those for borneol used in China. These uses were outlined in the Eclectic Materia Medica in 1922 (12). Both the effects of low doses (therapeutic levels) and high doses (toxic levels) were depicted. Following are the comments related to therapeutic levels:
In small doses, camphor warms the stomach, stimulates [gastric] secretion, increases peristalsis, and expels flatus....Camphor is readily absorbed, both from application [topical] and inhalation....In moderate doses, camphor directly stimulates the heart-muscle, causing slower and stronger contractions and increased arterial pressure....Respiration is slightly stimulated by it....The action of small doses upon the nervous system is to produce a feeling of slight exhilaration and contentment.
As to the applications of camphor:
External: Camphor is stimulant, rubefacient, antipruritic, and feebly antiseptic. Owing to its agreeable odor and pleasant stimulating effects, it is largely used as a powder, in lotions, and ointments, or rubbed up with other solids to produce anodyne and antiseptic liquids. In this manner, when triturated with chloral hydrate, menthol, phenol, thymol, and similar bodies, ideal liquid antiseptics are obtained for use upon wounds, neuralgic, and other painful areas. Powdered camphor is an ingredient of tooth powders and pastes and dusting powders for skin diseases. Alone or with zinc oxide, talc, or precipitated chalk, it may be used upon bed-sores with decided relief. Such combinations are valuable in intertrigo, chronic eczema, urticaria, and zoster. Many snuffs contain powdered camphor, and it is useful to stimulate sluggish ulcers. Sprinkled upon the face, it is used to control itching and to prevent pitting in small pox. The spirit [alcohol preparation] is a household embrocation for the relief of pain and itching, and it is used largely, alone, or in lineaments and embrocations, for the relief of pain, stiffness, soreness, and swelling, as in myalgia, facial and other neuralgias, and upon rheumatic joints, deep inflammations, chronic indurated glands, and other indurations, sprains, contusions, and inflammatory swellings. An ethereal tincture of camphor is said to give relief in erysipelas. Inhaling the spirit, or camphor dropped into hot water, gives relief in nervous headache, and often aborts acute colds, coryza, and influenza, giving respite from the excessive secretion and the accompanying headache....
Internal: Camphor is used to allay nervous excitement, subdue pain, arrest spasm, and sometimes to induce sleep. It is an important remedy in many disorders of neurotic women and children, being frequently most effective as a nerve sedative, antispasmodic, and carminative in nervous nausea and vomiting, flatulence, hiccough, and tendency to spasms or fainting. It is especially serviceable in palpitation of the heart due to gaseous distention of the stomach, or to nervous irritability. In occipital headache from mental strain, or overstudy, small doses of camphor, together with the consentaneous use of it locally, frequently give prompt relief. Camphor taken and inhaled may abort cold in the head [head-cold, common cold], or alleviate it when established. It checks the sneezing, copious, watery secretions, and lachrymation, and relieves the nasal and frontal headache....In very small doses, it is useful in the bronchitis of the aged, while it helps greatly when depression attends slowly resolving cases of acute capillary bronchitis. The most important use for camphor is in a dynamic depression attending or following exhausting diseases. In typhoid, typhus, and other low forms of fevers and low grades of inflammation...it is one of the most active stimulating sedatives in the materia medica....
The use of camphor to treat nervousness, neurosis, and depression, with the action of a "stimulating sedative" may parallel the Chinese application of borneol, often used along with musk, acorus, and various sedative herbs to "open the obstructed heart orifices" and calm the agitated shen.
In modern Chinese medicine, the properties and uses of camphor are these, described in Oriental Materia Medica:
Actions: opens orifices; removes turbidity and filth; removes dampness; kills intestinal parasites; disperses swelling.
Applications: pain and swelling in the chest and abdomen, beriberi, dermatosis, dermatitis, scabies, toothache, external and internal trauma.
Synthetic camphor, often made by chemically modifying turpentine, is now widely used as a substitute for the natural product (just as synthetic borneol is being used).
The California Health Department, Food and Drug Branch, has raised concerns about the safety of borneol in patent remedies. For example, in their Compendium of Asian Patent Medicines (20), which is actually a report on analysis for lead, arsenic, mercury, and drugs (including certain plant constituents) in patents, all forms of borneol detected in the screening process are listed. These include isoborneol, endo-borneol, bornyl-acetate, and camphor. This concern appears to stem from the possibility of harm from very high doses of borneol, even though the usual amounts found in such products appear to be safe. Guanxin Suhe Wan, because it is currently available in the form of small capsules, might be accidentally taken in some overdose, but it seems unlikely that anyone would consume several times the 3 capsule recommended amount.
For references purposes, borneol is included in the amount of either 1% or 2% in some of the Seven Forests herb formulas made available from ITM for prescription by practitioners. In 700 mg tablets, this corresponds to 7-14 mg of borneol per tablet. With daily dosing of 6-18 tablets (the upper dose being the highest recommended in the ITM literature and twice the highest amount suggested on the label), the amount of borneol taken in one day can range from 42 mg (6 tablets, 1%) to 252 mg (18 tablets, 2%). The amount of borneol is either below or within the range suggested by the Chinese Pharmacopoeia (100-300 mg), and corresponds well with recommendations in various Materia Medica guides (which have dosages as low as 30 mg). The Seven Forests formulas, used as examples of traditional-style prescriptions, have about the same concentration of borneol (1-2%) as does ordinary cardamon seed. Cardamon, including sharen and baidoukou, commonly used as a medicinal as well as food spice, typically contains 2-3% essential oil, for which borneol and camphor, as well as closely related chemical compounds, are the primary constituents.
The concern about borneol apparently stems from a worry about camphor oil. Camphor oil was a popular medicinal in the U.S. until about 25 years ago when several instances occurred in which children were fed camphor oil by parents who failed to distinguish it from castor oil. The pure camphor oil is toxic when given in the doses (several grams) for which castor oil is used. Also, the U.S. Food and Drug Administration worried that topically applied camphor oil would penetrate the skin in sufficient amounts that it could cause trouble for persons with cardiac disorders who were taking various medications (camphor has mild heart stimulant activity). As a result, it is no longer possible to purchase camphor oil for household use in the U.S. and the FDA has cautioned against the use of Chinese lineaments that include camphor oil in the formulation.
According to the Chinese, camphor can be used in dosages of 0.3-1.5 grams per day for oral intake. Since camphor is more toxic than borneol, it would appear that doses of up to about 1.5 grams of borneol ought to be safe under most circumstances. The more usual levels of under 300 mg per day in commonly available products are not known to cause any harm.
There are dozens of species of Artemisia, many of them used medicinally. Artemisia argyi (see Figure 2) is most often used for external applications, including moxibustion. It is reported (13, 14) to contain the following components in its volatile oil, which makes up about 0.3% of the leaf: carveol, terpineol, carvone, elemol, cedrene, borneol, bornyl acetate, isoborneol, cineol (eucalyptol), caryophyllene, linalool, and thujone. Cineol, which is similar to borneol, is reported to make up 30% of the volatile oil. These components are likely responsible for the analgesic qualities of artemisia; other non-volatile components, especially tannins, are probably responsible for the hemostatic and astringent qualities.
In the early Chinese description of artemisia, the uses are almost identical to those for blumea and borneol. Here, from the Smith and Porter analysis of the Bencao Gangmu:
It is regarded as having hemostatic, antiseptic, and carminative virtues. Therefore, it is prescribed in decoction in hemoptysis, dysentery, menorrhagia, post-partum hemorrhage, snake and insect bites, as a wash for all sorts of wounds and ulcers, and to allay the griping pains of indigestion, diarrhea, or dysentery.
The internal use of artemisia is illustrated by its inclusion in the following two traditional formulas (6):
| Jiao Ai Tang | ||
| rehmannia | 
| 18 g |
| peony | 
| 12 g |
| tang-kuei | 
| 9 g |
| artemisia | 
| 9 g |
| cnidium | 
| 6 g |
| gelatin | 
| 6 g |
| licorice | 
| 6 g |
This formula is used for deficiency of the conception and governing vessels, leading to uterine bleeding, especially that which occurs during pregnancy or after delivery.
| Ai Fu Nuangong Wan | ||
| cyperus | 
| 22 % |
| artemisia | 
| 11 % |
| evodia | 
| 11 % |
| tang-kuei | 
| 11 % |
| cnidium | 
| 11 % |
| peony | 
| 11 % |
| astragalus | 
| 11 % |
| dipsacus | 
| 6 % |
| rehmannia | 
| 4 % |
| cinnamon bark | 
| 2 % |
This formula is used for deficiency and cold of the uterus, manifesting leukorrhea, sallow face, pain in the arms and legs, lassitude, poor appetite, irregular menstruation, abdominal pain, and infertility.
As examples of its topical application, Manual of Dermatology in Chinese Medicine lists these:
Cang Fu Shuixi Ji: equal parts xanthium, kochia, clematis, artemisia, and evodia. Decoct the ingredients and apply as a wet compress for 15 minutes, 3-5 times daily for folliculitis.
Chuan Ai Tang: 30 grams acorus, 7.5 grams each zanthoxylum and artemisia, and 7 pieces scallion whites. Decoct ingredients and wash affected area with warm decoction once or twice daily for scabies.
Lulutong Shuixi Ji: combine 60 grams each of liquidambar and atractylodes (cangzhu), and 15 grams each of stemona, artemisia, and alum. Decoct the ingredients and wash the affected sites with the warm decoction for psoriasis.
The dominant use of this herb is for moxibustion. Around the end of the 19th century, during the time when Chinese medicine was losing ground to other practices, including Western medicine, Smith and Stuart noted (2):
This treatment [moxibustion] is recommended and practiced indiscriminately by native doctors for nearly all of the ills to which flesh is heir-from itch to sterility. It is reported to have fallen somewhat into disuse in some parts of the empire, but in Kiangnan it seems to be as much employed by the native faculty as it ever was.
Compared to acupuncture, moxibustion is usually deemed a secondary practice. In the Niejing, the basis of ancient and modern concepts about acupuncture and moxibustion treatments, only a few sentences are devoted to moxibustion, mostly with mention in passing. As depicted in the book Chinese Acupuncture and Moxibustion (15) the practice of moxibustion is a back-up for the failure of other therapies:
Chapter 73 of Miraculous Pivot [Ling Shu] states, "A disease that may not be treated [is not successfully treated] by acupuncture may be treated by moxibustion." In Introduction to Medicine [1575 A.D.] it says, "When a disease fails to respond to medication [Chinese herb therapies] and acupuncture, moxibustion is suggested."
A search for commentary on the history of moxibustion turns up little; the subject has not generated widespread interest, and the quotations above are typically the only reference to the traditional literature. A monograph on artemisia (Aiye Chuan), published around 1500 A.D. by Li Yenwen, was lost; its title is recorded, but nothing is quoted from it, not even in the Bencao Gangmu, published later that century, which carried quotations from his other monograph on ginseng (19). A search for clinical research on moxibustion in the Journal of Traditional Chinese Medicine (English-language edition, published for more than 15 years) revealed very few articles on moxibustion, and nearly all of the articles that mention this technique made use of it as an adjunct to acupuncture therapy. In the very few articles that mention moxibustion alone, the fact that it is "accepted by the patient" seems to be a key point in selecting its use (presumably, acupuncture is not sufficiently comfortable for the patients).
Still, moxibustion is a relatively common practice in China today, and its position in history may not be so poor as might be suggested by the quotes above. As to the use of artemisia for moxibustion, here is what Chinese Acupuncture and Moxibustion has to say:
Artemisia vulgaris is a species of chrysanthemum [it is in the same plant family]. The one produced in Qizhou is known as the best kind for moxa, as the climate and soil is good for its growth. The leaves of Qizhou Artemisia are thick with much more wool [soft fibers]. Moxa cones and sticks made of this kind of artemisia are thought to be the top quality used in moxibustion. In A New Edition of Materia Medica appears the following description: "The moxa leaf is bitter and acrid, producing warmth when used in small amount and strong heat when used in large amount. It is of pure yang nature, having the ability to restore the primary yang from collapse. It can open the 12 regular meridians, traveling through the three yin meridians to regulate qi and blood, expel cold and dampness, warm the uterus, stop bleeding, warm the spleen and stomach to remove stagnation, regulate menstruation, and ease the fetus....When burned, it penetrates all the meridians eliminating hundreds of diseases." Yang can be activated by the Artemisia leaf for [because of] its warm nature. The acrid odor [spicy fragrance] of the leaf can travel through the meridians, regulate qi and blood, and expel cold from the meridians, and its bitter nature resolves dampness. As a result, it is used as a necessary material in moxibustion treatment.
Artemisia leaf is also selected for its ability to burn slowly and project heat through the wool in a gentle manner. But the important thing to note in this context is that this description is not a simple depiction of applying heat: it is about applying artemisia specifically. Unless this is understood to be entirely spiritual, in the sense that something mysteriously travels from the mugwort into the body, it must be understood that some of the mugwort vapors and smoke have their effect by entering the body, either through the skin where the moxa is burned or through breathing the fumes, or both. The heat is also important, but, if one is to believe the traditional sources, it is not the sole function. According to the authors of Manual of Dermatology in Chinese Medicine:
Moxibustion is an important and perhaps underutilized therapeutic method in traditional Chinese medicine. It may be used alone or in combination with other modalities, such as acupuncture....This method involves the burning of moxa on or above the skin at the location of specific acupoints, or on or near the lesion [to be treated] itself. The heat of the cauterization, as well as the properties of the moxa itself, serve to warm the qi and blood in the channels, expel cold and dampness, restore yang, and, in general, help to regulate the organs and restore health.
Detailing the functions of moxibustion, Chinese Acupuncture and Moxibustion (15) says that it is used:
The relationship of moxibustion to the herbal material used for moxa wool depends on the technique. For example, when moxa cones are burned on the end of acupuncture needles, the constituents of the moxa do not interact with the skin and the local effect is that of transferring heat to the acupoint. When a moxa pole is used, there is some transfer of active constituents to the skin, but not much; the effect is still mostly heat, but to a broader area. When the moxa cone is burned directly on the skin, active constituents are transferred to the skin. This latter method was the most commonly used traditional approach, as best as one can tell from the old literature. When moxa is burned on top of another herbal material, such as a slice of ginger or garlic, cake of aconite, or mound of salt or powder of herbs in the navel, the heat will drive some of the ingredients of the interposing herbal material into the skin, but little of the moxa wool ingredients will penetrate. Fresh ginger, one of the commonly used interposing materials, contains compounds similar to borneol and camphor (small holes in the slice of ginger or slice of garlic permit a little of the moxa vapors to penetrate). Of course, with all moxibustion techniques, the smoke and vapors from the moxa are ultimately inhaled. The modern smokeless moxa poles are intended to eliminate this otherwise sure route to getting moxa ingredients internally, and might defeat part of the therapeutic action. The Chinese technique of applying moxibustion for an extended period of time (up to 30 minutes for a treatment session), assures that the patient inhales a substantial amount of the vapors and smoke.
The different styles of moxa application and the method of Keeping-fit Moxibustion (the fourth application listed above) was elaborated by Yuan Liren and Liu Xiaoming (16), though with reliance on different points, namely shenque [CV-8], zhongwan [CV-12], yongquan (KI-1], and zusanli [ST-36], the latter point was mentioned above and is a standard for many acupuncture and moxibustion treatments. According to the authors, these points are selected and treated as follows:
Zusanli [ST-36]: Frequent moxibustion on zusanli can invigorate the spleen and stomach, assist in digestion, and hence, strengthen the body and slow down the process of aging. Some ancient experts advocated the use of scarring moxibustion, placing moxa wool directly on the skin over the point so that a scar is formed after the local skin has developed a boil with pus. Constant application of scarring moxibustion will maintain the moxibustion boil, and this will help to strengthen the body and prolong life. Another similar method, known as hanging moxibustion, is composed of hanging an ignited moxa stick 3-7 centimeters over the point without touching the skin for 5-10 minutes.
Shenque [CV-8]: Frequent moxibustion on this point can replenish qi and strengthen the body; it is especially suitable for the middle-aged and elderly. The particular procedure of this kind of moxibustion is as follows: put some salt on the navel, knead some moxa wool into the shape of a cone to be ignited and placed on the salt for moxibustion. The size of the moxa cone should vary with the individual conditions. For people of strong constitution, use big cones in the size of a broad bean and for those of weak constitution, use the middle-sized cones as big as a soybean or use small cones in the size of a wheat grain. The burning up of one moxa cone is referred to as one zhuang. Moxibustion on shenque point requires 7-15 zhuan g .
Zhongwan [CV-12]: This point is an important point for reinforcement, capable of strengthening the spleen and stomach. Both moxa stick and moxa cone are advisable for moxibustion on this point, the duration of which may last 5-10 minutes.
Yongquan [KI-1]: Frequent moxibustion at this point can strengthen the body and contribute to longevity, for it replenishes the kidney and invigorates yang. When using moxa sticks for moxibustion, it should last 3-5 minutes, and in the case of using moxa cones, 3-7 cones are usually needed each time.
The authors state that the duration of moxibustion should be at least 3-5 minutes, but not more than 10-15 minutes. A relatively longer duration of treatment is indicated for recovery from a serious disease or injury to recapture good health, in autumn and winter, on points of the abdomen (i.e., CV-8 and CV-12), and when treating young and middle-aged adults. Relatively shorter duration of treatment is indicated for simple health maintenance and longevity promotion, for spring and summer treatments, when applying moxibustion to the limbs (i.e., KI-1 and ST-36), for the aged and for children. They caution that:
The aim of strengthening the body and achieving longevity cannot be achieved by just applying moxibustion once or twice, for it requires persistence for a long time. This does not mean that one should receive moxibustion every day. For the purpose of convalescence for the weak and sick, the moxibustion may be applied once every 2-3 days in the early stage; yet for reinforcement of the body or longevity, it should be once a week in the early stage. And when it has shown some effect, the frequency can be reduced to once a month, and later, once or twice every three months, or even once or twice a year. So long as the practice is persisted in, good effect is sure to ensue.
A treatment along these lines was described by Song and Zhu (17) in one of the few articles on moxibustion in the Journal of Traditional Chinese Medicine. They treated 97 patients with gastric spasms or intestinal spasms with moxibustion, relying primarily on the abdomen points CV-8 (along with ST-37 for intestinal spasm) and CV-12 (along with ST-34 for gastric spasm). The secondary points surrounding ST-36 were picked because of the intent to treat an acute symptom, but the function is similar. The authors report that nearly all the patients had their abdominal pain alleviated with one treatment. The technique used was:
The moxa roll was ignited and placed over the selected points to produce a comfortable warm feeling. When the heat became excessive, the moxa roll was moved around the points or a little higher to avoid burns. A piece of gauze could be laid over the point to protect the skin from accidental injury. 30 minutes constituted one session of treatment.
Today, especially in the West, herbal moxibustion is sometimes substituted by heat lamps or other techniques that eliminate the artemisia altogether. This may change the functions of moxibustion in a way that is not known. Also, many traditional moxa specialists believed that blistering of the skin was essential to the success of moxibustion when treating serious ailments, much the way that getting the qi reaction to needling was deemed essential to getting success with acupuncture therapy. This method is even mentioned in relation to Keeping-fit Moxibustion, which is for preventive health care. Such intensive moxibustion is avoided in the Western practice, which follows more closely the method used for the gastric and intestinal spasm treatments, though most Westerners use very brief rather than prolonged moxa therapy (in the study mentioned above, the duration of treatment was about 15 minutes per point at two points to yield a 30 minute moxa session). One theory of the effects of moxibustion and acupuncture is that the local tissue damage (twisting of nerve fibers when stimulating acupuncture needles, extended cellular damage by the intense heat of moxibustion) initiates a non-specific healing reaction that can have effects throughout the body. Modern techniques of acupuncture and moxibustion therapy may rely, instead on mechanisms of stimulation that do not depend on tissue damage. However, it must also be recognized that some modern techniques may do little more than comfortably warm the skin and help induce general relaxation.
An additional impact of moxibustion may be to help sterilize the atmosphere of the rooms in which it is being used. In China an incense made of artemisia and atractylodes (cangzhu), when burned in an outpatient operation room, would reduce the bacterial count in the air. It also apparently inhibited viruses. According to Chinese evaluations, it could be used in kindergartens and nurseries to reduce the transmission of diseases, including chicken pox, mumps, scarlet fever, common cold, and bronchitis. Thus, when used in an acupuncture clinic, the smoke from moxibustion might help to prevent transmission of disease from one patient to another, which is especially important when dealing with immune-compromised patients.
Artemisia is a significant part of the tradition of preventing and treating diseases by warding off demons (see Disorders caused by "demons" ). This report was provided by Smith and Stuart:
As this plant [artemisia] is so frequently used as a charm, and is held in a measure of superstitious veneration by the people, it is a little difficult to determine just where its remedial use in native therapeutics begins. At the time of the Dragon Festival (fifth day of the fifth moon), the Artemisia is hung up to ward off noxious influences. This is done either together with a Taoist charm, in which case it is called aifu and is hung at the head of the principal room of the house, or together with the Acorus calamus (changpu) at the door; the leaves of the latter being formed in the shape of a sword (called puchien) and placed over the door, while the stalk of the artemisia is hung on each door post. That this was efficacious in at least one instance was attested by the fact that the famous rebel Huang Ch'ao gave orders to his soldiers to spare any family that had Artemisia hung up at the door. The moxa is employed by Buddhist priests in initiating neophytes; three rows of three, four, or five scars each being burned on the crown of the head with this substance. Many also use the moxa on a three day old child, burning one or more scars on the face; this being supposed to insure the child's living through infancy. The places of burning are between the brows, on each cheek a little distance beneath the eyes, and at the root of the nose on the upper lip.
The uses of artemisia by the Chinese find a remarkable parallel with that of the Native Americans. Probably the most commonly used herb for dispelling demons is the one we often refer to as "wild sage" but is actually artemisia. The following descriptions come from Uses of Plants by the Indians of the Missouri River Region (18), including mention of simple herbal remedies with demon-dispelling approaches:
Artemisia gnaphalodes (wild sage): A decoction of the plant was taken for stomach troubles and many other kinds of ailments. It was used also for bathing. A person who had unwittingly broken some taboo or had touched any sacred object must bathe with Artemisia. The immaterial essence or, to use the Dakota word, the to, of Artemisia was believed to be effectual as a protection against maleficent powers; therefore, it was always proper to begin any ceremonial by using Artemisia in order to drive away any evil influences. As an example of the use among the Omaha of Artemisia, to avert calamity it is related that two horses ran wild in the camp, knocking down the Sacred Tent. Two old men, having caught the horses, rubbed them all over with wild sage, and said to the young son of the owner, "If you let them do that again, the buffaloes shall gore them." In the ceremonies of the installation of a chief among the Omaha, wild sage was used as a bed for the sacred pipes....It has already been mentioned that various species of Artemisia were used in old times as incense for the purpose of exorcising evil powers. It has also been stated that cedar twigs or sweet grass, either one, were used as incense to attract good powers. Some Christian Indians also still employ all these species as incense for these specific purposes, in church services, especially at Christmas, Easter, Pentecost, and on occasion of funerals. The writer has seen the use of Artemisia as an incense before a church door just before the body was carried into the church. A small fire was made before the steps of the church, Artemisia tops being used to raise a cloud of smoke.
Some species could be used for attracting good, not just repelling evil:
Artemisia dracunculoides (fuzzy-weed): Among the Winnebago the chewed root was put on the clothes as a love charm and hunting charm. The effect was supposed to be secured by getting to windward of the object of desire, allowing the wind to waft the odor of the herb thither. The Omaha ascribed the same powers to this species and used it in the same ways as they did the gray species of this genus [see above]. It was used also in smoke treatment. A Winnebago medicine-man said a handful of the tops of this species dipped into warm water served as a sprinkler for the body to relieve fevers. According to a Pawnee informant, a decoction made of the tops was used for bathing as a remedy for rheumatism....
Sweetgrass, often used with wild sage, is described thus:
It was used for perfume and was burned as an incense in any ceremony or ritual to induce the presence of good influences or benevolent powers, while wild sage, a species of Artemisia, was burned to exorcise evil influences or malevolent powers.
Aside from any mystical essence that Artemisia might possess, the unifying feature of the Chinese and Native American uses of this plant is its smoke and accompanying fragrance. This is, to a large extent, the heavenly fragrance of borneol.
Borneol was also used in Chinese internal remedies for treating demon-caused diseases. These remedies were made up of the most rare and auspicious materials. Two examples should illustrate the point:
Angong Niuhuang Wan
Rare animal components: ox gallstones, rhino horn, musk, pearl
Alchemical mineral components: gold, realgar, cinnabar
Herbal components: borneol, coptis, scute, gardenia, curcuma
Zhi Bao Dan
Rare animal components: ox gallstone, rhino horn, tortoise shell (daimao), musk
Alchemical mineral components: gold, silver, realgar, cinnabar
Herbal components: borneol, benzoin, succinum
These formulas were applied for delirium, coma, and convulsions-conditions that were thought (by many) to occur because demons penetrated the body. Using the more commonly relied upon descriptions of the medicinal materials and their actions, these substances opened blocked orifices (e.g., borneol, musk, benzoin, and ox gallstone), calmed agitation (succinum, cinnabar, pearl), and removed heat toxin (coptis, scute, gardenia). However, one can see by the selection of the particular materials, that these were "precious pills" relied upon for the disorders that were beyond the usual experience.
September 1998