CHECKING FOR POSSIBLE HERB-DRUG INTERACTIONS
The issue of herb-drug interactions looms large over the practice of herbal medicine. Up to now there have been very few incidents recorded of herb-drug interactions, but since the first such reports emerged a decade ago, a concern has been raised: that we know so little about herbs and their potential for interaction with drugs that these incidents could be just the "tip of the iceberg." Virtually all medical writers who review the literature acknowledge the small number of reports, but conclude that the issue of herb-drug interactions is a serious one that must be pursued. In a few instances, the interactions may have been responsible for severe consequences.
As described in a previous article (The interactions of herbs and drugs, 2000 START Manuscripts), the nature of herb-drug interactions is not a chemical interaction between a drug and an herb component to produce something toxic. Instead, the interaction may involve having an herb component cause either an increase or decrease in the amount of drug in the blood stream. A decrease in the amount of drug could occur by herb components binding up the drug and preventing it from getting into the blood stream from the gastrointestinal tract, or by stimulating the production and activity of enzymes that degrade the drug and prepare it for elimination from the body. An increase in the drug dosage could occur when an herb component aids absorption of the drug, or inhibits the enzymes that break down the drug and prepare it for elimination. A decrease in drug dosage by virtue of an interaction could make the drug ineffective; an increase in drug dosage could make it reach levels that produce side effects. Alternatively, an herb might produce an effect that is contrary to the effect desired for the drug, thereby reducing the drug effect; or, an herb might produce the same kind of effect as the drug and give an increase in the drug effect (without increasing the amount of the drug).
Examples of concerns about herb-drug interactions that have been raised are that an herb might:
Such responses can occur with drug-drug interactions and with food-drug interactions, so the finding of some instances of herb-drug interaction would not be surprising.
In China it is common for herbs to be combined with drugs. Their combination is sometimes incidental, but is often intentional and based on a prevalent favorable theory about using herbs and drugs. The general sense of the situation among Chinese doctors has been that herbs reduce the side effects of drugs and help them to perform their function better; in turn, drugs will make an herb formula work more strongly and quickly. Together, herbs and drugs may produce a more desirable result than either taken alone. As an outcome of working within this scenario, little attention has been paid to adverse herb-drug interactions.
The Chinese culture is one in which herbs were a dominant medical therapy during the 20th Century, and drugs were a relatively recent addition to the medical field. The situation was different in the West. Herbs had been almost entirely replaced by drugs during the 20th Century, and were later reintroduced once drugs had become a dominant feature of modern health care. In the West, the replacement of herbs by drugs took place over a period of many decades during which there was a prevailing attitude that drugs were more reliable than herbs. The re-introduction of herbs brings with it suspicions and concerns about their unreliability and the lack of adequate knowledge about them.
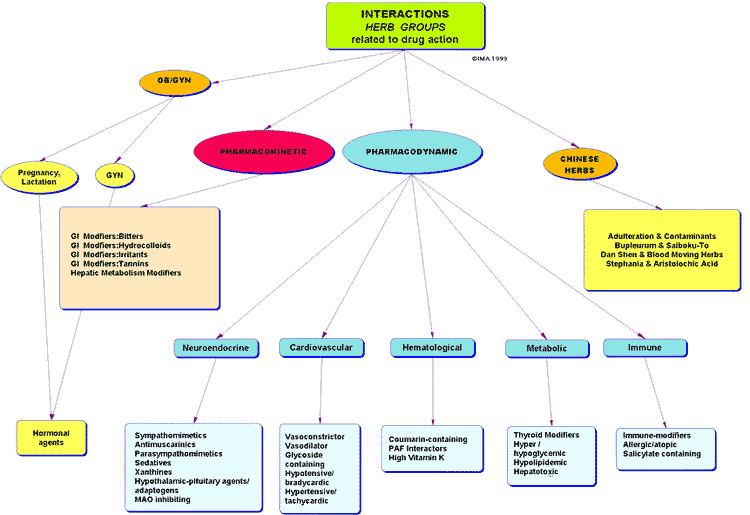
Today, doctors and pharmacists are provided courses and educational materials outlining potential problems with herbs that their patients may be using. The matter of herb-drug interactions involves a considerable amount of speculation about what might happen, based on knowledge-which is also quite limited-about drug-drug interactions and food-drug interactions. An example presentation to doctors is the following chart, produced in 1999 and presented by Jerry Cott, a neuropsychopharmacologist:

This chart first divides interaction concerns into broad subgroups, the main ones being related to pharmacodynamic interactions (mostly involved with herbs and drugs yielding similar effects or counteracting one another) and pharmacokinetics (such as changing the rate of absorption or elimination of a drug). There are also two specialty groups: therapies involving obstetric/gynecological/hormonal matters and Chinese herbs. Very little information about actual interactions is imbedded in the presentation. There is mention of "xanthines" (e.g., caffeine) under neuroendocrine, reflecting the concern that caffeine containing herbs (e.g., coffee and tea) could counteract the action of sedatives or produce excessive stimulation with stimulant drugs. Under the cardiovascular heading, there is mention of "glycoside-containing." The intended meaning is the specific class of cardiac-glycosides, as there are abundant glycosides that don't have significant cardiac effects (whereas, the cardiac glycosides are often quite potent, and can not only enforce or counteract the action of cardiac drugs but can themselves cause cardiac problems if the dosage is large). Generally, the field of herbal medicine has been purged of ingredients with cardiac glycosides; there remains a concern that one of the cardiac glycoside-containing herbs will find its way into a product by mistake. Under the heading hematological, there is mention of "coumarin containing," which makes reference to the fact that some herbs contain coumarins which might act along with Warfarin, a coumadin (binary coumarin, much more potent than coumarins), or along with other blood thinners. The table also makes passing mention of tannins (an herb component with several health benefits that can bind up drugs in the intestinal tract and make them less available). Under Chinese herbs, there is mention of three issues: the possible interaction of Minor Bupleurum Combination (Xiao Chaihu Tang; in Japan: Sho Saiko To) with interferon in treatment of hepatitis to cause an immune response leading to lung damage; the possible interaction of salvia (danshen) and Warfarin, leading to excessive blood thinning; and the possible interaction of aristolochic acid and diuretic drugs (or others) to cause renal failure. Other than these few specific examples (all of which have been addressed by previous START articles), the chart outlines areas of concern, but not necessarily known problems.
Due to the paucity of actual reports of herb-drug interactions, lists of herb-drug interactions are usually padded with other information, such as reports of simple adverse reactions (not involving interactions). A table provided to pharmacists of this nature is shown here; it is by Pharmacists Planning Service, Inc.
|
Name of Herb |
Some Common Uses |
Possible Side Effects or Drug Interactions |
|
|
External: used for muscle spasm and soreness |
External: potential for skin ulceration and blistering with greater than 2 days of use. Internal: overuse may cause severe hypothermia. |
|
|
Echinacea boosts the immune system and helps fight colds and flu. Aids wound healing. |
Echinacea may cause inflammation of the liver if used with certain other medications, such as anabolic steroids, methotrexate or others. |
|
|
Ephedra is also called Ma-Huang. It is used in many over-the-counter diet aids as an appetite suppressant. It is also used for asthma or bronchitis. |
Ephedra may interact with certain antidepressant medications or certain high blood pressure medications to cause dangerous elevation in blood pressure or heart rate. It could cause death in certain individuals. |
|
|
Feverfew is used to ward offf migraine headaches and for arthritis, rheumatic disease and allergies. |
Feverfew may increase bleeding, especially in patients already taking certain anti-clotting medications. |
|
|
Garlic is used for lowering blood cholesterol, triglyceride levels and blood pressure. |
Garlic may increase bleeding, especially in patients already taking certain anti-clotting medications. |
|
|
Ginger is used for reducing nausea, vomiting and vertigo |
Ginger may increase bleeding, especially in patients already taking certain anti-clotting medications. |
|
|
Ginkgo, also called ginkgo biloba, is used for increasing blood circulation and oxygenation and for improving memory and mental alertness. |
Ginkgo may increase bleeding, especially in patients already taking certain anti-clotting medications. |
|
|
Ginseng increases physical stamina and mental concentration. |
Ginseng may cause decreased effectiveness of certain anti-clotting medications. Persons using ginseng see increased heart rate or high blood pressure. It may cause bleeding in women after menopause. |
|
|
Goldenseal is used aas a mild laxative and also reduces inflammation. |
Goldenseal may worsen swelling and/or high blood pressure. |
|
|
Kava-kava is used for nervousness, anxiety or restlessness; it is also a muscle relaxant. |
Kava-kava may increase the effects of certain anti-seizure medications and/or prolong the effects of certain anesthetics. it can enhance the effects of alcohol. It may increase the risk of suicide for people with certain types of depression. |
|
|
Licorice is used for treating stomach ulcers. |
Certain licorice compounds may cause high blood pressure, swelling or electrolyte imbalances. |
|
|
Saw Palmetto is used for enlarged prostate and urinary inflammations. |
People using saw palmetto may see effects with other hormone therapies. |
|
|
St. John's Wort is used for mild to moderate depression or anxiety and sleep disorders. |
St. John's Wort may prolong the effect of certain anesthetic agents. |
|
|
Valerian is used as a mild sedative or sleep-aid. It is also a muscle relaxant. |
Valerian may increase the effects of certain anti-seizure medications or prolong the effects of certain anesthetic agents. |
References to what the herbs "may" do when combined with certain drug groups, (e.g., valerian may increase the effects of certain anti-seizure medications or prolong the effects of anesthetic agents) often refer to pharmacology studies rather than actual clinical experience. For example, when one wishes to demonstrate that valerian, used traditionally for seizures and for analgesic effects, is likely to accomplish what has been claimed, laboratory animal studies are conducted. A standard procedure is to test the herb extract alone and to also test it with drugs that cause the same effect. If the drug effect is increased or prolonged by the herb, it is implied that the herb has a similar effect, even though it may have a different mechanism. Thus, a study intended to demonstrate that a traditional claim for an herb is true turns out to be a source of worry about herb-drug interactions. However, the amount of herb used in the pharmacology experiments of this type is often far higher than the amount normally used in clinical practice; the likelihood of herb-drug interactions occurring with normal use of the herb may be minimal. Still, if one wishes to consider possible herb-drug interactions under a variety of scenarios, including excessive use of the herb and use of the herb by individuals who are more sensitive to the possible interaction, then such data must be included.
When published reports alluding to adverse herb reactions (but not interactions) and to pharmacology studies only are eliminated, one is left with few instances of reported herb-drug interactions. This is likely due to the low dose of any individual herb component usually consumed and the simple absence of significant interaction at any reasonable dose. To help illustrate the low frequency of clinical reports, the following abstract of a recent publication will be informative:
Drug-herb interaction among commonly used conventional medicines: a compendium for health care professionals.
Brazier NC, Levine MA.
Center for Evaluation of Medicines and McMaster University, Hamilton, Ontario, Canada.
In: American Journal of Therapeutics 2003; 10(3): 163-169.
The objective of the review was to consolidate the clinical and pharmacologic aspects of drug-herb interactions to develop a compendium of information to provide prescribers with a measure of the risk of interactions, a description of the clinical consequences, and an assessment of the quality (i.e., validity) of evidence. A variety of electronic databases and hand-searched references were used to identify documentation of interactions between herbal products and drugs from the most commonly used therapeutic classes. MEDLINE, Allied and Complementary Medicine Database, CINHAL, HealthSTAR, and EMBASE were searched from 1966 to the present. One hundred sixty-two citations were identified. Only 22 citations met the inclusion criteria. Using a matrix of 165 possible drug-herb interaction pairs (15 therapeutic drug classes by 11 herbal products), we identified 51 (31%) interactions discussed in the literature. Twenty-two of these 51 drug-herb pairs (43%) were supported by randomized clinical trials, case-control studies, cohort studies, case series, or case studies. The remaining interaction pairs reflected theoretic reasoning in the absence of clinical data. Most interactions were pharmacokinetic, with most actually or theoretically affecting the metabolism of the affected product by way of the cytochrome P450 enzymes. In this review, Warfarin was the most common drug and St. John's Wort was the most common herbal product reported in drug-herb interactions. To create a comprehensive and valid list of herb-drug interactions would require a substantial increase in research activities in this area. Improvements in the quality of methodology used are also necessary.
| Put simply, there were very few well-supported interactions detected: namely 22 that involved more than an individual report, or a simple pharmacology study, or a mere suggestion of potential interaction. Not surprisingly, the main drug of concern is Warfarin, which displays substantial sensitivity to interactions with foods and drugs, and which is very widely used (giving more opportunities to note interactions), while the primary herb involved is St. John's Wort, one with unique constituents (here is a chemical diagram of hypericin, one of the components) known to affect the drug metabolizing enzymes (such as cytochrome P450, mentioned in the abstract). Use of St. John's Wort declined dramatically after revelations that it could cause herb-drug interactions along with reports questioning its effectiveness. | 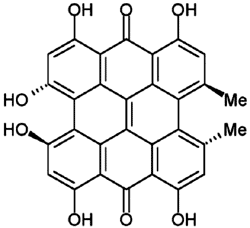
|
In an earlier survey of similar nature (1), an intensive search of the literature and evaluation of reports of herb-drug interactions yielded the following: "108 cases of suspected interactions were found: 68.5% were classified as 'unable to be evaluated,' 13% as 'well-documented' and 18.5% as 'possible' interactions. Warfarin was the most common drug (18 cases) and St. John's Wort the most common herb (54 cases) involved." Thus, 14 cases were well-documented in this report published about 2 years earlier than the new report which found 22 reasonably supported cases. The same drug and herb emerged as problematic. The rate of well-documented herb-drug interactions has been about 4 per year. No doubt, many more instances occurred and were not reported due to their minor nature or uncertainty about the cause. Even so, the numbers should be kept in perspective: the nutriceutical industry estimated (1999) that about 45 million American adults use an herbal supplement at least once per year, and that 21 million adults are regular users of herbal remedies.
If a patient merely asks you to assure that the herbs you prescribe will not interact or be a problem with a drug regimen being used at the same time, it is not possible to give such assurances. It is reasonable to relay the low incidence of herb-drug interactions and to offer the methods of minimizing herb-drug interactions (e.g., not taking the herbs and drugs at the same time; monitoring for potential interactions by maintaining routine testing, such as blood coagulation tests given to users of Warfarin). However, a practitioner with internet access can also offer to check the most recent literature for reported herb-drug interactions. To do so will require an accurate listing of the drugs being used.
Not all suspected cases of herb-drug interactions are published. However, in order for a suspected case to be published, it usually has to be formally written up by a doctor involved in the case, submitted to a journal, and reviewed by other doctors or researchers who are familiar with this subject area. Publication of a suspected case does not mean that the herb-drug interaction definitely occurred, but it does mean that the case was presented in a manner considered consistent with the modern standards for reporting such incidents. Current standards for many journal reports are inadequate, as indicated by the literature reviews.
All major medical journals, and many minor medical journals, have their articles listed-and often abstracted-in a huge database maintained by the National Center for Biotechnology Information (NCBI) of the National Library of Medicine (NLM), a division of the National Institutes of Health (NIH). The information is posted for easy access on the internet, and this type of posting was one of the original uses of the internet (the earlier designation for the main part of the service was MedLine). The website where one accesses the information is now called Entrez-PubMed and its access address is:
http://www.ncbi.nlm.nih.gov/PubMed/This site (which can also be accessed through any search engine by typing in Entrez-PubMed and then following the first link) will provide a space into which the user may type the search terms, to yield a series of abstract titles, with access to abstracts (or fuller reference information when abstracts are not available). The procedure for checking herb-drug interactions is to type in:
As an example, one can type in:
Cyclosporin, herb-drug interactionsUpon hitting the return button of the keyboard or clicking on the "go" icon on the screen, the search is rapidly completed. In the example cited here, there are three abstracts-two reviews and one specific article-all mentioning the same herb. The relevant abstract is this one:
Hazardous pharmacokinetic interaction of Saint John's wort (Hypericum perforatum) with the immunosuppressant cyclosporin.
Mai I, Kruger H, Budde K, Johne A, Brockmoller J, Neumayer HH, Roots I.
Institute of Clinical Pharmacology, Charite University Medical Center, Humboldt University of Berlin, Germany.
International Journal of Clinical Pharmacology and Therapeutics 2000; 38(10: 500-502.
Contrary to common belief, over-the-counter herbal remedies may cause clinically relevant drug interactions. With the enclosed report we would like to alert other physicians that herbal extracts of Saint John's Wort (Hypericum perforatum) may cause a sudden remarkable decrease of cyclosporin trough concentrations. A kidney transplantation patient treated with 75 mg bid doses of cyclosporin for many years experienced a sudden drop in her cyclosporin trough concentrations. This change was in temporal relationship to hypericum extract co-medication, and a re-challenge gave similar results….The potential clinical consequence of this pharmacokinetic herb-drug interaction is apparent, since low cyclosporin levels are associated with an increased risk of rejection after organ transplantation and are usually not suspected upon intake of plant products….
In most instances, when checking a drug for interactions, the page will display the following:
No items found.
The small number of reports of specific herb-drug interactions is the reason for getting this as a typical result. Even if one enters: Warfarin, herb-drug interactions, one will find only a few responses: some review articles (including the two cited above), and a specific report, such as a case involving an apparent interaction with boldo-fenugreek. The review articles indicate that interactions (increased blood thinning effect, with bleeding) are suspected or found for Warfarin with ginkgo (referring to the leaf), garlic, tang-kuei (danggui; sometimes spelled dong quai), and salvia (danshen). The potential for interactions has been confirmed with laboratory studies. However, such interactions are dose dependent, and it remains unclear what dosage might cause a problem. Since tang-kuei and salvia are widely used in Chinese medicine and used at widely varying dosages (from a few milligrams of powder to several grams in decoction), it would be helpful to know what dose might cause the effect; this remains undocumented. In a pharmacology study of salvia and Warfarin, the dose of salvia given to laboratory rats was 5 grams/kg body weight; this is a huge dosage. However, cases of patients experiencing bleeding when taking Warfarin and salvia have been informally reported.
If a report of interaction appears, it is important to check the abstract (when provided) for details to confirm that there is an actual report of herb-drug interaction (as with the St. John's Wort case above) rather than merely a concern raised. Also, once an herb-drug interaction report is found in the first search, a new search should be performed, specifying the herb and the drug in the search box (not just the drug name and general area of herb-drug interactions). For example, if one types in the entry-Warfarin, salvia-there are additional reviews, plus some reports on this specific interaction. One of the reviews expands the list of herbs that may reinforce the anticoagulant action of Warfarin to include ganoderma, papaw, ginseng, devil's claw, quinine, ginger, red clover, and horse chestnut. Two laboratory animal reports aimed at the study of Warfarin-salvia interactions appeared in this search. No individual clinical reports of the interaction were among those listed, so it remains unclear whether the referenced cases of bleeding had been confirmed. If one tries the entry-cyclosporin, St. John's Wort-33 references replace the earlier search results of just 3. While many of the reports review the same cases, others are relevant to understanding the interaction, and still others mention additional cases of apparent interactions. St. John's Wort has been blamed for several instances of transplant rejection due to its lowering of cyclosporin concentrations.
There are more sophisticated searches that can be performed by listing more key words to try and capture more references on the first search. However, an easy method of pursuing the subject further is to click on the words "related articles" posted next to each abstract title.
Once a search has been conducted, the following can be conveyed to patients:
It is not advisable to give firm assurances that there can be no problem, but it is also not advisable to overstate the concerns. Most doctors will be satisfied to know that the drugs they have prescribed to their patient have been checked for herb-drug interactions by the herb prescriber. A good perspective has been offered in a recent abstract from an article about herb-drug interactions with cardiac drugs:
The prevalence of herb-drug interactions has been exaggerated. Nonetheless, some herbs, including garlic, ginkgo, ginseng, and St. John's Wort, can have a significant influence on concurrently administered drugs. Herbal medicines may mimic, decrease, or increase the action of prescribed drugs. This can be especially important for drugs with narrow therapeutic windows and in sensitive patient populations such as older adults, the chronically ill, and those with compromised immune systems
The herbs mentioned in this abstract are those suspected of interacting with Warfarin, a drug with a narrow therapeutic window often used by sensitive patient populations. These herbs are often provided in single-herb products where they are at a relatively large dosage. A small amount of ginseng-an herb that has not been clearly implicated in the Warfarin interactions-is unlikely to cause interactions.
As noted above, the drug with greatest concern for interactions is Warfarin, but there is also a concern for interaction with any blood-thinning drug. The following report abstract describes a survey at one institution that found some potential interactions between herbs and drugs, where blood thinning was the main issue:
Potential interactions between herbal medicines and conventional drug therapies used by older adults attending a memory clinic.
Dergal JM, et al., Applied Research Unit, Baycrest Centre for Geriatric Care, Toronto
In: Drugs and Aging. 2002;19(11):879-886.
OBJECTIVE: Herbal medicines and conventional drug therapies are often taken in combination. The objective of our study was to identify the range of natural health products and conventional drug therapies used by older adults (aged 65 years and over) attending a memory clinic, and to specifically evaluate the frequency of potential interactions between herbal medicines and conventional drug therapies. DESIGN: We interviewed consecutive patients attending the Memory Disorders Clinic at the Baycrest Centre for Geriatric Care, a University of Toronto teaching hospital, between 4 July and 15 August 2000. Patients were asked to bring to their appointment all natural health products (i.e., herbal medicines, vitamins and minerals) and conventional drug therapies (i.e., prescription and over-the-counter) they were currently using. We collected information on current and previously-used natural health products and current conventional drug therapies. Patients were classified as having the potential for an interaction if they were using a current herbal medicine in combination with a conventional drug therapy and the interaction had been reported previously in the medical literature. PARTICIPANTS: We interviewed 195 consecutive patients attending the Memory Disorders Clinic at the Baycrest Centre for Geriatric Care, Toronto, Ontario, Canada. RESULTS: Of the 195 patients in our sample, 33 (17%) were 'current users', 19 (10%) were "past users," and 143 (73%) were "never users" of herbal medicines. Among the 52 patients who were "current or past users," the most frequently used herbal medicines were ginkgo (Ginkgo biloba) [39 users], garlic (n = 10), glucosamine sulphate (n = 9), and echinacea (n = 8). Among the 33 patients who were current users, the most commonly-used herbal medicines were ginkgo (n = 22), glucosamine sulphate (n = 8) and garlic (n = 6). Among the 33 current users, we identified 11 potential herb-drug interactions in nine patients. The 11 herb-drug interactions we identified were between ginkgo and aspirin [n = 8], ginkgo and trazodone (n = 1), ginseng and amlodipine (n = 1), and valerian and lorazepam (n = 1). CONCLUSIONS: Herbal medicines are widely used. Almost one-third of current users of herbal medicines were at risk of a herb-drug interaction. The most common potential herb-drug interaction was between ginkgo and aspirin. This finding has important potential implications because both of these products are regularly used by older people. Physicians and other healthcare providers should be aware of potential herb-drug interactions and should monitor and inform their patients accordingly.
This report would seem to give a shocking result: that nearly one-third of herb users (at least, among this elderly population) were at risk for herb-drug interactions. Because these people were going to a memory clinic and because modern medicine has limited impact on memory disorders, many patients were taking ginkgo, which is claimed to be a memory enhancing herb.
A brief literature search turned up no formal journal reports giving details of interactions between aspirin and ginkgo, but there was a review article-Herbal medication: potential for adverse interactions with analgesic drugs (2)-which indicated that:
Non-steroidal anti-inflammatory drugs (NSAIDs), particularly aspirin, have the potential to interact with herbal supplements that are known to possess antiplatelet activity (ginkgo, garlic, ginger, bilberry, dong quai, feverfew, ginseng, turmeric, meadowsweet and willow), with those containing coumarin (chamomile, motherwort, horse chestnut, fenugreek and red clover) and with tamarind, enhancing the risk of bleeding. Acetaminophen may also interact with ginkgo and possibly with at least some of the above herbs to increase the risk of bleeding."
A mild antiplatelet activity for ginkgo has been proposed as one of its mechanisms for aiding circulation to the brain and, thereby, enhancing memory. The Complementary and Alternative Medicines Institute says of the potential for herb-drug interactions with ginkgo that (3):
Ginkgo inhibits platelet aggregation. Preferably avoid use in patients on antiplatelet (aspirin, dipyridamole, ticlopidine) or anticoagulant (Warfarin) therapy. Monitor bleeding time and prothrombin time (PT) if patient is taking ginkgo concurrently with antiplatelet or anticoagulant drugs. Ginkgo may increase the activity/toxicity of monamine oxidase inhibitors.
Since elderly patients are more susceptible to spontaneous bleeds due to weakness of capillaries as well as having a prolonged healing time for response to incidents, this caution would seem reasonable. However, unless the extent of anticoagulant activity of an herb is measured, it is difficult to know whether or not to prohibit use. It is firmly established that increased blood coagulation is a problem in modern society, especially among the elderly, and this problem often accompanies other circulation-related disorders. As a result, herbs that have anti-coagulant properties are generally attractive (e.g., garlic, ginkgo).
Researchers who are working to demonstrate the potential health value of herbs may be drawn to demonstrating the anti-coagulation potential for herbs during laboratory animal studies. These studies may not accurately reflect what happens in human clinical cases, because of dosage of herb (usually high in laboratory studies of this type) or the model used (coagulation of blood under circumstances different that occurs naturally in humans). Ginkgo antiplatelet activity cautions appear to be based on case reports that still require verification. In the review article Dietary Supplement-Drug Interactions (4), the author states: "several case reports document bleeding complications with Ginkgo biloba, with or without concomitant drug therapy." The suggestion here is that the antiplatelet activity of ginkgo is high enough that it can cause bleeding complications on its own. At least three cases of brain hemorrhage have been blamed on ginkgo (5).
To be safe, a practitioner would either not prescribe ginkgo to a regular user of NSAIDS, especially aspirin and particularly for the elderly patient. An added risk to the practitioner is that the patient would suffer a bleed that would be blamed (rightly or wrongly) on the interaction, and the practitioner "should have known and should have warned the patient." The problem of using herbs with anticoagulants was address by Robert Rountree in an article that appeared in Herbs for Health magazine (2001):
Millions of people regularly take blood-thinning drugs such Warfarin, and even more take aspirin and similar medications to prevent heart attacks and strokes. At the same time, with the use of herbal medicines more popular now than ever, surveys show that most people don't tell their physicians about their use of herbs or vitamin supplements.
Herbs may interact with the blood thinning drugs in different ways, some of them beneficial, some of them potentially harmful. Herbs that enhance the effect of the anticoagulants may have antiplatelet activity, meaning that they keep platelets from forming clots, or anticoagulant activity, meaning that they increase the time it takes a clot to form, usually because they contain a compound called coumarin. Other herbs may counteract the effect of anticoagulants by decreasing blood-clotting time, most likely because they contain a coagulant compound called berberine.
Meanwhile, physicians are starting to realize that many herbs possess potent pharmacological activity. Concerns have been raised in prominent medical journals that this activity could have detrimental effects, especially for patients taking certain types of medications. Cautious physicians have chosen the route of absolute avoidance rather than risk an adverse reaction, they recommend that patients stop taking herbs altogether. Is this rational policy? Or is there another approach somewhere in between? To better answer these question, let's look more closely at how anticoagulants, or blood thinners, work in the body.
Warfarin is the most commonly prescribed anticoagulant drug. Doctors typically give anticoagulant to people with high risk of blood clotting, such as those who have artificial heart valves, deep vein thrombosis (a large blood clot) in the legs, or arterial fibrillation (a chronic irregularity in heart rhythm). The process by which blood thickens into a clot involves a chain reaction: various proteins interact to produce thrombin, which then produces fibrin, the protein material that forms the clot's core. Several of these interacting proteins are made in the liver, where vitamin K is essential for their production. Warfarin inactivates vitamin K to limit clotting proteins, so it increases the amount of time it takes for blood to clot. This effect can be monitored with a simple blood test called the prothrombine time (PT).
Vitamin K is found in high concentrations in many foods, including dark green leafy vegetables (especially turnip greens), alfalfa sprouts, broccoli, asparagus, egg yolks and dairy products. Eating these foods increases the potential for higher blood levels of vitamin K, which would interfere with the anticoagulants, a few herbs also promote clotting, most notably shepherd's purse, possibly because it contains vitamin K.
Another aspect of blood clotting involves the clumping together of platelets: the combination of platelets clumps and the fibrin clot is what causes blood to thicken into full clots. Platelet function can be measured with the test called the bleeding time. Many antiplatelet drugs are commonly used in medical practice, primarily to prevent strokes and heart attacks. Aspirin is the most common antiplatelet agent; others include dipyridamole (Persantine), sulfinpyrazone (Anturane), clopidogrel (Plavix), and ticlodipine (Ticlid). Many herbs also inhibit platelet aggregation (see below). Undoubtedly the list will expand with further research.
| Activity | Commonly Used Herbs* |
| Anti-coagulant | chamomile, dong quai (tang-kuei), horse chestnut |
| Anti-platelet | bilberry, bromelain, cayenne, feverfew, flaxseed oil, garlic, ginger, ginkgo, ginseng, green tea, meadowsweet, motherwort, and turmeric |
| Pro-coagulant | goldenseal, Oregon grape root, shepherd's purse |
| *To expand the list of anticoagulant and antiplatelet herbs, the following are mentioned in Pharmacology and Applications of Traditional Chinese Medicine (6): white atracytlodes, cnidium (chuanxiong), salvia, garlic, zedoaria, pueraria, carthamus, lysimachia, cinnamon bark, tien-chi (sanqi), and capillaris (also listed: tang-kuei and turmeric). | |
If using anticoagulants has impaired a person's normal clotting mechanism, good platelet function is obviously an important backup system. Otherwise, a minor injury could lead to a severe hemorrhage. Or, if you are taking antiplatelet drugs everyday, the addition of ginkgo or one of the herbs listed in the first two sections of the chart above could lead to uncontrolled bleeding.
So what is an informed person to do? Well, there are several options, depending on the degree of effort one is willing to put out. As a start, I propose the following step by step method.
Given the increasingly large number of people taking complex mixtures of herbs, vitamins and drugs, it's probable that we will see more reports of side effects and negative interactions. Some authorities are using these incidents to discourage the public from taking herbs. But rather than turning back the clock on herbal medicine, I propose learning from these examples and upgrading our database of medical information.
Fugh-Berman A, Ernst E, Herb-drug interactions: review and assessment of report reliability, British Journal of Clinical Pharmacology 2001, 52(5): 587-595.
September 2003