SAFETY ISSUES AFFECTING HERBS:
Herbs That May Increase Blood Pressure
Patients with hypertension are cautioned by their doctors to be very careful about keeping their blood pressure within acceptable limits, and this is often accomplished with drug treatments as well as through efforts to control diet and get sufficient exercise. Blood pressure can vary markedly from test to test as a result of numerous circumstances, including eating food, any physical activities just prior to taking the measurement, and the emotional state of the individual (accounting for what has been called "white coat hypertension"-elevation of blood pressure due to stress when visiting the doctor). For this reason, blood pressure measurements are usually taken before meals, after resting for a while, and when the patient is calm.
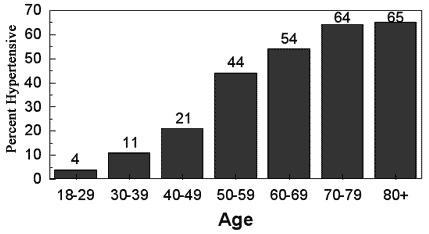
Prevalence of Hypertension in U.S. Adult Population

When people with hypertension are given herbs, a high blood pressure reading after starting the regimen may bring suspicion that the herb therapy provoked a reaction. A single reading is not reliable, but practitioners should be able to advise their patients appropriately about the potential for the herb to be involved in a blood pressure change. Very few medicinal herbs have been noted to cause an increase in blood pressure: the most frequently cited cases being ephedra (ma-huang, Ephedra sinensis) and licorice. Ephedra has potent alkaloids, mainly ephedrine, that can stimulate the nervous system and endocrine system to generate an acute rise in blood pressure. Ephedra has been removed from most consumer products due to concerns about its effects. Licorice contains triterpene glycosides, including glycyrrhizic acid, that can increase the sodium content of blood and thereby gradually increase blood pressure.
Sometimes herbs are held responsible for hypertensive actions as a result of unusual dosing patterns. For example, licorice can cause significant hypertension when used in high doses, such as when a person binges for several days on licorice candy made from real licorice. It is rare to have such a reaction from normal doses of licorice in Chinese herb formulas, where licorice doses in long-term therapies tend to be low. In one case of a hypertension reaction to licorice recently recorded in the medical literature (1), "a detailed history revealed that an elderly man had ingested tea flavored with 100 grams of natural licorice root containing 2.3% glycyrrhizic acid daily for 3 years." It has been clearly demonstrated that licorice ingestion can cause adverse reactions even at much lower levels of licorice consumption than this (see further explanation below). As another example, ginseng, which lowers blood pressure at normal dosages about 3-4 grams per day, is used in China to treat shock (a sudden drop of blood pressure) given at 30 grams for a dose or given by injection. The reference to the treatment method for shock, where very high-dose ginseng restores normal blood pressure, should not deter the ordinary use of ginseng as a health promoting tonic.
Recently, a listing of herbs that "provoke hypertension" was compiled for a symposium in Seattle sponsored by the American Academy of Family Physicians (Clark, 2003). This is the list (2):
| Aniseed St. Johns Wort Capsicum Parsley Blue Cohosh | Vervain Chaste Berry Bayberry Licorice Ginger | Ginseng Ephedra Pau d'Arco Coltsfoot Gentian | Cola alkaloids Broom alkaloids Calamus amines Guarana |
Four of the herbs are used routinely in Chinese medicine: ma-huang, ginseng, and licorice, and ginger. In addition, coltsfoot is occasionally used; and there is a Chinese gentian and a Chinese vitex (chaste berry) that might have the same properties as the Western ones. Cola alkaloids refer to caffeine and related compounds (called xanthines), and this is the main ingredient in guarana (used as a caffeine source). Broom alkaloids refer to Cytisus scoparius (Scotch Broom), which contains the hypertensive alkaloid sparteine.
The reports on hypertensive action for several of the herbs are quite limited and may not apply at all to what happens with normal clinical use. As an example, coltsfoot (tussilago) contains pyrrolizidine alkaloids (see: Safety Issues Affecting Herbs: The Case of Pyrrolizidine Alkaloids), and the herb has been banned from use in Europe due to its content of these alkaloids. These components do not, in themselves, cause hypertension. Excessive consumption of pyrrolizidine alkaloids (PAs), especially in infants and young children, can cause liver damage, which, in turn, can produce hypertension. Thus, the relationship of coltsfoot to hypertension is not that it is a hypertensive agent but that in rare cases where liver damage occurs from its excessive use, the damage provokes hypertension (in the one case reported, it was reversible damage). The story is even more complicated. While it is true that coltsfoot contains PAs, the herb in the reported case of hypertension had been gathered by the child's parents, but another herb with higher concentration of PAs, Adenostyles alliariae (alpendost), had been administered mistakenly (3). Hence, the listing of coltsfoot in this table is actually erroneous.
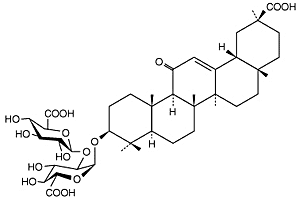
Regarding licorice ingestion, the effect is understood to be entirely due to increased renal sodium retention. The active compound of licorice, glycyrrhizic acid (GA), is hydrolyzed in the body to form glycyrrhetinic acid, which inhibits renal 11beta-HSD2 (a steroid metabolizing enzyme) and by that mechanism increases access of cortisol to its receptors to produce renal sodium retention and potassium loss (4). In a study to find the dosage-response relationship, healthy volunteers consumed licorice in various doses: 50-200 g/day (referring to a candy preparation) for 2-4 weeks, corresponding to a daily intake of 75-540 mg of GA (5). Systolic blood pressure increased by 3-14 mm Hg, with a linear dose response relationship. It is projected that doses as low as 50 mg GA consumed daily for 2 weeks could cause a small but measurable rise in blood pressure. The effect of licorice consumption reached a maximum after 2 weeks.
The question arises as to the lowest dosage of licorice to produce no effect on hypertension. A study was performed to test this. Doses of 0, 1, 2 and 4 mg GA per kilogram body weight were administered orally to 39 healthy female volunteers for 8 weeks (6). A no-effect level of 2 mg/kg was suggested from the results of this study. The no-effect level corresponds to 120 mg in a 60 kg woman. However, the study authors recommended a lower acceptable daily intake of just 0.2 mg/kg body weight, using a safety factor of 10, yielding a figure of 12 mg GA/day for a person with a body weight of 60 kg. In the above study, doses of 75-540 mg were given, with a small effect noted at 75 mg.
In a review of published reports on licorice (7), it was observed that: "for the most sensitive individuals a regular daily intake of no more than about 100 mg glycyrrhizic acid seems to be enough to produce adverse effects. Most individuals who consume 400 mg glycyrrhizic acid daily experience adverse effects. Considering that a regular intake of 100 mg glycyrrhizic acid/day is the lowest-observed-adverse-effect level and using a safety factor of 10, a daily intake of 10 mg glycyrrhizic acid would represent a safe dose for most healthy adults."
So, there is a consensus that about 10-12 mg/day of glycyrrhizic acid should be safe for everyone (even those who might be sensitive to licorice effects) and that for most others, a safe level would be about 40-50 mg/day to avoid any blood pressure effects, with 100 mg (75-120 mg/day) having minimal effects that may barely be measurable. Licorice roots can have variable levels of GA, with typical figures in the range of 4% for Glycyrrhiza glabra (the Western licorice). If one uses a figure of 50 mg GA as a maximum allowable amount based on the above estimates, regular ingestion of licorice would be limited to about 2 grams per day. Higher dose licorice preparations might be used for a maximum period of 10 days.
A deglycyrrhized licorice (DGL) is available for situations where regular use of licorice (acting as an anti-inflammatory) at significant dosage is intended. DGL is commonly prescribed for gastro-intestinal ulceration. A new drug developed by Myogen for treating hypertension, Darusentan, blocks the action of licorice on raising blood pressure.
To minimize the chance of hypertension responses to licorice, patients should be interviewed about knowledge they might have about their blood pressure sensitivity to salt; presence of such sensitivity suggests that there will also be a potential reaction to licorice at moderate to high doses. Further, post-menopausal women, who have a tendency towards of blood pressure, should be cautioned about using high doses of licorice for a prolonged period.
In contrast to the story of licorice, ginger is mentioned in passing as provoking hypertension, but original sources are not readily found; apparently, no attempt has been made to study this suggested adverse effect. Similarly, a search of the literature regarding Pau D'arco, also known as Taheebo (Tabebuia impetiginosa) and for chasteberry (Vitex agnus-castus) does not reveal sources for information on hypertensive effects. Few of the other traditional herbs mentioned in the table have been shown to have a significant impact on blood pressure, and some, like parsley, seem to be listed incorrectly, as parsley is attributed a hypotensive action by most sources. Still, it advisable to be aware of those items suspected of causing a hypertensive reaction.
While one cannot assure patients that herbs not listed here won't affect blood pressure, one can assure patients that few commonly used herbs are known to have such an effect. To the contrary, numerous herbs have a hypotensive action. In Pharmacology and Applications of Chinese Materia Medica (8), 97 herbs (of which 68 are commonly used) are listed as having hypotensive effects (see Appendix 2 for a list of primary ingredients of hypotensive Chinese herb formulas).
September 2003