NEIGUAN (PERICARDIUM-6)
The acupuncture point neiguan (Pericardium-6) is probably best known in the West as a treatment for nausea and vomiting. It has been claimed in Western literature that not only standard acupuncture needling is effective for this application, but that one can use finger pressure massage (acupressure) at that site or even have the person wear a wristband that includes a bump that will press into neiguan when positioned properly. Unfortunately, the limited research on finger pressure for nausea and vomiting was notably flawed (see: Status of acupuncture research).
A clinical evaluation of stimulating neiguan to treat cisplatin-induced nausea also revealed no effect from using a 0.5 cm steel ball compressed against the point and held in place by a band (24). However, the researchers claimed that there was a high degree of success when applying, instead, a magnetic disk at neiguan, but not a non-magnetic disk. This result, implying that a magnetic field could markedly affect the point, appears suspicious with the lack of any detailed reporting in the publication, even at the level usual for Chinese medical publications. Further, in the several years since the study, follow-up research with magnet application has yet to appear in the literature.
Needling neiguan was used to alleviate nausea, vomiting, and chest pain caused by transcatheter arterial chemoembolization (a catheter is introduced into an artery that feeds the liver to locally introduce chemotherapy drugs in the treatment of liver cancer). In a study (26), involving 187 patients, treatment would be given once the side effects were noted during the invasive medical procedure. Needles were inserted to a depth of 0.8–1.0 cun, and after the needling sensation was attained, the needles were manipulated by lifting and thrusting 10–15 times (bird-pecking maneuver), this being repeated every 2 minutes. The needles were retained until the end of the procedure, which usually took about 50 minutes. The authors reported that Western medical treatments (the drugs zofran or granisetron given intravenously) could control the nausea and vomiting, but did not affect the chest pain. However, needling neiguan could alleviate the chest pain very rapidly. Nausea and vomiting could also be alleviated by the acupuncture treatment, but usually only after longer stimulus: in the most successful cases, after about 1 minute, but in many cases after 1–7 minutes of the intensive needling. The treatment of nausea and vomiting by this method is acceptable in China, where the drug therapies are quite expensive and needling can be done in the hospital at the same time as the catherization, but is less practical in the West, where intensive needle stimulation for several minutes may be impractical. Still, the rapid alleviation of chest pain—which was not attained with drug therapy—but was achieved by needling neiguan bilaterally, may yield a practical application even outside of China.
It turns out that, in China, the use of neiguan needling for nausea and vomiting is not the major application either historically (see following section) or in modern practice, though neiguan is sometimes included as a secondary point in such cases. For example, acupressure treatment of nausea (as commonly suggested by Western practitioners) was clinically evaluated by applying the pressure to hegu (Large Intestine-4) rather than neiguan (9); this study involved patients who become nauseated or even vomit during oral or laryngopharyngeal examination or treatment. The choice of the acupoint to treat was explained this way: “As the hegu point is used in treating facial and pharyngeal diseases and vomiting in pregnancy, the point was studied for possible prevention of nausea.”
For the treatment of morning sickness (1), characterized by nausea and, in severe cases, vomiting, a clinical trial involved acupuncturing women according to differential diagnosis (stomach-deficiency, liver heat, or phlegm-damp), using two acupuncture points (bilaterally, a total of four needles) as the main ones. In each case, zusanli was selected as one of the points (see: Zusanli), with either taichong (Liver-3) or fenglong (Stomach-40) as the second point. It was reported that “Most patients were relieved of vomiting after needling the main points. If curative effects were insignificant, however, auxiliary points were resorted to.” Auxiliary points in this study were an additional point or pair of points (treated bilaterally), for which neiguan was included for the phlegm-damp category (only point added) and neiguan was added along with zhongwan (Conception Vessel-12) for the stomach-deficiency category. The basis for adding neiguan was that it “has the action of regulating the triple burner, reducing rebellious qi, and stopping vomiting.”
When neiguan is the main point in a treatment, it has a different use, at least in China. According to reports, stimulating neiguan with appropriate techniques is an effective treatment for cardiovascular diseases, particularly cases where there is irregular heart rhythm or constricted blood flow (e.g., angina or heart attack). The most frequent application of neiguan stimulation, however, is as an adjunctive point to a number of acupuncture formulas, for which it has many uses aside from treating either cardiac disorders or nausea/vomiting.
HISTORICAL BACKGROUND
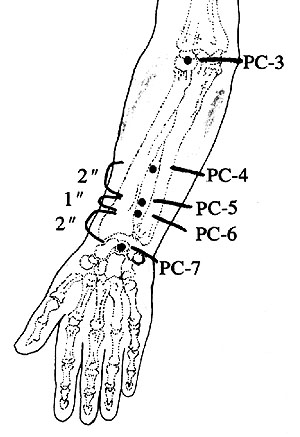
Neiguan is one of the 365 classical acupuncture points, located on the forearm portion of the short pericardium meridian that has a total of only nine standard points (see Figures 1 and 2). The term nei (inner) probably refers to the fact that it is on the inner side of the forearm; it appears to secondarily refer to the fact that the meridian travels between two tendons in the forearm, as is mentioned in the Lingshu (2) and the Compendium of Acupuncture (also known as the Systematic Classic of Acupuncture and Moxibustion (3)). Guan (pass) refers to the fact that the point is a luo vessel connecting point; that is, it is where there is a connection via the luo vessels (originally identified as the veins, easily seen in the area of neiguan) to waiguan (outer pass) on the triple burner meridian. In this case, wai (outer) refers to the fact that the meridian is running on the outer part of the forearm; guan has the same implication, with connection from the triple burner meridian to the pericardium meridian. According to the analysis presented in Grasping the Wind (4) both points have just the one name.
The pericardium (as an organ), pericardium meridian, and pericardium points barely get mentioned in the Neijing (5) and there is only a short passage in the Ling Shu that describes the pathway of the meridian and its influences:
When this channel is shaken [disturbed], it results in the palm of the hand being hot, the forearm and elbow being warped and stiff, and swelling in the armpit. In extreme cases, it results in fullness in the chest and ribs, palpitations of the heart, the face becoming red, yellow eyes, and incessant laughter. This channel controls the blood channels and pulses and may give rise to diseases such as anxiety in the heart, pains in the heart, and heat in the middle of the palm.
There is little mention of neiguan in the Compendium of Acupuncture (1691 A.D.). In The Golden Needle (6) these comments are presented:
· Jianli [CV-11] and neiguan sweep out suffocation within the chest.
· A full sensation in the chest due to abdominal pain—needle neiguan.
· A stomachache—then go for gongsun (SP-4), neiguan is the proper response and it must surely heal.
· Clamber through neiguan to zhaohai (KI-6) to cure a severe tummy-pain [this probably means treating both points; zhaohai is reportedly used for retention of urine, which would cause abdominal pain].
· Illness within the breast, neiguan will support.
It can be seen that the dominant historical uses are for fullness or illness in the chest and abdominal pain. The historic basis of needling neiguan for cardiac disorders (such as heart attack) resulting in chest fullness and epigastric pain is explained by Tang Zhaoliang (10), who has outlined the traditional descriptions of cardiac diseases:
In traditional Chinese medical literature, many physicians of various Dynasties recorded symptoms such as xin bi (heart pain) and zhen xin tong (genuine heart pain), both of which are very similar to those of coronary heart disease. In Su Wen, the chapter on the vitality of the vital organs has this account: ‘Cardiac patients usually complained of chest pain, substernal fullness, epigastric pains, back and interscapular aching, and pain in both arms. Ling Shu, the chapter on collapse describes: ‘Patients suffering genuine cardiac pain show cyanosis in the extremities, severe chest pains, and usually die in the evening if the attack starts in the morning, or die the next morning if the attack starts in the evening.’ Compendium of Acupuncture describes that acupuncturing neiguan causes the regaining of consciousness and the relief of cardiac pain. If the cardiac pain is acute, the reducing maneuver is indicated; if it is chronic, the reinforcing maneuver is indicated.’
MODERN APPLICATIONS
The references to
neiguan in the historical literature are not many, suggesting that the
widespread use of it that occurs today is due to relatively recent
interpretations of how the point can function in larger point formulas. The modern applications of neiguan,
as the main point in a treatment, are
described in Chinese Acupuncture and
Moxibustion (7):
Cardiac pain, palpitation, stuffy chest, pain in the hypochondriac region, stomachache, nausea, vomiting, hiccup, mental disorders, epilepsy, malaria, contracture and pain of the elbow and arm.
In another book by the same name (8), the following list is presented for neiguan indications:
Cardiac pain, palpitations,
stuffiness in the chest, gastric pain, vomiting, epilepsy, febrile diseases,
motor impairment of the upper limbs, hemiplegia, insomnia, vertigo, unilateral
headache (migraine).
The principal use of neiguan in modern China,
when used as a single point or primary point in a small group of points
in modern China, is cardiac
disorders, with pain in the stomach area as a second application, and other
uses being relatively minor, as will be seen.
For purposes of clinical and experimental research, zusanli, a widely used and extensively researched acupoint that is
not deemed specific for cardiovascular disorders, is sometimes utilized as a
control. Hegu (Large Intestine-4) is also sometimes utilized as a control
treatment, but because of its proximity to neiguan, and the possibility of
overlapping actions, it may not be as suitable for that purpose.
CLINICAL RESEARCH
Cardiac
research is conducted by monitoring the various measurable qualities of the
heart, which generally have to do with the details of its pattern of
beats. Patients are also monitored for
subjective sensations such as pain, chest fullness (pressure sensation),
palpitations (brief periods of sensing the heart beat as a result of
irregularities), and breathing disorders (which can occur secondarily). A common objective test is the
electrocardiogram (ECG; sometimes written EKG), an evaluation made by attaching
electrodes to the chest near the heart that can detect electrical fluctuations
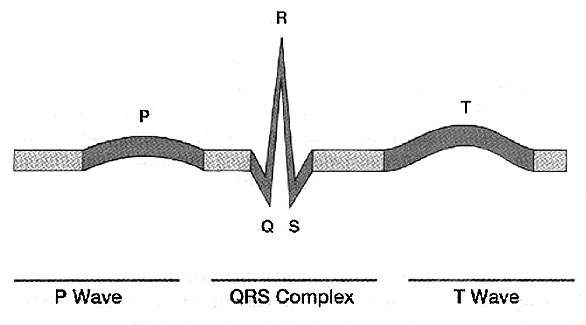
of the heart, which produce a characteristic wave form (see
Figure 3). The wave structure is
divided into segments labeled P, Q, R, S, and T. One of the most variable portions that is of interest in clinical
evaluation is the ST segment, which reflects the transition from activation of
the ventricles (lower chambers of the heart) to relaxation (recovery), with
reversal of electrical field. The heart
beat is regulated by surges of metal ions, such as sodium and potassium and
calcium, which give rise to changing electrical potential. In the normal heart, when monitored at rest,
the pattern detected by the ECG is quite regular and the heart rate is
appropriate to the individual (body size, age, sex, and level of weekly
exercise). Irregularities or abnormal
wave forms indicate a defect in the cardiac regulatory mechanism, cardiac
muscle, and/or condition of the cardiac arteries. Another monitoring device is the rheoencephelogram (REG), which
is used for monitoring the flow of blood through the vessels. When electrodes are appropriately placed,
the wave form reveals the underlying dynamics of blood flow: amplitude
reflects blood volume in pulsating vessels, influx time indicates the function
of the cerebral blood vessels, and main peak is an index of the elasticity of
the vessels. The echocardiogram is the reading obtained by ultrasound imaging of the
heart; it can be used to detect abnormalities in the condition and motion of
the heart walls and in the blood flowing through the heart.
In a study by Zhang Ren (11),
neiguan was needled for 137 patients with history of cardiovascular
disease. Most of the patients had
fullness in the chest, precordial pain, and dyspnea, and an abnormal ECG. Each day, neiguan would be needled on one side, alternating sides
from one day to the next. The needle
was inserted perpendicularly, and allowed to penetrate until the qi sensation
was felt. The tip of the needle was
directed toward the shoulder and manipulation of the needle was
performed until there was propagated qi to the chest. Then, the needles were stimulated for two minutes at moderate
intensity. The manipulation, with both
lift/thrust and twisting (100 times/minute), was repeated again after 10 and 15
minutes of treatment; at 20 minutes, the needle was removed. Needling was done daily for 10 days,
followed by a break of 3–5 days, and then again for 10 consecutive days. It was found that there were some immediate
beneficial effects of acupuncture on the symptoms and an increase in those
benefits gradually occurring with the full course of needling
on the characteristic symptoms. . In 41% of the patients, the symptoms of
palpitations, fullness in the chest, precordial pain, and dyspnea were totally
eliminated and in 54% of patients they were improved after the course of
therapy. ECG remained essentially
unchanged in 53% of the patients, showing that the underlying disorder in
cardiac rhythm could persist while other aspects of the disorder were
alleviated. It was also found that
there were declines in cholesterol, triglycerides, and beta-lipoproteins.
A study reported by Wang Wenzheng and Liu Weizhou involved 68
patients with hypertension and early cerebroarteriosclerosis (12). Neiguan was needled perpendicularly to a
depth of 0.5–1 cun on the left side.
Manipulation was by twirling to give moderate stimulation until the qi
sensation was obtained, and thenwas
continued for about one minute. The
needle was then retained for three minutes and removed. Control patients had needling done at hegu (LI-4), at 2–2.5 cm deep, using the
same method and timing of manipulation and retention, also on the left
side. A rheoencephalagram was used to
monitor the effects, with electrodes on the same side as the needling. Beneficial changes in the recorded wave form
of the pulse were found with needling at both neiguan and hegu, but only the needling at neiguan produced a significant
improvement in influx time (still, the authors could not assure that
differences between needling the two points reflected their functions or some
slight differences in patients being treated).
Needling of both points slowed the heart rate, dilated the cerebral
arteries, and improved blood supply to the brain.
Patients with rheumatic heart disease were treated with acupuncture at neiguan at the Shanghai Second Medical College (13). The 21 patients had chronic disease lasting at least 9 years (average 17.5 years), and most suffered from mitrial valve disorder and auricular fibrillation. The patients had previously been receiving acupuncture therapy to control their symptoms, but stopped two weeks before the investigation began. Neiguan was needled bilaterally, with perpendicular insertion and a depth of 0.5–1.0 cm depth until the patient felt a needling sensation. Then the needles were twirled in 150–180 degree rotation at a frequency of 80–100 times per minute for two minutes. Needles were retained for 15 minutes and then removed. The author reported that the needling sensation was very strong. After the 5th acupuncture session, the rotation on twirling was reduced to 80–120 degrees. All patients experienced needling sensation and most experienced propagation of the needling sensation along the channel (some patients had the propagated sensation to the shoulder or chest, but most had a shorter distance of propagation). All patients reported a feeling of lightness during acupuncture. Acupuncture was performed every other day (three times per week) for four weeks.
Some responses were noted during the acupuncture treatment: 10 patients with precordial distress had alleviation during the sessions. Other improvements required several days; the reported changes after the month of treatment included relief of: palpitations, fatigue, edema, insomnia, and liver enlargement. The patients had an initial low level of plasma cortisol, which increased after treatment. Improvements were noted in heart function monitored by ECG and echocardiogram. Most of the patients were on medications to control their condition prior to the study, and some patients were able to reduce their dosage or discontinue medications without return of symptoms. Of the 21 patients treated, 20 showed notable improvements in symptoms and in the function tests. Two months after the course of acupuncture therapy, 15 of 21 patients retained the improvements; for the other 6, recurrence of symptoms appeared 2–4 weeks after cessation of acupuncture.
Patients with idiopathic cardiomyopathy (18) were treated with
acupuncture at neiguan and, later, for additional testing, at shaofu (Heart-8). Needling was performed bilaterally at
neiguan to evoke needle sensation (qi reaction) of soreness, numbness,
distention or heaviness, and electroacupuncture equipment was then attached to
provide a current with frequency of 120 pulses per minute for two minutes. Then the needles were retained without
further stimulus for 15 minutes. Twenty
minutes later, shoufu was treated
bilaterally with the same stimulus method.
Changes in heart function were monitored with an echocardiogram. According to the authors, younger
individuals had quicker responses, with changes observed 2 minutes after the
electroacupuncture treatment, increasing to a maximum in 7–10 minutes. Older individuals had a slower response that
was maximal about 10-–20 minutes after stimulus.
There were different responses to neiguan and shaofu. As to the effect of neiguan, the authors report:
In patients with congestive cardiomyopathy, acupuncture of neiguan caused an increase of systolic diameter in some, and in increase in diastolic diameter in most cases, with an increase in cardiac contraction....There was shortening of isometric contraction time and systolic time interval. The above results suggest that puncturing neiguan could increase cardiac contraction in congestive cardiomyopathy....Acupuncture of neiguan could reduce the left ventricular and diastolic pressure by increasing myocardial contraction.
One patient with hypertrophic cardiomyopathy had an increase in the left ventricular and diastolic pressure, so that the authors suggested to avoid this treatment in such cases (at least, until more is known).
In a study of patients who had experienced heart attack, with
myocardial ischemia confirmed by ECG, neiguan was treated by using needle
rotation stimulus intermittently during a period of 30 minutes (22). In 20 of 21 patients so treated, there was a
significant changes in the ST segment of the ECG. Plasma endothelin (a peptide that causes
vasoconstriction), which was elevated before treatment, was shown to decline
notably after treatment. Needling at zusanli (Stomach-36) used as a control
produced no significant effects.
The time of day when neiguan is needled may have an influence on
the effectiveness of the treatment of heart disease. Researchers as the Huaibei Hospital in Anhui compared acupuncture
treatment of coronary heart disease patients at 8:00 A.M. versus 8:00 P.M. (23). The researchers had previously studied the
influence of time of electroacupuncture at neiguan on the effects on systolic
time interval (STI; time of heart contraction) in coronary heart disease patients. They had noted that the most remarkable
difference was between administering the stimulus at chen time (daybreak: 7:00–9:00 A.M.) versus at xu time (dusk: 7:00–9:00 P.M.).
Therefore, they undertook additional investigations at these two
times. Patients were treated at neiguan
bilaterally, and after getting the qi reaction, the
needles were connected to electrical stimulation apparatus and stimulated at 4
Hz for 2 minutes, using the greatest stimulus that the
patients would permit, and then t. The needles were then removed
and the effects of treatment were recorded (via electrocardiophonogram, similar
to ECG, and carotid pulsilogram, similar to rheocardiogram).. The treatment was administered every day for
6 days at one of the times, then there would be a 2 day break, followed by
another series of 6 days at the other time, in randomly assigned order; thus,
each patient was his/her own control.
It was revealed that left ventricular function was improved when needling was done in the morning, but not in the evening. The authors speculated that this was due to the natural changes that occur in the dominance of the sympathetic versus parasympathetic nervous systems at the different times of day and their influence on heart function. They concluded that:
At chen time, the excitability of the parasympathetic nervous system reduces gradually while that of the sympathetic one rises and the heart has had enough rest at night so acupuncture performed at that time increases the sympathetic nervous function of the heart and gives a beneficial stimulation for the recovery of the function of ischemic myocardium. Therefore, the left ventricular function of coronary heart disease patients can be improved.
By contrast, at xu time, increasing the excitability of the sympathetic nervous system and decreasing the excitability of the parasympathetic nervous system when the heart is tired could disturb its normal rhythm because acupuncture at this time works against the natural cycle. According to this interpretation, coronary heart disease patients should be treated early in the morning and should not take late afternoon appointments, at least when attempting recovery of heart regularity via needling at neiguan.
The potential of nearby acupuncture points to have effects similar to that of neiguan is illustrated by a study conducted at the Shaanxi College of Traditional Chinese Medicine (25). A total of 86 patients, most of whom had suffered from coronary heart disease, rheumatic heart disease, and hypertensive heart disease, were treated at acupoint ximen (Pericardium-4), located slightly higher on the inner forearm than neiguan. Needling was carried out bilaterally with medium intensity stimulation using lifting, thrusting, and rotating of the needle; this stimulus was provided every 5 minutes over a total treatment time of 30 minutes. ECG was monitored before and after treatment to observe the immediate effects. According to the report, substantial improvements in ECG (with it appearing normal) were noted in 14% of the patients, and moderate improvements in ECG were noted in another 67% of the patients. The best results were said to have been obtained from patients with acute myocardial infarction and those with chronic coronary insufficiency.
EXPERIMENTAL RESEARCH
A summary of research on acupuncture for cardiovascular diseases was presented by Tang Zhaoliang (14). In it, he mentioned:
Animal experiments
demonstrated that electroacupuncture of neiguan accelerated the recovery of
deviation of the ST segment of the ischemic heart of a rabbit. In the experimental dog in which the
coronary artery had been ligated, acupuncturing neiguan decreased the total
amount of ST segment elevation and the number of leads of elevated ST segments
in epicardial ECGs. In addition, it
also reduced the coronary resistance, and improved the oxygen supply to the
ischemic heart.
Chen Lianbi reported (17) that myocardial oxygen pressure is
increased by needling neiguan. He
treated dogs that had induced cardiac ischemia and monitored the heart
oxygenation with oxygen electrodes.
Treatment was carried out with electroacupuncture, using a 2.2 Hz spike
wave. Treatment ast zusanli was used as a control,
and did not produce the improvements in cardiac tissue oxygen levels.
Other experimental studies
have been undertaken to elucidate the mechanism by which needling neiguan
ultimately affects the heart. In an
experimental study (15), the authors studied the relation of neiguan needling
to activity of the vagus nerve (part of the parasympathetic system that
regulates the heart).
They concluded from their experimental observations that
electroacupuncture of neiguan acupoints primarily produces inhibition of
cardial vagal activity. They noted that
it also produces some excitation of cardio-sympathetic activity, but suggested
that this was only a stress reaction to acupuncturing. In their review of the literature, the
authors pointed out that “Clinical practice and animal experiments showed
acupuncture at neiguan acupoints was useful in improving or modulating
ventricular performance....Li reported that electric acupuncture of
neiguan acupoints could stabilize the fluctuations of left ventricular pressure
induced by asphyxia. The homeostatic
action apparently mobilizes a circuit or part of a circuit in the central
nervous system.”
Investigating the role of the brain in mediating the acupuncture therapy, Lai Zhongfang and his colleagues (16) tested electroacupuncture at neiguan in rabbits. The points were stimulated for 5 minutes by electrical pulse stimulation. As a control, some rabbits were treated at zusanli (Stomach-36) instead. They found that the frequency of spontaneous discharges at the amygdaloid nucleus neurons, a part of the limbic system, were elevated by myocardial ischemia and could be normalized by treatment at neiguan; the effect of needling zusanli was far less. The authors mentioned that previous studies indicated that the amygdaloid nucleus is also a site of action of acupuncture anesthesia.
This work was followed up by Lai and his colleagues (19) with
more extensive studies, also in rabbits.
He confirmed that in rabbits with acute myocardial ischemia
(AMI; heart attack), neiguan treated by acupuncturetreatment by
acupuncturing neiguan bilaterally and using electrostimulation for 5
minutes would affect the amygdaloid nucleus.
As before, the cardiac ischemia induced changes in the amygdaloid
nucleus and these changes could then be normalized by electro-acupuncture,
suggesting that this part of the brain is the mediating region between
acupuncture at neiguan and therapeutic benefits to patients who suffer from
heart attacks.
TO IMPROVE THE OUTCOME OF OTHER ACUPUNCTURE TREATMENTS
The most frequent use of neiguan, aside from cardiovascular diseases, is to enhance the outcomes from other acupuncture treatments. Unfortunately, this application has little basis in historical records and is virtually untestable by modern clinical research (detecting the difference between an effective therapy and a more effective therapy requires very large numbers of patients matched, randomized, and treated by a consistent method). Therefore, the following discussion is intended primarily to reflect the thinking of experienced acupuncturists that leads to this particular application.
Perhaps the best summarization of the use of neiguan as an aid to acupuncture therapy is given by Yu Huichan and Han Furu in their book on physician Wang Leting (20). There are three underlying concepts presented:
1. “Because the heart rules the spirit brightness and the blood vessels, therefore neiguan frees the flow of the vessels and quickens the blood.”
2. “Since the pericardium [meridian] branches to traverse the triple burner [meridian], neiguan can free the flow of the three burners. Therefore it has the function of freeing and regulating the three burner qi transformation and thus the movement of qi and disinhibition of water.”
3. Based on the traditional concepts that “Yin and yang are rooted in each other” and that “solitary yang cannot engender; solitary yin cannot grow,” Wang Leting selected neiguan “in order to make yin combine with yang.”
The underlying belief, then, is that needling neiguan restores movement of qi and blood and interchange of yin and yang, thereby aiding the basic processes by which the body heals. If an acupuncture treatment is failing to gain the desired results, or if it requires the assistance of restoring normal flow of qi and blood, then needling neiguan may stimulate the extra movement in the vessels that is essential to make the change in the person being treated. This sentiment was also expressed by physician Andrew Tseng, who came to America to practice acupuncture after long experience in Shanghai. His concepts and methods are relayed by Robert Johns, in the book The Art of Acupuncture Techniques (21). He claims, without detailed reference, that there is an historical basis for the use of neiguan as an adjunct point, suggesting that Yang Jizhou, at the end of the 16th century (when the Compendium of Acupuncture was published) investigated the traditional literature and found that “in addition to enhancing the effect of treatments, neiguan has a synergistic influence on acupuncture points.” Johns concludes that “When applying a prescription for treatment, it is possible to bolster the outcome of that treatment by adding neiguan.” Although other literature references to this are not easily found, it does seem to reflect the current thinking about use of the point.
According to Dr. Tseng’s clinical notes, neiguan is useful in numerous small prescriptions involving 1–5 acupuncture points (bilaterally, so 2–10 needles; the one point treatments are neiguan alone). A list of 58 such formulas are presented in Johns’ book and the applications can be summarized as follows (examples given below include combining with other points, mentioning one of the other points in a formula):
·
Cardiovascular disorders: tachycardia, irregular heartbeat, missing
heartbeat, angina, heart pain, chronic heart disease, rheumatic heart disease,
hypertension, hypotension, neurasthenia (as defined in this case as weak heart,
with weak pulse). Typical combining:
use with shenmen (Heart-7) in cases
of irregular heartbeat and rheumatic heart disease; use with taichong (Liver-3) in cases of
hypertension and hypotension.
· Brain and mental disorders: cerebral concussion, schizophrenia, hysteria, mental disorder (manic/depressive), epilepsy, hysteria, vertigo, insomnia. Typical combining: use with yamen (Conception Vessel-15) in cases of schizophrenia, manic/depressive, and epilepsy.
· Lung disorders: wheezing, cough, asthma, whooping cough, pneumonia, pleurisy, loss of voice. No other single point appears repeatedly in these therapies.
· Stomach disorders (other than pain): vomiting, nausea, hiccup. No other single point appears repeatedly in these therapies.
· Pain of the chest and abdomen: gallbladder stones, pain of indefinite origin (chest region), pain in hypochondriac region, postoperative pain, pain or distention of chest or epigastric area, stomach pain, upper abdominal pain, abdominal pain, pain before eating, pain after eating (not due to overeating), stomach spasm. Typical combining: use with zusanli (Stomach-36) for pain in the stomach and pain after eating; combine with sanyinjiao (Spleen-6) for abdominal pain and pain before eating.
· Female disorders: leukorrhea, menstrual cramps, infertility, anemia. Typical combining: use with sanyinjiao (Spleen-6) for menstrual cramps and anemia.
· Emergency cases: heatstroke, revival from drowning, coma or shock, electrical shock. Typical combining: use with zhongchong (Pericardium-9) for heatstroke and electrical shock.
REFERENCES
1. Zhao Rongjun, 39 cases of morning sickness treated with acupuncture, Journal of Traditional Chinese Medicine 1987; 7(1): 25–26.
2. Wu
Jing-Nuan (translator.), Ling
Shu, or The Spiritual Pivot, 1993 Taoist Center, Washington, D.C.
3. Mi Huangfu, Systematic Classic of Acupuncture and Moxibustion, 1994 Blue Poppy Press, Inc., Boulder, CO.
4. Ellis A, Wiseman N, and Boss K, Grasping the Wind, 1989 Paradigm Publications, Brookline, MA.
5. Ni M, The Yellow Emperor’s Classic of Medicine: A New Translation of the Neijing Suwen with Commentary, 1995 Shambhala, Boston, MA.
6. Bertschinger
R (translator.), The Golden Needle, 1991 Churchill
Livingstone, London.
7. Qiu
Maoliang (managing editorng. ed.), Chinese Acupuncture and Moxibustion,
1993 Churchill Livingstone, London.
8. Zhang
Enquin (editor. in chief), Chinese Acupuncture and Moxibustion, 1990 Publishing House of
Shanghai College of Traditional Chinese Medicine.
9. Deng
Dianhua, Tan Qinglan, and Han Jisheng,
Observation on combating nausea by finger pressure on the hegu point,
Journal of Traditional Chinese Medicine 1986; 6(2): 111–112..
10. Tang Zhaoliang, Assessment of acupuncture in the prevention of sudden death from coronary heart disease, Journal of Traditional Chinese Medicine 1987; 7(2): 142–146.
11. Zhang Ren, Effect of neiguan needling in cardiovascular disease: analysis of 137 cases, unpublished manuscript, Shanghai Association of Acupuncture and Moxibustion, 1983.
12. Wang Wenzheng and Liu Weizhou, Effect of acupuncture at neiguan and hegu on the rheoencephalogram in patients with hypertension and early cerebroarteriosclerosis, Journal of Traditional Chinese Medicine 1987; 7(4): 238–242.
13. Wu Yixian, et al., Therapeutic effect and mechanism of acupuncture at neiguan in chronic rheumatic heart disease, Journal of Traditional Chinese Medicine 1982; 2(1): 51–56.
14. Tang Zhaoliang,
assessment of acupuncture in the prevention of sudden death from coronary heart
disease, Journal of Traditional Chinese Medicine, 1987; 7(2):143-–146.
15. Kong Suming, Heart rate power spectral analysis during
homeostatic action of neiguan acupoint—role played by the cardial vagus nerve,
Journal of Traditional Chinese Medicine, 1988; 8(4): 271-–276
16. Lai Zhongfang, Effect of electro-acupuncture of neiguan on spontaneous discharges of single unit in amygdaloid nucleus in rabbits, Journal of Traditional Chinese Medicine 1989; 9(2): 144–150.
17.
Chen Lianbi, The effects of electrical acupuncture of
neiguan on the PO2 of the border zone between ischemic and non-ischemic
myocardium in dogs, Journal of Traditional Chinese Medicine 1983; 3(2):
83–88.
18.
Chen Shuxia, et al., Preliminary investigation of the effect of
acupuncture at neiguan and shaofu on cardiac function of idiopathic
cardiomyopathy, Journal of Traditional Chinese Medicine 1983; 3(2):
113–120.
19. Lai Zhongfang, Role of amygdaloid nucleus in the correlation between the heart and acupoint neiguan in rabbits, Journal of Traditional Chinese Medicine 1991; 11 (2): 128–138.
20. Yu Huichan and Han
Furu, Golden Needle Wang Leting,
1997 Blue Poppy Press, Boulder, ColoradoO.
21. Johns R, The Art of Acupuncture Techniques, 1996
North Atlantic Books, Berkeley, CaliforniaA.
22. Lin Hongwu, et al., Specific therapeutic effect of neiguan on heart disease, International Journal of Clinical Acupuncture 1998; 9(8): 303–305.
23. Li Lei, et al., Comparative observation on effect of electric acupuncture of neiguan at chen time versus xu time on left ventricular function in patients with coronary heart disease, Journal of Traditional Chinese Medicine 1994; 14(4): 262–265.
24. Liu Shaoxiang, et al., Magnetic disk applied on neiguan point for prevention and treatment of cisplatin-induced nausea and vomiting, Journal of Traditional Chinese Medicine, 1993; 11(3): 181–183.
25. Yin Kejing and Jia Chengwen, Treatment of chronic coronary insufficiency with acupuncture on ximen point, Journal of Traditional Chinese Medicine 1991; 11(2): 99–100.
26. Mu Rong, et al., Observation on therapeutic effect of acupuncturing neiguan on the complication of hepatic carcinoma intervention therapy, Chinese Journal of Integrated Traditional and Western Medicine 1996; 2(2): 130–131.
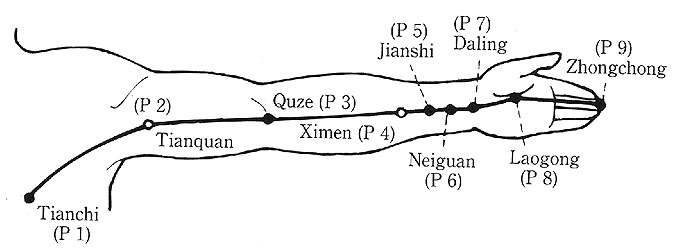
Figure 1.
December 1998