 Sweet clover |  Karl P. Link |
WARFARIN AND CHINESE MEDICINE
The history of Warfarin can be traced to the story of dairy farming in the midwestern U.S. Dairy herds were introduced to the Midwest soon after the Civil War, around 1870, with a large concentration in Wisconsin, which eventually became known as "the Dairy State." This farm industry grew rapidly once commercial milk pasteurizing machines were developed in 1895. Researchers at the University of Wisconsin, Madison (founded 1848, the same year that Wisconsin became a state) also contributed greatly to the development of the dairy industry. For example, in 1890, an agricultural chemistry researcher, Dr. S.M. Babcock, developed a rapid testing method for determining the butter fat content of milk, allowing the milk to be sold according to the fat content to an industry where butter manufacture was becoming a major undertaking.
More importantly, another professor at the University, Harry Steenbock, demonstrated in late 1923 that irradiation with ultraviolet light increased the vitamin D content of milk and certain other foods (it converts cholesterol derivatives into the vitamin). Although others had come upon this finding around the same time, Steenbock knew his observation held the potential to eliminate rickets, a crippling bone disease of children caused by vitamin D deficiency, if he could only make it practical. So, he worked on design of procedures and equipment to generate the vitamin and he convinced the University to form an organization to manage patents of this and other discoveries. His efforts led to the establishment of the Wisconsin Alumni Research Foundation (WARF) in 1925. Its first formal action was to license the use of Steenbock's irradiation process to fortify the vitamin D content of breakfast cereals (1927). Soon after, the invention was licensed to several pharmaceutical companies for the production of vitamin D that could be used as a supplement. In order to deal with rickets (a childhood disorder in which malformation of the weakened bones occurred as the child grew) he wanted to get the vitamin into milk. The disease usually began soon after weaning from breast milk.
At that time, it was not legally possible to add anything to milk, so Steenbock's process was elaborated to allow irradiation of milk as it flowed through processing equipment-to generate vitamin D without adding anything-which was accomplished by 1932. The increased vitamin D in milk, cereals, and bread virtually ended the tragedy of rickets by the time the patent ran out in 1945. Income from this extremely beneficial work transformed WARF into a huge research supporter (currently providing $30 million/year).
The dairy industry in the area had grown considerably during this time. Efforts were undertaken to find the best way to feed the increasing herds. Hay and corn were the main silage, but as the dairy farms spread out into less favorable terrain, these crops were not always easily provided in sufficient quantity. Sweet clover (Melilotus sp.), introduced from Europe, was found to be a good food source, having a nutrient composition about the same as alfalfa. It grew well on poor soil and could be grown with or blended into hay, and so it became a common part of dairy feed in much of the Midwest since about 1900. The problem with sweet clover, however, was that it was much moister than the hay, and could easily rot. Animals eating the rotted feed might suffer from adverse effects. Hemorrhage in animals feeding on spoiled clover had been noted as early as the 1920s, and the contaminated feed could also cause abortions. Two researchers at the University of Wisconsin, R.A. Brink and W.K. Smith, had been trying to breed a strain of clover free of the anticoagulant factor for several years, and efforts to isolate the compound were underway in Karl P. Link's laboratory by the time a Wisconsin farmer, Ed Carlson, visited in 1933, but Carlson's visit stimulated intensive follow-up. An article describing the anticoagulant was published by Link (photo, below) in 1940 and the isolation of the compound, dicoumarol, was reported by Link and a coworker in 1941.
 Sweet clover |  Karl P. Link |
Plant enzymes in sweet clover are released when the plant is cut and they act on its glycoside component melilotoside, removing the sugar group and leaving coumarin. The moist, soft stems of the clover are easily contaminated with molds (including Penicillium and Aspergillus) which metabolize the coumarin into dicoumarol. Dicoumarol interferes with the vitamin-K activation of clotting (by tying up the enzyme vitamin K epoxide reductase).
Dicoumarol was patented as an anticoagulant in 1941. However, its action was difficult to control, the dosage range was very large (25-200 mg/day), and it was never extensively used, partly because another anticoagulant was of greater interest-heparin (isolated from cattle liver and lung, and purified sufficiently for human use in 1937). Heparin was relatively safe to use, but had to be given intravenously. It remains a valuable therapy to this day, with a modified low molecular weight version, enoxaparin, introduced recently.
Link continued his work with coumarin and dicoumarol. But, he turned to the problem of rodent control, which was another issue faced at dairy farms (and elsewhere). Since his work with dicoumarol was traced to the problem of hemorrhaging in cattle, he thought of using the compound as a rat poison, to cause hemorrhaging and death. It turned out to be too weak and unreliable for that purpose, so he and his coworkers synthesized some variants and successfully isolated a more potent compound. Patent rights were assigned to the foundation that funded the work, WARF, from which the name warfarin was derived (WARF + coumarin). In 1948, warfarin was launched as a new commercial product: the ideal rat poison. It is currently the most widely used rodenticide in the world.
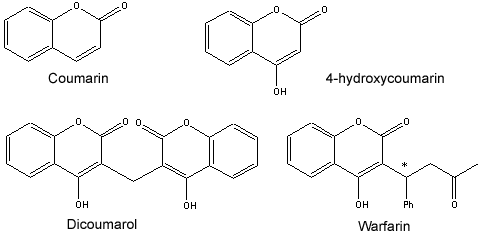
Turing a rat poison into a widely used drug for humans may seem odd, and its path to success was paved by an unusual series of events. In 1951, a navy recruit unsuccessfully attempted suicide by taking rat poison. He had consumed over 500 mg of warfarin (100 times the standard clinical dose of the drug as now used in humans), seemingly more than enough of a rat poison to cause death. Yet, he made a full recovery. This led to research into the potential of using warfarin instead of dicoumarol in humans, since it was a more potent anticoagulant, yet not acutely toxic. In fact, early testing showed that it was far superior to dicoumarol, and clinicians soon discarded dicoumarol in favor of warfarin. The rat poison turned drug was introduced commercially as a human anticoagulant in 1954. It was soon put to very good use: President Eisenhower was treated with warfarin following a heart attack during his early presidency, in 1955, and it is credited, along with other medical interventions, with saving him. He remained president until the end of his second term (January 1961) and lived until 1969 (reaching the age of 79).
Warfarin is currently the most frequently used prescription-only "blood thinner" (aspirin, available over the counter, is also an important anticoagulant, functioning by a different mechanism). Warfarin is also one of the most frequently prescribed drugs overall, ranking 11th in 1999 (the top ten positions are dominated by lipid-lowering, anti-ulcer, and antidepressant drugs). Warfarin is often sold under the brand name Coumadin (trademark of DuPont), but is also available as a generic. About 1.5 million people take the drug on any given day in the U.S.; many people use it for years. Most medical researchers believe warfarin is greatly underutilized. The dominant uses, at present, are for persons who have had a prior history of dangerous blood clots (e.g., heart attack, stroke, deep vein thrombosis); for those who have heart disorders that may easily lead to clotting (e.g., atrial fibrillation, heart valve deformities, etc.); and those who are undergoing surgery that may lead to formation of clots that can migrate to the heart or brain (e.g., hip or pelvic surgery).
Warfarin "thins" the blood by inhibiting clots from forming (it also helps to inhibit existing small clots from growing larger, but does not dissolve existing clots; see next section). Warfarin is an antagonist of vitamin K, a necessary element in the synthesis of four clotting factors (II, VII, IX and X; see below for list) and three of the naturally-occurring anticoagulant proteins (C, S and Z). These factors are biologically inactive without an enzymatic process (occurring primarily in the liver) that requires vitamin K as a cofactor.
| Factor | Name |
| I | Fibrinogen |
| II | Prothrombin |
| III | Tissue Factor or thromboplastin |
| IV | Ca2+ |
| V | Proaccelerin |
| VII | Proconvertin |
| VIII | Antihemophilic A factor |
| IX | Antihemophilic B factor |
| X | Stuart factor |
| XI | Plasma thromboplastin antecedent |
| XII | Hageman factor |
| XIII | Fibrin Stabilizing Factor |
Therapeutic doses of warfarin reduce the production of functional vitamin K-dependent clotting factors by 30-50%; there is a 10-40% decrease in the biologic activity of the clotting factors. As a result, the coagulation system responds slowly. Vitamin K ingestion at high levels will partly counter this effect, so patients are cautioned about taking supplements with vitamin K and about consuming any large amount of vitamin-K rich foods (e.g., cabbage, cauliflower, spinach and other green leafy vegetables, cereals, soybeans, and other vegetables).
The current recommended daily intake for vitamin K, which corresponds closely to amounts typically consumed, is 70-80 mcg, though up to twice this amount is readily attained and may prove helpful in preventing osteoporosis. Foods rich in vitamin K can provide far more than these amounts. For example, the vitamin K content in a 100 gram serving (3.5 ounces) of cooked spinach is about 540 mcg (similar amounts are obtained from kale, turnip greens, collards, and raw parsley); for green leaf lettuce, it is about 270 mcg (but the paler butterhead lettuce has only about 100 mcg); and broccoli has about 120 mcg.
Despite the concerns often expressed about consuming vitamin K during warfarin therapy, the FDA guidelines allow for considerable intake of the vitamin. In their "Important Food and Drug Information" series, the FDA recommends for warfarin users no more than one serving per day of high vitamin K foods (those that provide 2-6 times the usual recommended daily intake of vitamin K) and no more than 3 servings per day of foods moderately high in vitamin K (from 2/3-2 times the usual recommended daily intake). Hence, one could easily consume over 500 mcg of vitamin K each day under these guidelines, more than 6 times the typical level. With the higher regular vitamin K intake, a person may require a somewhat higher warfarin dosage to maintain the desired blood thinning effects of the drug. Earlier suggestions that people taking warfarin should avoid vitamin K-containing foods to the extent possible have been overturned. In fact, such an approach would likely lead to other health problems, as vitamin K has important roles in the body other than participating in blood clotting factors, particularly in regulating calcium distribution (enriching the bones, preventing calcification of the arteries). Further, the vegetable sources of vitamin K provide other important nutritional components and fiber. It has been suggested that one must maintain a relatively constant level of vitamin K rich foods to maintain the desired anticoagulant activity, but that is a difficult lifestyle goal with minimal impact on blood coagulation during warfarin therapy in most cases.
A blood test is used to monitor the effects of warfarin therapy; the main one relied upon for determining the appropriate drug dosage is the Prothrombin Time (PT, sometimes called protime for convenience). The results of the test for persons on anticoagulant therapy is expressed in terms of the International Normalized Ratio (INR; the data may be described as PT/INR, meaning prothrombin test expressed in INR). The INR indicates how much longer it takes the blood to clot when taking an anticoagulant compared to typical times required without an anticoagulant present (which is about 11-14 seconds). The common goal of warfarin therapy is to have an INR in the range of 2-3 (this goal may be shifted under certain circumstances). An INR of 2 indicates that the blood is taking twice as long as normal to clot in the test (i.e., about 22-28 seconds); an INR of three, three times as long (about 30-45 seconds). An INR above 1 (actually, above 1.2, to allow for natural variability) indicates that there is some degree of reduced coagulation; a value greater than 3 may be desired in some cases, but is associated with a significant risk of spontaneous bleeding. Once the INR reaches the desired range, the blood should be monitored weekly until it is stable (e.g., when the variation is not more than about 10%). Thereafter, the time between tests can be extended for those on long-term therapy.
In many cases, patients are started with 5 mg/day of Coumadin or its generic version (as a single tablet), and then the dosage can be modified according to the measurement of PT/INR. Warfarin begins having an effect within 24 hours, but the full response to the drug is attained over a period of about 3-4 days; and this is the time it takes to note INR changes when the dose is changed, so a weekly test is usually adequate. Warfarin effects on clotting vary markedly with the individual, and the response is often sensitive to age (less dosage of the drug is usually needed at higher ages). Typical long-term warfarin dosage ranges from 2-10 mg per day. For persons who have some history of bleeding, the starting dosage is usually low and the target INR may be kept in the range of 2.0-2.5. When the INR is outside the desired range, modifications of dosing are made gradually to bring it into that range. Half tablets are often used to make the adjustment, so Coumadin tablets have a slit in the center to aid breaking them cleanly in half.

Although a variety of rare side effects to the drug have been reported (e.g., cold intolerance, loss of appetite, stomach pain or cramping, which are usually alleviated after a few days; but also the more severe problem of skin necrosis), the main concern about adverse responses is related to the desired action of the drug: to prevent clotting. Its use can lead to undesired bleeding. In most instances, problems of bleeding can be easily detected (e.g., numerous observable bruises, stool blackened by congealed blood, blood in the urine, nose bleeds, etc.), and the dosage can be adjusted to reduce these effects. However, bleeding can occur internally with serious results, including fatality (such as with a brain hemorrhage).
Interactions of drugs with warfarin are frequently cited in the literature, with long lists of over 100 suspected drugs and entire categories of drugs. Several of the reported cases may involve interactions that are rare idiosyncratic responses unlikely to be observed repeatedly. Drugs can accelerate the removal of warfarin from the system or block its effects, thus reducing the INR when added to the regimen (and increasing the risk of experiencing a clot), while others may reduce the rate of elimination of the drug or enhance its effects, or provide anticoagulant effects by other mechanisms, thus increasing the INR (and increasing the risk of experiencing bleeding). Drugs that are used in anticoagulant therapy, such as aspirin, are an obvious concern (however, combining anticoagulant therapies may be intentional). In most cases, it is not necessary to avoid use of the drug that may interact with warfarin; rather continued monitoring of the PT/INR will help the physician to adjust its dosage to keep the anticoagulant activity in the correct range.
The situation where formation of a blood clot is considered a desired, natural, and healthy response is when an injury occurs. If a blood vessel is broken, it is important that a clot form to prevent excessive blood flow (out of the body or into areas of the body not intended to be infused with blood). The damaged vessel releases a number of messengers that interact with the blood clotting system, yielding a clot at the site of damage. This same clotting mechanism must be maintained in the "off" condition where there is no injury. A complex and tightly controlled system helps assure capability to form clots as needed while avoiding clots the rest of the time, and breaking down clots only after the injury is repaired.
Several diseases can adversely affect blood clotting, as can the influence of lifestyle. Inflammatory processes that affect the blood vessels may contribute to signaling the clotting system that there is an "injury;" high levels of blood lipids (especially when in oxidized form) and of blood sugars may make the clotting factors more active; lack of exercise may shift the balance of lipids and affect their influence on clotting. An increasing number of blood tests can monitor levels of substances that contribute to clotting events, including homocysteine, platelet activating factor, and plasminogen activator inhibitor (see below). Recommendations to help avoid excessive clotting include maintaining healthy weight through diet and exercise, avoiding smoking, and consuming foods and beverages rich in phenolic compounds (e.g., flavonoids), such as apples, tea, onions, and moderate amounts of red wine or grape juice.
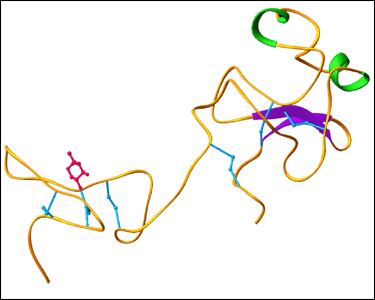
Once blood clots form, there are natural mechanisms to break them down. The primary mechanism is fibrinolysis: degrading fibrin polymers that stabilize a clot via strong bonds formed by activated factor XIII (fibrin-stabilizing factor; it is not inhibited by warfarin). These fibers produce a mesh that traps platelets, blood cells, and plasma to form a clot. The removal of the clot is caused, in part, by plasmin, which cleaves the fibrin monomers. Plasmin, in turn, is produced by the cleavage of its precursor, plasminogen, by enzymes called plasminogen activators (PAs; such as tissue PA and urokinase-type PA, pictured below). But, there is an inhibitor of this enzyme that is present at elevated levels in many people who have problems with excessive clot formation, such as diabetics. This inhibitor is called PAI (plasminogen activator inhibitor); there are two known types: PAI1 and PAI2. Drugs that block the inhibitor could help the body resolve clots more readily. Statin drugs, increasingly used to help prevent heart attacks, lower the level of PAI (as well as lowering cholesterol, their primary known action). An natural enzyme called subtilisin may also lower PAI levels (see Appendix).
A significant portion of Chinese herb therapies, particularly those in current use, involve the action of "vitalizing blood circulation." The Chinese terms "huoxue" (activate blood) and "huayu" (to transform stasis) are often used in depicting the action of the herbs. The former term suggests that the circulation of blood is enhanced by alleviating restrictions, such as dilating blood vessels, enhancing cardiac output, reducing thick substances in the blood (e.g., excess lipids), and inhibiting clot formation; the latter term suggests removal of clots. However, the effects on blood circulation may vary considerably among the herbs, as there are numerous types of active constituents, and there are several possible combinations of actions that each herb might exert on the circulatory system. For the most part, Chinese herbalists base their decision to use certain herbs on the reputed benefits that were described prior to availability of any laboratory or clinical tests that could ascertain the mechanism or actual impact of the therapy on blood properties (hemorrhology).
A list of commonly used Chinese herbs is presented in the table below, taken from the Materia Medica category of herbs that vitalize blood and transform stasis (1, 2). Some of the herbs in this table have recently been added to the list of blood vitalizers, such as crataegus and pueraria. The "additional properties" of the herbs listed in the second column reflect traditional Chinese categories of therapy or other common descriptions.
TABLE 1: Commonly Used Chinese Herbs that Vitalize Blood
| Herb Designations | Additional Properties | Comments |
| Achyranthes niuxi Achyranthes bidentata | nourishes blood, dispels wind-damp (alleviates arthralgia) | Commonly used for rheumatic syndromes affecting the lower body; a directing herb to move blood from upper to lower body. |
| Carthamus honghua Carthamus tinctorius | regulates menstruation, alleviates pain of injuries | Combined with persica in treatments of blood stasis causing pain. |
| Cnidium chuanxiong Ligusticum chuanxiong | dispels wind, regulates qi, controls pain, nourishes blood | It is the main herb used for headache pain; used in most formulas for blood stasis syndromes and in many formulas for nourishing blood. |
| Corydalis yanhusuo Corydalis ambigua | controls pain, regulates qi | Mainly used for abdominal pain syndromes, including menstrual pain. |
| Crataegus shanzha Crataegus pinnatifida | helps digestion of meat and fats, resolves phlegm | This herb has modern uses of promoting blood circulation and removing excess blood fats; traditionally used to promote digestion. |
| Curcuma yujin Curcuma aromatica | regulates qi, disperses accumulations | Mainly used in cases of stagnation with accumulation, including treatment of phlegm masses and other lumps. |
| Cyathula chuanniuxi Cyathula capitata | regulates menstruation | Mainly used for pain associated with menstruation. Increasingly used more generally for abdominal blood stasis. |
| Frankincense (or mastic) ruxiang Boswellia carterii | controls pain, relaxes muscles, reduces bleeding | Mainly used in treatment of injuries, usually combined with myrrh. |
| Leonurus yimucao Leonurus heterophyllus | regulates menstruation, disperses water accumulation | Most often used for women's reproductive system disorders; also used for cardiovascular diseases. |
| Millettia jixueteng Spatholobus suberectus | nourishes blood, alleviates numbness, relaxes tendons | Modern applications are mainly for anemia; traditionally used for numbness of the legs in the elderly. |
| Moutan mudanpi Paeonia moutan | clears heat | Commonly used for regulating menstruation and for alleviating bleeding due to heat in the blood; also used for abdominal blood stasis. |
| Myrrh moyao Commiphora sp. | controls pain, disperses swellings, promotes tissue regeneration | Used mainly for injuries (along with frankincense) and for swellings (such as abscesses). |
| Notoginseng sanqi Panax notoginseng | stops bleeding, tonifies qi, nourishes blood | Especially used for bleeding (and bruising) due to injuries, used raw; when fried, it is a tonic for qi and blood. |
| Red peony chishao Paeonia obovata | clears heat, cools blood | Especially used for blood stasis syndrome with blood heat, often combined with salvia and/or moutan. |
| Persica taoren Prunus persica | moistens the intestines | Often used for abdominal blood stasis accompanied by constipation; combined with carthamus for many blood stasis disorders. |
| Pueraria gegen Pueraria lobata | regulates muscles, alleviates thirst | Commonly used in treatment of muscle tension affecting neck and shoulders; a new use is treating cardiovascular disease and stroke. |
| Salvia danshen Salvia miltiorrhiza | cools blood, nourishes blood, sedative | Primarily used for cardiovascular disorders and for liver fibrosis; also useful as a sedative. |
| Sparganium (or scirpus) sanleng Sparganium stoloniferum | regulates qi, disperses mass | Mainly used for hard masses (blood stasis type), especially those in the abdomen; usually combined with zedoaria. |
| Tang-kuei danggui Angelica sinensis | nourishes blood, moistens intestines, regulates menstruation | This is the most widely used blood nourishing herb; it is also especially used for treating all types of menstrual disorders and blood stasis. |
| Typha (or bulrush) puhuang Typha latifolia | astringent, cools blood, stops bleeding | Most often used for menstrual disorders; the raw herb vitalizes blood, the fried herb is a hemostatic. |
| Vaccaria wangbuliuxing Vaccaria pramidata | regulates menstruation, disperses swelling | Primarily used for swelling in the lower abdomen, particularly for women's disorders. |
| Zedoaria ezhu Curcuma zedoaria | regulates qi, disperses masses, benefits stomach functions | Mainly used for hard masses, in combination with sparganium; also for digestive disturbance with distention. |
During the past century, research has been carried out on several of these herbs, such as evaluations of cardiovascular and hemorrhologic effects in laboratory animals and in some clinical trials. One problem with most of these recent tests is that the quality of their design, conduct, and reporting (more specifically, the lack thereof) is such that the results are difficult to interpret. In addition, it is often the case that the dosage of herb materials used in the studies far exceeds that which is commonly administered in clinical practice outside of China, so that the effect of the therapies on blood circulation in such circumstances may be substantially less than observed in the studies.
Nonetheless, it is worthwhile to examine the types of reports found in this literature to aid in understanding what Chinese doctors expect the herbs to accomplish for their patients. In a summary of research published from 1984-1987 (relayed in a book published in 1991), two herbs (salvia and cnidium) and two formulas (Shengmai San and Guanxin II) were featured (3). The effects observed were often similar, and those for salvia, the herb studied most extensively as a single remedy, are outlined here:
TABLE 2: Effects of Salvia
| Pharmacological Effect on Cardiovascular System | Pharmacological Effect on Blood | Clinical use |
| Increase coronary blood flow (clinical). Dilate coronary arteries, decrease resistance to blood flow, and increase coronary blood flow (laboratory). Facilitate collateral circulation; enhance redistribution of blood; improve microcirculation; increase tension and decrease fragility of capillaries (laboratory). Reduce size of myocardial infarction (laboratory). | Inhibit platelet aggregation induced by ADP; increase platelet cAMP; activate plasminogen and fibrinolysis systems to promote conversion of fibrin (laboratory). Decrease blood viscosity; increase erythrocyte electrophoretic rate; improve microcirculation (clinical). | Relieve angina and improve ECG in cases of coronary heart disease. Relieve symptoms of ischemic stroke. Reduce disseminated intravascular coagulation in epidemic cerebrospinal meningitis and epidemic hemorrhagic fever. |
If some of these benefits can be attained by use of the herb, the therapeutic effects would be more far-reaching than, for example, the simple anti-coagulant action of warfarin therapy based on blocking vitamin-K activated factors. One can imagine using salvia in place of or in addition to warfarin to benefit the circulatory system. Salvia is the most extensively used Chinese herb in the treatment of chronic cardiovascular diseases in China today. Recently, it has been proposed that some of the benefits of salvia can be attributed to a protective effect against homocysteine-induced damage to the endothelium of the vessels (4). The actions of salvinolic acid-B, one of the main active components of salvia, and of ligustrazine, the main active component of cnidium, include reducing PAI levels (5, 6).
In an appendix summarizing the pharmacological and clinical effects of herbs presented in monographs, the book Pharmacology and Applications of Chinese Materia Medica (7) lists the following commonly used herbs as having cardiovascular benefits (herbs repeatedly mentioned with three or more of the specified actions are underlined).
TABLE 3: Commonly Used Chinese Herbs Affecting Blood Flow
| Anti-Atherosclerotic | Anti-Coagulant | Anti-Lipemic | Cardiotonic | Coronary Vasodilator | Peripheral Vasodilator |
| Cnidium Tang-kuei Garlic Polygonatum Turmeric Ganoderma Typha Capillaris Alisma Gardenia Licorice Ho-shou-wu Curcuma | Cnidium Tang-kuei Salvia Garlic Pueraria Carthamus Turmeric Notoginseng Capillaris Atractylodes Zedoaria Cinnamon bark Lysimachia | Citrus Salvia Garlic Eucommia Polygonatum Turmeric Ligustrum Typha Crataegus Capillaris Alisma Bupleurum Rhubarb Lycium bark Licorice Lycium fruit Ho-shou-wu Hu-chang Lonicera Morus leaf Epimedium | Citrus Cnidium Eucommia Ganoderma Notoginseng Schizandra Cyperus Scrophularia Yu-chu Chih-ko Chih-shih Psoralea Hoelen Aconite Forsythia Deer antler Achyranthes Ligustrum Ginseng | Citrus Cnidium Tang-kuei Salvia Pueraria Carthamus Polygonatum Ganoderma Ligustrum Typha Notoginseng Crataegus Capillaris Alisma Eleuthero Fritillaria Psoralea Rehmannia Fo-shou Coptis Astragalus Hu-chang Lysimachia Chrysanthemum Cinnamon bark Morus branch Gastrodia Corydalis Leonurus Epimedium | Cnidium Tang-kuei Salvia Eucommia Pueraria Carthamus Typha Ginseng Morus bark Gastrodia Schizandra Scrophularia Atractylodes Aconite Coptis Astragalus |
In addition, the book provides a huge listing of herbs that lower blood pressure. Among the herbs listed above, the ones occurring repeated are: the blood-vitalizing herbs cnidium, tang-kuei, salvia, crataegus, carthamus, carthamus, turmeric, notoginseng, and pueraria; the tonic herbs eucommia, ligustrum, ganoderma, and polygonatum; and herbs in miscellaneous categories: garlic, alisma, and capillaris. Some of the herbs mentioned in the table are botanically related: yu-chu is a type of polygonatum; curcuma is a variety of turmeric; ginseng is a relative of notoginseng; chih-ko, chih-shih, and fo-shou are related to citrus; in addition, there are three parts of the mulberry plant listed: morus bark, morus leaf, and morus twig. It is possible that overlapping active ingredients occur in these related materials, and that the number of unique active components that yield broad cardiovascular benefits are limited.
The Chinese formula called Coronary Heart II (Guanxin II) has the main ingredients salvia, cnidium, and carthamus, which, when taken together, express all six actions depicted in the table. A modern preparation for improving blood flow to the heart and brain for persons suffering from heart attack and stroke is comprised of five ingredients listed in the tables: notoginseng, carthamus, cnidium, pueraria, and crataegus. In a treatment for prevention of restenosis (narrowing of the artery) following insertion of a stent, Chinese researchers administered a formula with the blood-vitalizing herbs salvia and pueraria, plus astragalus, rehmannia (cooked and raw), lycium fruit, loranthus, and ophiopogon along with anticoagulant therapy (aspirin and ticlopidine). It was noted that C-reactive protein (which stimulates platelet sticking) was much lower in the group taking the herbs (8).
Although Chinese herbs, especially salvia, cnidium, carthamus, and pueraria, are extensively used in China to treat people who might otherwise receive warfarin, there is little evidence that these or other Chinese herbs have a potent anticoagulant action comparable to that of warfarin or even aspirin. Traditional Chinese literature provides some cautions for use of the herbs in cases of bleeding, such as during menstruation, because of concern of increasing total blood loss, indicating that clotting time may be prolonged somewhat.
There is some evidence to suggest that Chinese herbs can interact with warfarin, but the number of reports is quite low and evidence of the effects is limited. Salvia is the herb suggested to have such an interaction, but only three cases have been reported in the literature (9), despite its widespread use by persons who have blood coagulation problems; the three cases involved large changes in INR, however. One clinical report of interaction with warfarin involved tang-kuei (10); a laboratory study showed limited interaction (11). Herbs mentioned briefly in the literature as potentially interacting with warfarin are garlic, ginseng, and ginkgo leaf.
In a recent evaluation of reports about herb-drug interactions, few publications contained sufficient data for making an evaluation of actual interaction, and, of those, only 18 out of 108 involved warfarin, and most of those involved the Western herb St. John's Wort (11). In a survey of people in Hong Kong starting warfarin therapy, it was found that about one in four were taking Chinese herbs (12). Their INR values, rather than being enhanced, were slightly lower, and this corresponded with a somewhat lower dose of warfarin taken by those who were using the herbs.
Thus, it may be possible for these herbs to be used along with warfarin therapy, so long as monitoring of the INR is maintained in order to detect rare interactions. When the herbs provide additional benefits to the cardiovascular system (aside from simple anti-coagulation), the effect of the total treatment may be improved compared to the drug therapy alone. It is important to consider that when the PT test is carried out, it measures the coagulation of blood that is removed from the body. The test does not indicate any conditions of the vascular system that may lead to induction of clotting; yet, such conditions may be very important in determining whether or not a serious clotting event will occur. Those other conditions may be addressed by the herbs.
Alternatives to warfarin are in advanced stages of drug research. One of the central problems with use of warfarin is its limited dosage range for therapeutic benefit and safety and its apparent susceptibility to interactions. These issues are related to the nature of the warfarin molecule, being somewhat similar to several naturally occurring compounds, and its interaction with at least six vitamin-K dependent clotting factors. As an example of a potential alternative, the drug ximelagatran (brand name: Exanta) is metabolized to yield melagatran, which inhibits only thrombin. This may allow patients to take a single prescribed dosage without having to frequently monitor the INR and adjust dosage; in addition, it appears to have a low level of interactions. As of this writing, the drug is not approved in the U.S., but is being used for some limited applications in Europe (short-term therapy for leg surgeries). A potential role for Chinese blood-vitalizing herbs will still be present even if this (or other alternatives to warfarin) provides a safer anticoagulant therapy.
In the search for natural blood thinning agents, a substance obtained from natto (a type of fermented soybeans used as a food in Japan) has been proposed as useful. The substance is called natto-kinase (renamed recently as subtilisin NAT), and is administered in doses of about 100 mg, derived from about 100 grams of natto. Most products are assayed to determine their activity in fibrinolytic units (FU), and a typical recommendation is to obtain 2,000 FU per day.
Unlike warfarin, which has the focus on preventing clotting, natto-kinase appears to have the primary effect of breaking up clots, via a fibrinolytic activity; it interacts with the plasminogen system, by reducing the PAI level and increasing the amount of plasmin. This substance was isolated by Japanese researcher Hiroyuki Sumi in 1980 while he was studying at the University of Chicago Medical School. Notto-kinase is produced by the bacterial culture (Bacillus subtilis) that ferments the soybeans; it is also found in the Chinese fermented soybean called heidou or douchi (subtilisin DFE), but is not found in unfermented soybeans.
Other subtilisin molecules are proteases used commercially, for example, as additions to laundry detergent (to break down protein stains) and to contact lens cleansers (to remove protein contaminants that cloud the lenses). The fermented soybean subtilisins appear specific for breaking down fibrin.

December 2004