 Young xanthium plant. | |
 Mature xanthium plant with fruits. |  Close-up of xanthium fruits. |
SAFETY ISSUES AFFECTING CHINESE HERBS:
The Case of Xanthium
Practitioners of Chinese herbal medicine have been alerted in recent years to safety concerns about some of the medicinal materials that had been relied upon previously. The most significant issue has been the revelation that plants in the Aristolochiaceae family may contain an organic acid, aristolochic acid, which, in rare and often unexplained cases, causes a severe renal reaction in consumers of the herbs (see: Are Aristolochia plants dangerous?). For many years, the possibility that herbs containing this compound were actually responsible for the adverse reactions was debated, but the issue has largely been settled by intensive investigation, implicating aristolochic acid as a contributor to renal failure in some individuals. Another issue that has arisen is the case of pyrrolizidine alkaloids (PAs), which, with prolonged use of significant doses, may cause a serious liver reaction (see: Safety issues affecting herbs: pyrrolizidine alkaloids). The potential for cardiac reactions to ephedrine from ma-huang (see: Safety issues affecting herbs: the case of ma-huang) and to synephrine from chih-shih (see: Synephrine: is chih-shih toxic?), has been raised. These alkaloid reactions are dose-dependent, where both compounds have been isolated and used in high doses for weight loss or other non-TCM applications. Questions about the safety of ginseng and other common herbs have also been mentioned.
Practitioners of Chinese medicine who prescribe herbs have had mixed reactions to these matters. Some have argued that the herbs are safe except when substantially misused, and that their safety compared to drugs is so great that it is unfair to single out rare problems with them. Others have reacted to the alerts by strictly avoiding herbs for which safety issues have been raised. Sometimes this avoidance is carried on to the extent of ignoring evidence that exonerates the herbs from a causative role in the purported adverse effects, such as the absence of hypertensive effect from ginseng when used at normal doses (see: Safety issues affecting Chinese herbs: the case of ginseng, and The nature of ginseng).
The various concerns about safety have been described in ITM literature, with an effort to carefully detail all contributing factors to the issue, so that practitioners can make a more sound judgment about using the herbs. In addition, the investigations into herb safety can influence herb formulations provided by ITM or other organizations. In an effort to head off unexpected problems in the future, safety questions are being explored proactively, so that prescribers of Chinese herbs can be fully aware of the issues at hand.
In this article, the safety of xanthium is explored. Xanthium is extensively used for the treatment of sinus congestion (see Appendix), a problem frequently presented by patients seeking natural health care. Xanthium has not been blamed for any harmful effects among Western consumers, and has not been banned by any health department in any country. Yet, it is an herb that should be investigated, as will be revealed here.
Xanthium refers to the fruits of Xanthium strumarium, the common cocklebur. Xanthium is from an ancient Greek word xanthos meaning yellow; strumarium means "cushionlike swelling," in reference to the seedpods which turn from green to yellow as they ripen (later they become deep yellow to brown). Cocklebur is a reference to the cockle shell-like appearance of the pods and their "burry" nature. The pods (fruit) are used in Chinese medicine and known as cangerzi. Cang is based on the character that means deep green; er means ear, this referring to the appearance of the leaves like green pig's ears (see photo, below); zi is the fruit.
 Young xanthium plant. | |
 Mature xanthium plant with fruits. |  Close-up of xanthium fruits. |
Several Chinese herb guides list xanthium as being somewhat toxic without any explanation or specific cautions. The usual place where toxicity of an herb is mentioned is along with the herb's nature, such as warming or cooling; xanthium is classified as having a warm nature. Some examples of how toxicity of xanthium is presented in various English language texts are listed in Table 1.
Table 1: References to xanthium (cangerzi) in English language guides (1-9).
| Title | Toxicity Related Statements |
| Oriental Materia Medica | no mention of toxicity |
| Chinese-English Manual of Commonly Used Herbs in Traditional Chinese Medicine | mildly toxic |
| Thousand Formulas and Thousand Herbs of Traditional Chinese Medicine | slightly toxic |
| Chinese Herbal Medicine Materia Medica | toxic. "Overdosage may cause nausea, vomiting, diarrhea, and/or abdominal pain....The toxic ingredients are changed by decoction and are not significantly present in the herb after it has been decocted or subjected to high heat." |
| Chinese Herbal Medicine: Chemistry, Pharmacology, and Applications | "Xanthium is defined as a toxic herb in Chinese Pharmacopoeia….Patients taking over 100 g of the fruit may complain of malaise, headache, and gastrointestinal disturbance in 12 hours. Other toxic symptoms in humans include dizziness, drowsiness, coma, and generalized tonic seizure, appearance of jaundice, hepatomegaly, impairment of liver function, proteinuria, cylindruria, and hematuria. The toxic substance is soluble in water and may be reduced or abolished by rinsing the fruit in water. |
| Advanced Textbook on Traditional Chinese Medicine and Pharmacology | toxic. "Overdose may cause intoxication." |
| Pharmacopoeia of the People's Republic of China (1988) | no mention of toxicity |
| A New Compendium of Materia Medica | "with a little toxin!" |
| The Illustrated Chinese Materia Medica, Crude and Prepared | toxic. "The toxin is removed by stir-frying." |
As can be seen in these examples, the comments on xanthium toxicity range from no mention at all, to brief mention of slight or mild toxicity, to simply calling it toxic. There is caution about overdosage (usual dosage is listed as 3-10 grams), and a suggestion that the toxin is removed by washing with water, by decocting, by subjecting to high heat, or by stir-frying, though no evidence is provided in these sources to prove that potential outcome. The idea, as conveyed in Chinese Herbal Medicine Materia Medica, that the herb is detoxified by decocting seems to be contradicted: high doses are almost always administered by decoction (as this is the only method to easily provide high doses), and these are the preparations that are said to produce adverse reactions or toxicity. In laboratory animal studies, hot water extracts of the herb, similar to decoctions, produce the toxic reactions.
In Western literature, xanthium is not described as a medicinal herb, but is a well-known toxic herb (rated as highly toxic) for grazing animals (e.g., cattle, pigs, horses, poultry). The common cocklebur is particularly known to American ranchers: it is found throughout the United States from the south of Canada to Mexico and is a common weed found in corn and soybean fields. A related herb, Xanthium spinosum, has been dubbed one of the world's worst weeds because the plants, like those of Xanthium strumarium, can quickly become dominant in an area due to their prolific seed production and high germination and survival rates.
Cocklebur readily invades pasture and grazing lands, the shorelines of shallow ponds, lakes, and streams (where animals seek water), and any marshy flatlands that are moist during much of the year but dry out during the summer. The transition from wet to drier conditions stimulates the plant germination and growth. The hooked spines of the fruits make them easily carried from place to place by attaching to animal fur or human clothing. The burry fruit capsule contains two seeds; only one seed germinates the first year. Germination is delayed in the second seed until the following year, giving each fruit capsule two years to yield viable plants.
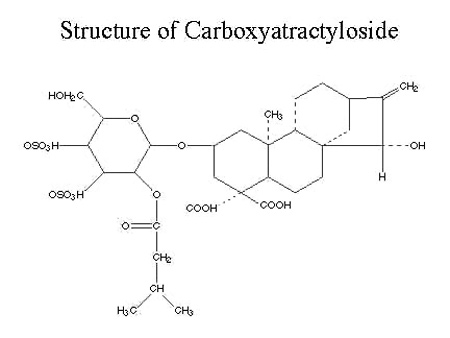
The main toxic compound isolated from Xanthium strumarium has been identified as carboxyatractyloside, a kaurene glycoside (10-15; see structure diagram below). This compound, isolated and identified in 1975, was previously called xanthostrumariam, a name still seen in the Chinese literature. Cocklebur seedlings, often consumed by grazing animals, are high in carboxyatractyloside (CAT) until the emergence of their first true leaves after which the compound is present in the whole plant in reduced quantities. Even though the content of CAT in the mature plant is reduced, hay containing mature xanthium plants has caused toxic reactions in animals. CAT is a plant growth inhibitor; it has been hypothesized that it functions in a germinating cocklebur seed to keep the second seed in the fruit capsule dormant so that its development is delayed until the next year. Cocklebur fruits, the portion used in Chinese herbal medicine, have the risk of high carboxyatractyloside content. In fact, the spines are particularly rich in this compound.
When ingested in sufficient quantities by animals, CAT by itself or xanthium that contains CAT, produces hypoglycemia and hepatic damage, the latter possibly due to increased vascular permeability in response to severe hypoglycemia. The mechanism of action has been proposed to be an uncoupling (disruption) of oxidative phosphorylation, a process essential to the cell's energy metabolism and transfer system. In addition to CAT, potentially toxic ingredients of xanthium include several sesquiterpene lactones (e.g., guaianolides, germacranolides, and elemanolides) that can cause vomiting, weakness, tremors, weak pulse, a loss of appetite, and convulsions in high doses.
The quantities of xanthium ingested by foraging animals can be quite large. In the case of the seeds, a quantity of 0.3% of the animal's body weight can yield toxic symptoms. Translated to a human body weight of 70 kg, this corresponds to 210 grams of the seeds, a huge amount compared to the dose of fruits used in Chinese herbal medicine (typically 3-10 grams, sometimes less). Two cases of toxicity to humans were reported in the Chinese literature; one, involving an adult who consumed more than 100 grams in one day, and another a child, fed 300 grams over two days (16). Thus, there appears to be a large safety margin between the recommended dose and the toxic level with regard to acute toxicity. In America, the seeds in the pods were eaten raw or cooked by Native Americans as a food, no doubt in small quantities, but without reported adverse effect. Nonetheless, it is possible that moderate doses of xanthium consumed over an extended period of time (many weeks, as when treating seasonal allergic rhinitis) might be able to yield some toxic effects in sensitive individuals. Therefore, limiting exposure to CAT is important when using the herb as a medicine.
An analysis of xanthium fruit by Jiang Xiao and Sui Jinjiang (working at the pharmacy of Yantai Yuhuangding Hospital, in Shandong) indicated that the toxic principles were water soluble (17). This was demonstrated by finding heightened toxicity of a water extract derived from the defatted fruit but no toxicity of the fatty portion, which makes up about 39% of the dried fruit. The toxin was identified as a glycoside (most likely, this is CAT, though the institute was not able to identify the specific compound). Heat treatment, at temperatures beyond boiling, could inactivate it. The authors stated that the fruit should be stir-fried to eliminate toxicity. This is one of the standard processing methods for xanthium fruit, though it is not always employed. The spines of xanthium are thought to contain more of the toxin then the rest of the fruit shell, so stir-frying to remove the spines is considered a suitable method for removing toxic potential.
According to Jin Chuanshan and his colleagues, at the Department of Pharmacy, Anhui College of TCM, since ancient times it has been the practice to remove the prickles from the crude herb (18). To evaluate the value of that practice, they tested the toxicity of xanthium fruit in mice using the plain dried xanthium fruit, stir-fried xanthium fruit, and stir-fried fruit that was then freed of prickles by grinding and sieving. The tests indicated that the stir-frying alone reduced the toxicity by half, but that removal of the prickles led to no detectable toxicity with the test used.
Chinese researchers have suggested that the toxin in xanthium is a protein, to explain its diminished effect with heating, and others have thought that washing the fruit would eliminate the toxic component because it is water soluble (a Chinese report in 1960 stated that water washing removed the toxicity, but this has never been substantiated by subsequent experiments). In fact, it appears that the compound of primary concern is not a protein, but a kaurene glycoside, CAT. It is water soluble, but is not destroyed by boiling (decocting) and probably not washed away by simple rinsing. Rather, removing the prickles appears to be the best way to reduce the toxic component, which is partly accomplished by stir-frying alone.
The Illustrated Chinese Materia Medica, Crude and Prepared (9) displays a picture of stir-fried xanthium fruit that retains the spikes (see Figure 5), as an indication of a pharmacy preparation. In the Pharmacopoeia of the PRC (7), two products are described: one is plain xanthium fruit (no frying) and the other is stir-fried xanthium fruit. The latter is prepared by stir-frying until the pods become yellowish brown followed by removing the spines and sifting. If this latter method is followed (see Figure 6), the toxic potential of xanthium fruit should be eliminated, as evidenced by a laboratory toxicology study (18). There is no evidence that CAT, which is greatly reduced by this processing (though some remains in the seeds), is an active component for the treatment of rhinitis, so its reduced content simply improves the safety of the herb. Excessive stir-frying, however, could destroy other substances in xanthium fruit that may be desirable; the finished product should be of light color. Stir-frying of the whole fruits, where the spikes are the part exposed directly to the hot surface, makes the spikes dry and brittle, thus easily removed by mechanical means.
To assure the safe use of xanthium, it should be processed by stir-frying, as described in the Pharmacopoeia of the PRC, to eliminate most of the prickles. Water washing of the fruits or decocting is not a satisfactory detoxification method; stir-frying with retention of most of the fruit spikes is not as effective in eliminating the toxic component as when spikes are removed. There is no evidence that the residual amounts of CAT or other compounds are a threat to human health. Still, as a further precaution, the dosage of xanthium should be limited to the range (3-10 grams/day) normally recommended in Materia Medica guides whenever there is prolonged use of the herb, thus allowing a 10-fold margin of safety compared to the dose reported to have caused a significant reaction in a human (100 grams). By the combination of correct processing and limiting the dose, the risk (as observed in animals grazing on the plants) should be eliminated. Practitioners who use crude herbs can check the xanthium pods for the condition of the prickles. Manufacturers who produce extracts or powders need to check the pods prior to processing the finished product.
December 2002
Xanthium was first described in the Shennong Bencao Jing (ca 100 A.D.), where it was attributed several favorable properties (19):
Xanthium is sweet and warm. It mainly treats wind-cold headache, wind-damp generalized stiffness and pain, contracture-pain of the limbs, and gangrenous flesh. Protracted taking may boost the qi, sharpen the ears and eyes, strengthen the will, and make the body light.
Thus, the herb appears suitable for both short-term use in treating painful wind disorders of the head and limbs, and long-term use to benefit the body functions (reference to making the body light indicates it was thought to be an herb for the immortals). Nonetheless, this herb is rarely found in any of the traditional formulas that are handed down to us today. Only one formula is frequently cited, and that is (3):
| Xanthium Formula (Canger San or Cangerzi San) | |
| Magnolia flower | 30 g |
| Angelica | 30 g |
| Xanthium fruit | 15 g |
| Mentha | 3 g |
The herbs are ground to powder, and taken 6 grams each time with tea made from chive bulb (congbai) and green tea. The amounts indicated above are sufficient for making 13 doses, usual use is to take 2-3 doses per day. This formula comes from Chong Ding Yan Shi Ji Sheng Fang, which is Chong Dingyan's version of the famous book Ji Sheng Fang. The three main herbs of Xanthium Formula were compared and contrasted by Yang Yifan, in her book Chinese Herbal Medicines (20). As to xanthium, she writes:
Xanthium is bitter and warm, and enters the lung meridian. It is effective for drying dampness. Its warm and bitter nature give it a spreading ability, so it can spread the qi and expel wind....It is particularly used when there are large amounts of clear nasal discharge and itchiness of the nasal passage, which is considered the result of wind invasion....It can treat headache due to wind-dampness. It has a drying nature but is not harsh, so it is also used in some skin diseases where the skin lesions are characterized by itching and weeping.
Xanthium is classified in modern Materia Medicas as either an herb for dispelling wind chill (along with angelica and magnolia flower, for example) or an herb for dispelling wind damp. Its modern uses are mainly for allergy-type disorders, specifically allergic rhinitis and atopic dermatitis (urticaria), and their chronic counterparts-chronic paranasal sinusitis and chronic eczema. It is usually the ingredient of a large formula, so its role in the therapeutic benefit is difficult to determine. In one study of urticaria treatment (21), the decoction was comprised of four main herbs, with xanthium, licorice, red peony, and earthworm. In a study of rhinitis treatment, a pill made from the extracts of xanthium, gypsum, angelica, and scute was utilized. In both those studies, positive results, without adverse effects, were declared. According to a report relayed by Zhu Youping (5), xanthium powdered and made into pills or extracted and made into tablets (in both cases, the dosage administered was 3 grams each time, three times daily) was used for a two week treatment for chronic paranasal sinusitis, with satisfactory results claimed. Similarly, an alcohol extract of the herb, dried and made into tablets, with 3 grams extract each time, three times daily, was claimed beneficial for those with allergic rhinitis.
While several chemical constituents of xanthium have been isolated, the active components of this herb in relation to its traditional applications have not been determined and there is little information about its pharmacology that might help evaluate the potential of xanthium to successfully treat various disorders. The sesquiterpene lactones, such as xanthanol, isoxanthanol, xanthinin, and xanthumin may contribute some of the apparent anti-inflammatory and anti-allergy activities.


Figure 6 Xanthium processed by stir-frying followed by grinding to remove prickles.