| INTERNET
JOURNAL OF THE INSTITUTE FOR TRADITIONAL MEDICINE AND PREVENTIVE HEALTH CARE |
|
TREATMENT OF DIABETES WITH Web Posting Date: January 2003 Key medical terms: diabetes mellitus, NIDDM (type 2 diabetes, non-insulin dependent) Key Chinese medical references: deficiency and impairment of qi, yin, and yang Chinese herbs: alisma, anemarrhena, astragalus, atractylodes, dioscorea, ginseng, ho-shou-wu, hoelen, lycium, platycodon, polygonatum, pueraria, rehmannia, salvia, scrophularia, trichosanthes Chinese formulas: Baihu Jia Renshen Tang, Liuwei Dihuang Wan, Bawei Dihuang Wan, Maimendong Yinzi, Fangfeng Tongsheng San, Yu Quan Wan, Xiao Ke Wan |
|
SUMMARY: Diabetes is out of control in the U.S., with incidence rates as high as 15-20% in some population groups (e.g., the elderly, blacks, Hispanics, and Native Americans), and with substantial increases in all age and racial groups in the past few years. Chinese medicine, relying mainly on herb formulas, but also on acupuncture, has been utilized extensively in East Asia to reduce blood sugar in persons with diabetes, especially those with the most common type (non-insulin dependent diabetes mellitus, NIDDM). Based on extensive laboratory and clinical evaluations, about 20 herbs have emerged as primary candidates for treatment. These herbs have been utilized in a small number of traditional formulations for centuries, both for treating obvious diabetes and for other disorders that produce similar symptoms. Acupuncturists have identified about 20 points on the body that appear to be effective in lowering blood sugar; typically, a dozen of these points are selected for treatment at one time. Although more clinical research needs to be done to demonstrate the level of effectiveness of the herbs and acupuncture, these methods of therapy are currently available in many locations in the Western cultures as a result of the increasing acceptance of Chinese medicine during the past three decades. This article outlines the history and development of Chinese approaches to diabetes and reveals the currently accepted concepts. A second article will present treatment for secondary effects of diabetes, such as impairment of circulation and resulting damage to the eyes, peripheral neuropathy, and increased risk of heart attack.
|
|
TREATMENT OF DIABETES WITH I. Lowering Blood Sugar Diabetes is a major health problem worldwide, but particularly in America. It is estimated that about 2.1% of the world's population has diabetes, but the disease is out of control in America. In the U.S., current estimates are that over 6% of the adult population has the disease, 99% of them with the type 2 diabetes mellitus (late onset or non-insulin-dependent: NIDDM). Type 2 diabetes usually appears around the age of 50 or later, though it can occur during teen years in some cases of obesity. The incidence rate becomes quite high among elderly Americans (20% for those over the age of 65) and in groups with genetic or other predispositions including blacks (14%), hispanics (15%), and Native Americans (19%). Furthermore, the overall incidence of diabetes is growing, apparently because of increased rates of obesity. 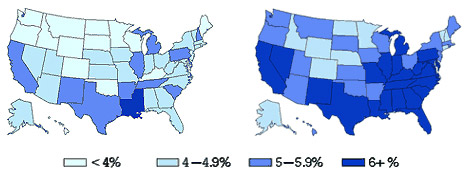 CDC data on prevalence of diabetes across the United States in 1994 (left) and in 2000 (right). The rise in diabetes rates is striking. In the year 2000, no states had less than 4% of the population with diabetes, and only 10 states had under 5%. Despite the major medical advances in rapid and easy monitoring of blood sugar and treatment with drugs, diabetes remains a serious problem. Blood sugar regulation that can be attained by standard methods, particularly when patients are not fully compliant with all medical recommendations, is often not adequate to avoid common secondary effects of diabetes, including cardiovascular diseases, degenerative eye conditions, limb numbness and pain, skin ulceration, and kidney failure. Thus, investigating other avenues for aiding the treatment of diabetes and its secondary consequences is an important undertaking. Although the incidence of diabetes is far lower in China than in the U.S., predictions are that China and the rest of southeast Asia will rapidly become the world's main site of diabetes cases (by the year 2025) due to the combined high population and change in lifestyle as the countries modernize. The disease has been known since ancient times and it has been a subject of considerable laboratory and clinical research in the Orient. So, the methods of Chinese medicine will no doubt play an important role in the coming years in the population of East Asia. Chinese medical treatment of diabetes includes herbal prescriptions, acupuncture, and dietary recommendations. There is not a single established treatment for diabetes, so it is necessary to review the traditional medical ideas about diabetes and the research that has been conducted to date to give guidance in using these medical therapies. This part of the two-part series focuses on treatments to lower blood sugar; part II focuses on treatment of secondary manifestations of diabetes. Practitioners of Chinese medicine in the U.S. and other Western countries often have more time to spend consulting with their patients than do medical doctors. This extra time gives an opportunity for exploring with the patient the key roles of exercise and dietary control in limiting the impact of diabetes and preventing its development with aging for those who do not currently have the disease. While acupuncture and herbs are an important option for these patients, it is clear from the evidence that exists that as much or more can be accomplished through changes in behavior. It is necessary for practitioners to keep current with information about dietary advice, as some concepts that were common just a few years ago have turned out to be incorrect or misleading, and are replaced by new approaches backed by recent research. BRIEF HISTORY OF CHINESE MEDICINE AND DIABETESChinese medicine owes its current stature to the long history of its practice, dating back more than 2,000 years in a form similar to that utilized today. Chinese physicians appear to have had a reasonably good understanding of diabetes since ancient times. In one of the oldest books about Chinese medical theory, the Huangdi Neijing (1), compiled around 100 B.C., the condition known as xiaoke is mentioned. This is translated today as diabetes or diabetic exhaustion. The literal translation of the term is emaciation-thirst, referring to the disease manifestation when it has gone untreated: namely, one loses body weight despite eating normally, and thirst is persistent. According to this ancient text, the syndrome arises from consuming too much fatty, sweet, or rich food. It is said that it typically occurs among wealthy people: "you ask them to refrain from a rich diet, advice which they may resist." The description fits that of non-insulin-dependent diabetes mellitus. Two of the traditional herbal formulas most frequently used in modern China and Japan for the treatment of diabetes were described in the book Jingui Yaolue (2), which is about miscellaneous diseases, written around 220 A.D. The text described symptoms characteristic of uncontrolled diabetes, including thirst, frequent urination, and loss of body weight. One of the formulas is Rehmannia Eight Formula (Bawei Dihuang Wan; also called Jingui Shenqi Wan), originally indicated for persons who showed weakness, fatigue, and copious urine excreted soon after drinking water; in some cases, this may have been diabetes as we know it today. The other formula is Ginseng and Gypsum Combination (Baihu Jia Renshen Tang); it was indicated originally for severe thirst and fatigue and is considered ideal for diabetes of recent onset. In 752 A.D., the distinguished physician Wang Tao mentioned that diabetes was indicated by sweet urine and he recommended the consumption of pork pancreas as a treatment, implying that the pancreas was the organ involved in the disease (3). Further, he suggested that the urine of diabetes patients should be tested daily (by tasting for sweetness) to determine the progress of the disease and its treatment. Liu Wansu (ca. 1120-1200 A.D.) propounded the theory that diseases are usually caused by heat in the body, which should be countered by herbs that had a cold nature (4). One of his published formulas for diabetes, Ophiopogon and Trichosanthes Combination (Mainendong Yinzi), is traditionally described as clearing heat and nourishing yin. It is comprised almost entirely of herbs that have been shown by modern research to lower blood sugar. Another of his formulas, Siler and Platycodon Formula (Fangfeng Tongsheng San), is recommended by many Japanese doctors for treatment of obesity and accompanying type 2 diabetic syndrome (5). By the latter half of the 20th century, there were about 200 standard prescriptions recorded as suitable for treating diabetes (6). The majority of these may be viewed as combinations that rely primarily on about two dozen anti-diabetic ingredients (see Table, page 4) plus a small number of auxiliary herbs. These other herbs are understood to have complementary properties (assist the function of the main herbs) or are aimed at treating a specific manifestation of the disease. The main traditional prescriptions brought forward include Rehmannia Eight Formula and its simplified version Rehmannia Six Formula; Ginseng and Gypsum Combination, and Ophiopogon and Trichosanthes Combination. A theory has arisen as to how diabetes progresses (7, 41). The disease begins with a deficiency of yin. This seems contradictory to the appearance of the patient, who often shows obese constitution and low metabolism, signs that would correspond to excess of yin and deficiency of yang. However, the patients with early stage of diabetes actually have a hyperactive metabolism that does not provide useful energy. Hence, the food nutrients are not successfully utilized; hunger persists, sugar pours out in the urine, thirst develops, and there may be easy sweating. This yin deficiency then generates heat that becomes pathological and then parches the yin. The imbalance of yin and yang eventually degrades and inhibits the qi, so that qi and yin deficiency co-exist. At this point, secondary effects, such as blood stasis and damp-heat, manifest, causing many serious symptoms (29). Without proper nourishment of qi and yin, yang eventually becomes impaired, and the patient, now with advanced disease, has a combined deficiency of qi, yin, and yang. MODERN HISTORY OF EVALUATING HERBS AND FORMULASThe research on diabetes treatment has been ongoing for several decades, yet remains in the developmental stages due to the complexity of the task at hand. Initial laboratory animal studies of blood-sugar lowering effects of herbs were conducted in China, Korea, and Japan during the period 1927-1952 (6, 13). Several commonly used herbs were shown to lower blood sugar, including yin nourishing rehmannia, scrophularia, ho-shou-wu, and yu-chu; qi tonifying ginseng, atractylodes, and polygonatum (haungjing, which also nourishes yin); and heat clearing herbs, such as phellodendron, coptis, lycium bark, lonicera, and alisma. This hypoglycemic effect occurred when the herbs were used to treat blood sugar increases induced by epinephrine, which acts as a stress hormone. Since the 1960s, a much invigorated program of diabetes research arose. New laboratory evaluations were made possible by the finding that the toxic chemical alloxan selectively destroys the beta cells of the pancreas. Thus, mice, rabbits, or other laboratory animals treated with this compound suffer from a diabetic syndrome quite similar to that of a person who has insulin-dependent diabetes (type I, early onset). Dr. S. Nagayoshi was able to report that Rehmannia Eight Formula reduced blood sugar in alloxan-treated rabbits in a 1960 journal report (6). Comparing the herbal effects in normal laboratory animals with those in alloxan-treated animals provides some indication of the mechanisms by which the herbs affect blood glucose levels; further information is obtained when using the same herbs to treat animals affected by epinephrine. Progress has been made with studies of a genetic strain of mice-first described in 1979-that gain weight unusually and begin developing a type 2 diabetes after about 10 weeks of growth. These mice were used in a study of the hypoglycemic role of ginseng and its active constituents in the traditional formula Ginseng and Gypsum Combination (24). Perhaps the most extensive laboratory investigation of Chinese herbs for diabetes has been carried out by Huang Ray-Ling and his coworkers at the National Research Institute of Chinese Medicine in Taiwan (16). Dr. Huang tested a variety of herb extracts in both alloxan-treated mice and normal mice, in order to compare the impacts of the herbs with or without insulin involvement. To obtain more significant results, blood sugar responses were monitored at different times after administration of herbs, in glucose tolerance tests, and with differing dosages of the herb materials. Herbs that showed significant hypoglycemic action in both alloxan-treated and untreated mice included some that were not commonly used in traditional formulas, such as red atractylodes (cangzhu), cyperus, and phaseolus (mung bean). Herbs that showed a substantial hypoglycemic effect in alloxan-treated mice but little effect in normal mice, however, matched the pattern of traditional herb therapy; they include rehmannia, scrophularia, astragalus, coix, moutan, lycium bark, lycium fruit, trichosanthes root, alisma, and asparagus root. Traditional herb formulas that had significant hypoglycemic activity by these tests included Rehmannia Six Formula (Liuwei Dihuang Tang), Rehmannia Eight Formula (Bawei Dihuang Tang), and Ginseng and Gypsum Combination (Baihu Jia Renshen Tang). The dosages of herbs administered to the mice to obtain the significant hypoglycemic action ranged from 1.25 to 5.0 grams/kg. These dosages are quite high, and it is difficult to translate the effects seen in these diabetes models with these herb dosages to human requirements, but human dosages would be expected to be at the high end of the range normally recommended for treatment of other diseases based on these figures. A summary of Chinese laboratory research on hypoglycemic agents, reported in the books Modern Study and Application of Materia Medica (30) and Pharmacology and Applications of Chinese Materia Medica (13) yielded the following listing of herbs. Only the commonly used items are included here; there were also a small number of additional herbs that showed positive effect but are not included repeatedly in prescriptions mentioned in the published clinical trials. Note that most of the materials are roots and rhizomes and many of the herbs contain saponins or their aglycones, triterpenoids.
CLINICAL APPLICATIONSClinical trials of Chinese herbs for diabetes have been conducted with increasing frequency over the past thirty years. At the 9th Symposium of Oriental Medicine in 1975, Dr. Takahide Kuwaki reported on partial success in treating 15 diabetes patients with traditional herb formulas; nine of the patients treated (duration of using herbs ranged from 2 to 36 months) showed notable improvements (6). In Beijing, a Diabetes Unit was established in 1975 at the Department of Traditional Chinese Medicine at the Capital Hospital; a summary of their recommendations has been published in America, giving an opportunity for Western practitioners to provide similar treatments to their patients (14). In Changchun, the Kuancheng Institute of Diabetes was established; in 1989 researchers there published results of a highly successful clinical trial of herbs used for treating diabetic ketonuria, in which 28 of 33 patients showed marked improvements after consuming a complex formula comprised almost entirely of herbs that individually have hypoglycemic actions (15). These Chinese clinics, and other facilities in China and Japan, have provided herbal treatments to thousands of patients with diabetes, and the results have often been monitored and reported. Examples of clinical recommendations and evaluative trials for the treatment of diabetes are presented in the book Modern Clinic Necessities for Traditional Chinese Medicine (17). The formulas that had been shown to have hypoglycemic effects in the animal studies, Rehmannia Six Formula and Ginseng and Gypsum Combination, were recommended to treat those who have normal insulin secretion but suffer from diabetes (this would be type 2, or insulin-independent diabetes). These formulas are for the common qi and yin deficiency syndrome found in early stage of clinical symptoms. A traditional variation of Rehmannia Six Formula was also suggested, made by adding anemarrhena and phellodendron (to form Zhi Bai Dihuang Wan). Reducing Sugar Tablet A (Jiang Tang Jia Pian), comprised of astragalus, polygonatum, trichosanthes root, pseudostellaria, and rehmannia, was recommended for those with low levels of insulin, but who are still capable of producing insulin. The herbs were administered as extracts in tablet form, with 2.3 grams raw material per tablet, 6 tablets each time, three times daily, for a total dose of over 40 grams per day (raw materials equivalent). The effects were said to be enhancing sugar tolerance and elevating the level of serum insulin. In the treatment of 405 cases of diabetes with this preparation at the Guanganmen Hospital, 76.5% of the patients had improved sugar tolerance. Among those patients who most closely fit the therapeutic pattern of the herbs-those with qi and yin deficiency-the effective rate was slightly higher, 81%. Rehmannia Eight Formula was recommended for those patients who produced little or no insulin. This is for patients with advanced disease, representing a deficiency of yin and yang (the cinnamon bark and aconite added to Rehmannia Six Formula to produce Rehmannia Eight Formula are said to restore yang). In laboratory animal studies, use of this formula resulted in reduction of water demand (thirst), blood sugar, and sugar spill into the urine. Jade Spring Pill (Yu Quan Wan), a patent formula from China, is recommended for diabetes treatment in the dosage of 50 grams per day (the original form was large honey pills of about 6 grams each), for at least one month. In laboratory animal studies, this formula was shown to increase glycogen in liver cells. The Sichuan Province United Pharmaceutical Manufactory, developed a second generation of Jade Spring Pills comprised of pueraria, trichosanthes root, rehmannia, licorice, schizandra, and other herbs not mentioned on the label. These pills are indicated in the package labeling for the "ill function of the islets of Langerhans." The relatively small pills are packed into small bottles with a total of 6 grams each, and 20 bottles are packed in one box, accompanied by instructions to take one bottle each time, four times daily (the box is a five day supply at 24 grams/day). Compared to the first generation, it is said on the package insert, the new product had been clinically proved to have an improved rate of cure and that the dose had been reduced. Jade Spring Pill is useful for the early stage of diabetes, when yin deficiency and dryness dominate. In a recent clinical evaluation of a Chinese herb formula for diabetes, Jade Spring Pills, used for the control group, was reported to be effective in reducing blood sugar for 79% of cases treated (33). Several clinical trials have been reported in Chinese medical journals with brief English summaries appearing in Abstracts of Chinese Medicine (a Hong Kong publication produced from 1986-1996). A representative report is one that originally appeared in the Journal of the Zhejiang Traditional Chinese Medical College in 1989 (18). Patients were treated with a decoction containing astragalus, codonopsis, rehmannia, gypsum, salvia, persica, carthamus, red atractylodes, anemarrhena, and tang-kuei. This combination of qi and yin tonics plus blood vitalizing herbs is appropriate to treating patients with a middle stage disease showing some secondary symptoms. Modifications of the formula would also be made for the specific symptoms. The patients showed a variety of secondary manifestations of the disease, including nephropathy, peripheral neuropathy, dermatological disorders, retinitis, and liver cirrhosis. Among 19 non-insulin dependent cases treated, fasting blood glucose levels decreased from the pretreatment range of 160-300 mg% to 80-110 mg%. One patient with insulin-dependent diabetes showed a decline in fasting blood sugar from 500 mg% before treatment to readings of 110-200 mg% after treatment. Generally, it was found that blood glucose decreased after 1-2 weeks of treatment and became steady after one month, and the blood glucose changes were followed by symptomatic improvements. A new patent formulation developed by the Chengdu University of Traditional Chinese Medicine and Pharmacology is made comprised of Gui Shao Dihuang Wan (Rehmannia Six Formula with tang-kuei and red peony) with added morus leaf, litchi seed, and coptis. The latter three herbs were recently demonstrated to be effective in lowering blood sugar (34, 35, 36). DIFFERENTIAL THERAPYAlthough certain herbs have been identified as having hypoglycemic activity, Chinese physicians prefer using them in a formulation that addresses differential diagnosis rather than relying solely on herbs proven effective in laboratory tests. As an example of how the herbs are used in this context, the following is the strategy outlined by Lu Renhe in the treatment of 865 elderly patients with diabetes (41); the large number of patients allowed highly differentiated diagnostic categories. He first divided the disease into five stages, representing a progression from simple yin deficiency to complete break down of the body systems (note that "impairment" is more severe than deficiency, in that it involves active degradation):
The first four stages were subdivided into a total of 16 syndromes based on the organ systems affected and types of disorders generated by the basic pattern. Within each of these subcategories, the patients could further be grouped according to the severity of manifestation, but this did not influence the choice of herbs to use in treatment. For each pattern, a base formula of 8-12 herbs was presented (see Table below). Among the herbs used in the formulas listed in this table, there is frequent reference to a few that are known as hypoglycemic agents. These are (number of formulas that include each herb in parentheses):
Aside from these herbs, some herbs were used with less frequency, but commonly relied upon for certain syndromes:
In the case of rhubarb-containing formulas, the rhubarb would be included only so long as constipation remains a problem; after that, it could be removed. Differential Treatment of Diabetes by Stage and Syndrome
DOSAGE AND FORM OF ADMINISTRATIONThe dosage of herbs applied to treatment of diabetes is often quite high. As revealed by the experience with Reducing Sugar Tablet A and Jade Spring Pills, a formula that is considered highly effective must be taken in dosages of about 12-24 grams per day even when presented as a highly condensed extract (made from about 40-80 grams of crude herbs) in convenient form. This apparent requirement is reflected in several books that recommend herbs in decoction form. In the book Clinical Experiences (19), a number of different decoctions are suggested. The dosages of the formulas range from that of an "experiential prescription" containing three herbs (astragalus, rehmannia, and dioscorea, 30 grams each in decoction) at a total dose of 90 grams per day, to a dozen herbs in each of three formulas for yin deficiency syndrome (each prescription contains rehmannia, ophiopogon, and scrophularia), with about 120-150 grams for one day. There is also presented in this book a modified Rehmannia Eight Formula for advanced cases showing yang deficiency, with about 170 gram per day dosage. Added to Rehmannia Eight Formula are the anti-diabetes herbs trichosanthes root, pueraria, salvia, and atractylodes. Regarding efficacy, it is stated that the early-onset type of diabetes responds poorly, but the insulin-independent type with slow onset responds favorably. In the book 100 Famous and Effective Prescriptions of Ancient and Modern Times (20), the Decoction for Diabetes (Yi Tang Tang) is mentioned. It contains rehmannia, trichosanthes root, dioscorea, gypsum, ophiopogon, dendrobium, and seven other herbs. Taken as a decoction, the standard formula is made with 226 grams of herbs for a daily dose. This formula is usually prescribed with additional herbs to address specific symptoms, so that the total daily dosage often reaches 250 grams. In a study with 215 diabetic patients, it was reported that 62 cases were relieved of thirst, overeating, polyuria, and sugar in the urine; the fasting blood glucose declined to below 130 mg%. Additionally, 88 others had some degree of improvement (total effective rate: 70%). In the book Integrating Chinese and Western Medicine (21), four herb formulas are described: each of the formulas, a two day supply of herbs, is made with over 250 grams of herb materials (thus, over 125 grams/day). All four formulas contain twelve to thirteen herbs, and they all include pueraria, rehmannia, and salvia. Nothing is said directly about the degree of effectiveness of the formulas, but the text ends with the comment that certain pills "are also very effective," citing Rehmannia Six Formula, Jade Spring Pills, and Diabetes Pills (Xiao Ke Wan). In A Clinical Guide to Chinese Herbs and Formulas (22), three formulas for diabetes are presented. The formulas are comprised of typical hypoglycemic herbs as mentioned above, and the dosage is usually 10-15 grams of each major ingredient, with 6-7 major ingredients, and a total dosage of about 100 grams per day. The formulas can be modified for specific symptoms, which might add about 10 to 30 grams of herbs. The large amount of raw materials apparently needed for treating diabetes may be a reflection of the need to consume several hundred milligrams of mixed non-toxic active components (e.g., flavonoids, saponins, alkaloids, iridoids, anthraquinones) derived from herbs to attain substantial physiological improvements within a typical treatment period of three months or less. It is expected that most of the anti-diabetic active constituents are present at a level of approximately 2% (or less) of the dried herb material. Decoctions that have 90-150 grams of materials (or more), might yield only about 2 grams of hypoglycemic constituents, perhaps an average of 250 mg of each chemical type. Condensing the active components will yield dried materials that must be taken at a level that is often still regarded as inconvenient by many. For example, dried decoctions (manufactured mainly in Taiwan and Japan) of mixed herbs typically yield a product that is about a 5:1 concentration factor (500 grams of raw materials yields 100 grams of finished product). Such materials are available in the West and often packaged in units of 100 grams. To obtain the equivalent of a dosage of 100 grams of crude herbs in decoction, one would consume about 20 grams of the dried extracts (a one day dose), and a bottle of herbs would be a 5 day supply. This is similar to the dosing for the second generation Jade Spring Pills described above, made of condensed extracts. Attempts have been made to isolate active constituents, as one way of making treatment more convenient, but one then loses several of the purported advantages of whole herbs and formulas. One item of current interest is the alkaloid berberine, which has many therapeutic uses, including treatment of hyperglycemia. Rats treated with alloxan and with berberine were less likely to show blood glucose rise and pathological change in the beta cells. Insulin-independent diabetes patients treated with 300-500 mg of berberine daily for one to three months (along with dietary control), showed definite reduction of blood sugar (23). Berberine is an active component of coptis and phellodendron, used in several diabetes prescriptions. A flavonoid-rich fraction isolated from guava leaves was extracted, made into tablets with 400 mg of the concentrate in each, and administered at a dosage of 6-12 tablets each time, three times daily (total daily dose is 7.2-14.4 grams), to produce hypoglycemic action (17). Flavonoids are active components of many herbs, though not necessarily the key components of most anti-diabetes herbs. Ginseng and its saponins have been studied in alloxan-treated, genetically diabetic, and normal mice (24), revealing a hypoglycemic effect; ginseng saponins also stimulate the production of insulin. In elderly patients with hyperglycemia, the saponins reduced serum glucose (25). Ginseng saponins are typically provided in tablets of 50 mg each, with a dose of 1-2 tablets each time, two to three times per day. Other saponins, such as those in platycodon and the Indian herb gymnemma, have been shown to lower blood sugar, and the dosing appears to be in a range of about 300 mg/day or more. Still, an article in the Journal of Traditional Chinese Medicine (26) suggests that a condensed blend of herbs can be prescribed in moderate dosage. This article described treatment of 102 cases of non-insulin-dependent diabetes, using the Gan Lu Xiao Ke capsule, with rehmannia, codonopsis, astragalus, ophiopogon, asparagus, scrophularia, cornus, tang-kuei, hoelen, alisma, and cuscuta. Patients were treated with the herbs for three months. The group average blood glucose level fell from an initial value of 200 mg% to 154 mg%. The dosage of material in the capsules was only 5.4 grams per day. However, the results were also modest (30% were markedly improved, 57% were improved, but the average blood sugar remained quite high), and patients would receive additional herbs to treat specific symptoms: those herbs, adding to the total dosage, might also contribute to the hypoglycemic action. Another example, was a report about treatment of persons with vascular complications of insulin-independent diabetes (e.g., coronary heart disease, vascular disease of the lower extremities, stroke, retinopathy, etc.). They were treated with a sugar-reducing, pulse-invigorating formula. Unfortunately, the ingredients were not specified other than astragalus and rehmannia; the formula is said to tonify qi, nourish blood, and vitalize blood. The herbs were simply powdered and given in capsules, at a dosage of 2-3 grams each time, three times daily (29). The treatment time was three months, and if the treatment was deemed effective, it would then be continued. Improvements in blood parameters were noted in 82% of the cases that fit the pattern of qi and yin deficiency (which the formula mainly addressed), but only about 63% for other cases (yin deficiency with fire, or yin and yang deficiency; the more advanced cases). Fasting blood sugar was maintained below 150 mg% for 77% of those treated. Further investigation is necessary to determine the minimum formula size (number of ingredients) and the proper dosage of those ingredients, as well as the best form (powdered herbs, extracts, or a combination) to get the desired effects. The use of nutritional supplements (9) and Oriental dietetic practices (10) might add to the benefits of herbal medicine prescriptions, a factor that has not yet been the subject of study. COMBINING DIABETES DRUGS WITH HERBSThere is no evidence that diabetes drugs and Chinese herb therapies are incompatible, but there is a concern that when combining the two, the blood sugar may decline too far. If the herbs are added gradually over a few days with continued monitoring of blood sugar, this problem can be avoided. When herbs successfully contribute to lowering blood sugar, drug dosage may be reduced under a physician's instructions. While Chinese literature sometimes mentions, in passing, the use of Chinese herbs along with modern drugs, specific strategies for combining the two are not commonly presented. A report on integrated Chinese and Western treatment of diabetes was published in 1987 (27). For insulin-dependent diabetics, a formula made with codonopsis, astragalus, atractylodes, rehmannia, ophiopogon, and lycium fruit was given (the formula tonifies qi and nourishes yin). For those with non-insulin-dependent type, they were treated with the same mixture either alone or with tolbutamide or glyburide. The herbs, prepared in liquid form, were given twice daily for three months. It was reported that the herbs exhibited a hypoglycemic effect and synergized with insulin and other drugs. For the group of 53 patients treated, the average fasting blood glucose at the beginning was 177 and at the end of the three months was 135. In another clinical trial (18), a group of 10 patients was identified who had responded poorly to Western drugs and also failed to respond to Chinese herbs. They were then given both the herbs and drugs concurrently. Significant improvements were observed in eight of the ten patients. Further, ginseng is reported to reduce the dosage of insulin needed by patients and to prolong the action of a dose of insulin (13). ACUPUNCTURE FOR DIABETESAcupuncture therapy is a common approach to treating diabetes in China. Many Americans assume that acupuncture is only suitable for treating pain, perhaps because the initial introduction of acupuncture was mainly for this application. Indeed, the general opinion here appears to be that acupuncture ought to be used mainly for treating chronic back pain. Therefore, relatively few people have turned to acupuncture for treating the disease. Increasingly, people with pain and other health problems for which acupuncture is selected also have diabetes. A report in the 1994 Journal of Traditional Chinese Medicine (37) serves as a model of Chinese research on acupuncture. The researchers recruited 60 patients with diabetes and divided them randomly into two groups: the acupuncture group (38 patients) and the control group (22 patients); the two groups were found to be well matched for symptoms and laboratory results (blood and urine tests). Both groups followed a regulated diet during the study, but one group received acupuncture. Electrical stimulation of the needles was used (this method replaces twirling the needle by hand and provides a pulsating stimulus that can be continued for the entire treatment period). Acupuncture was administered once a day for 30 days. The main acupuncture points used were quchi (LI-11), sanyinjiao (SP-6), zusanli (ST-36), and yishu (special diabetes point located at 1.5 cun lateral to the lower border of the spinous process of the 8th thoracic vertebra). Supplemental points include yuji (LU-10), guanyuan (CV-4), and baihui (GV-20). For the control group, a well-known herbal pill, Xiaoke Wan or Diabetes Pill, was administered. This pill had been the subject of earlier study and the level of effectiveness was already established. The patients were not using diabetes drugs during the trial except for 8 patients who required insulin injections. To evaluate the effects of treatment, three levels of responses were defined. Patients who experienced markedly effective results were those who had their initial symptoms essentially disappear by the end of the one month treatment and their fasting blood-sugar levels had dropped below 130 (or the blood sugar two hours after a meal would be below 150). Further, the 24-hour, urine-sugar content was reduced by 30% or more at the end of treatment compared to beginning of treatment. These patients were not "cured" of diabetes but they showed very evident improvements. For those deemed effectively treated (not markedly effective), symptoms were improved but not gone, and fasting blood-sugar levels dropped to below 150 (or two hours after meals below 180), and the 24-hour, urinary-sugar excretion declined by at least 10% from initial values (but not up to 30%). If these standards could not be met, then the treatment was deemed ineffective. All but two of the patients showed declines in blood sugar and urinary sugar excretion and improvements in symptoms. More than one-third of the patients had marked improvement. For the 38 participants in the acupuncture group, there were 25 cases rated markedly effective and 10 cases rated effective: nearly 2/3 of the patients treated showed marked improvement and only three patients failed to respond. Further, it was reported that the patients receiving acupuncture experienced a statistically significant decline in cholesterol, triglycerides, and beta-lipoproteins. The drop in triglycerides was most substantial, with a decline from an average value of 151 at the start to 117 one month later (a decline of more than 20%). There were significant improvements in "nail-fold microcirculation," which is a measurement of blood circulation through capillary beds (poor circulation through these beds is one reason persons with diabetes suffer from skin ulceration), which has also been observed in other diabetes studies (11, 12). Among those who were using insulin, the amount needed after the 30 days of acupuncture declined in six of the eight individuals; in two of those cases, the insulin could be stopped altogether. The objective of the study was to show the benefits of acupuncture, using a common patent pill for the control group. Among the 22 participants who took the diabetes pill, there were 8 cases rated as markedly effective and 12 cases as effective (2 ineffective). In both the acupuncture and herb pill groups, most patients responded well. The authors of the study concluded: "the therapeutic effects of acupuncture on diabetes are similar to those of the diabetes pills, however, acupuncture excels in the prevention of complications, especially cardiovascular diseases." In another study, the acupoint sanyinjiao (SP-6) was used as the primary treatment, with adjunctive points according to syndrome differentiation for 30 patients with diabetes (38). Among the common adjunct points were feishu (BL-13) plus sanjiaoshu (BL-22) for thirst and dryness of the mouth; zusanli (ST-36) for hunger; and taixi (KI-3) plus shenshu (BL-23) for polyuria. Treatment was administered once daily for 12 days as a course of treatment, then a 2-3 day break before starting another course. Needle retention was for 30 minutes following getting the qi sensation. The author noted that the effectiveness of treatment (evaluated as reduction of blood sugar to normal or near normal) was better for younger patients than for older patients and that it generally took 2-3 courses of treatment to get optimal results. He pointed out that diabetes may be due to a combination of deficiency syndrome of qi and yin complexed with blood stasis: "Sanyinjiao is the crossing point of the liver channel, spleen channel, and kidney channel, which has the actions of supplementing qi, nourishing yin, and removing blood stasis. Acupuncture of sanyinjiao can therefore regulate the level of blood sugar in the body." Differentiation of the disease manifestation with corresponding acupuncture for each syndrome was reported by Liu Zhicheng and Sun Fengmin of the Nanjing College of Traditional Chinese Medicine (39). Their treatment patterns are summarized in the table below:
The authors concluded that the best results were attained in younger patients and those with milder disease manifestation. In a review article on acupuncture treatment of diabetes (40), Hu Hui, of the Dongzhimen Hospital of the Beijing TCM University, observed that points are usually selected among back shu points (e.g., the bladder meridian points), front mu points (e.g., the conception vessel points), and limb points (e.g., spleen, stomach, kidney, and liver points). He listed the most commonly used points as: feishu, pishu, shenshu, zusaanli, sanyinjiao, guanyuan, taixi, zhongwan, geshu, yishu, quchi, hegu, shenmen, diji, neiguan, xuangzhong, fuliu, jinjin, yuye, and chengjiang. APPLYING THE ACUPUNCTURE TECHNIQUES HEREIn the U.S., it is uncommon for people to receive acupuncture therapy every day, as is the method used in the clinical studies reported in the Chinese medical journals. Instead, one may undertake a course of therapy with acupuncture once or twice per week. Needless to say, the impact of the intermittent treatment is not as great as with daily acupuncture. However, through the combination of the less frequent acupuncture and the daily ingestion of herbs, one might reasonably expect to accomplish results comparable to those reported in China where the majority of patients get some degree of blood sugar normalization and relief of symptoms. Best results are expected for younger individuals and those who have had diabetes for only a few years. Most acupuncturists in the U.S. have not been called upon to treat many patients with diabetes, mainly because of the misconception that acupuncture is not suitable for that disorder. Nonetheless, acupuncturists are in a position to provide expert treatment because the points to be needled are also used (in various other combinations) for treating other disorders. For example, the acupuncture point zusanli (called Stomach-36; located on the lower leg) is one of the most commonly used points for chronic diseases and is used especially when the disease is obviously affected by dietary factors. All of the acupuncture points listed above have been used in the U.S. and other countries. The needling techniques reported for the diabetes treatments are also essentially the same as used world-wide, without requiring special additional training. REFERENCES
December 2002 |
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|